Poster Session C
Myopathic rheumatic diseases (polymyositis, dermatomyositis, inclusion body myositis)
Session: (1945–1972) Muscle Biology, Myositis & Myopathies – Basic & Clinical Science Poster III
1947: National Incidence, Prevalence & Mortality in Idiopathic Inflammatory Myopathies & Associated Interstitial Lung Disease in England
Tuesday, November 14, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
.png)
James Galloway, MBBS
King's College London
London, United KingdomDisclosure information not submitted.
Abstract Poster Presenter(s)
Jennifer Hannah1, Fiona Pearce2, Myron Odingo2, Megan Rutter2, Jeanette Aston3, Jennifer Lai3, Matthew Grainge2, Sean Mcphail3, Peter Lanyon2, Mary Bythell3, James Galloway4 and Patrick Gordon5, 1King's College London, London, United Kingdom, 2University of Nottingham, Nottingham, United Kingdom, 3National Disease Registration Service, Leeds, United Kingdom, 4King's College London, London, United Kingdom, 5NHS, London, United Kingdom
Background/Purpose: Ethnicity, sex, age & socioeconomic deprivation can all lead to health inequity. Impact of these factors in epidemiology of Idiopathic Inflammatory Myopathies (IIM) has not been widely researched.In collaboration with National Congenital Anomaly & Rare Disease Registration Service (NCARDRS), we described national incidence, prevalence & mortality in IIM and associated Interstitial Lung Disease (IIM-ILD) according to demographics.
Methods: Hospital Episode Statistics (HES) collected at every NHS hospital admission in England, were used to create a national cohort of patients with IIM & IIM-ILD associated ICD-10 codes between 2006-2022. Cases were identified according to pre-validated methods (Hannah, 2022). Age, sex, ethnicity, Index of Multiple Deprivation (IMD) and death certification were collated. Denominator populations were extracted from Office of National Statistics publications. Incidence rates were calculated by multivariate Poisson regression, standardized mortality ratio (SMR) by indirect standardization, and survival analysis by multivariate Cox models. Incidence Rate Ratios (IRR) were mutually adjusted for age, sex & IMD (Ethnicity IRR was not adjusted for IMD due to lack of suitable denominator data). Cox models were adjusted for age, sex, ethnicity, IMD and ILD status.
Results: 14,891 incident IIM cases were identified giving an incidence rate of 1.72/100,000 person-years. Point prevalence was 17.9/100,000 in 2022. Mean age was 59.7 years with incidence peaking at 70-80 years. Multivariate models (Table) showed IIM incidence was higher in females IRR 1.30 (95%CI 1.25, 1.34), but mortality was lower (hazard ratio (HR) 0.78 (95%CI 0.74, 0.82)). Incidence was higher in Asian and Black ethnicities than White (IRR 1.56 and 2.77 respectively). Mortality was higher in White ethnicity (Asian HR 0.80 and Black HR 0.78). The most deprived population quintile had similar incidence IRR 1.06 (95%CI 1.02, 1.11), but higher mortality HR 1.34 (95%CI 1.25, 1.44) than less deprived populations. 17.2% of IIM cases had ILD. IIM-ILD incidence did not vary largely by socioeconomic deprivation, but was substantially higher in Black, Other and Asian populations compared to White (IRR 5.11, 4.07, 2.48). Mortality of IIM-ILD was also lower in Asian HR 0.76 (95%CI 0.61, 0.95) and Black HR 0.73 (95%CI 0.57, 0.93) patients. SMR was 5.13 for IIM and 7.92 for IIM-ILD. Crude mortality increases with age, but standardized mortality is highest in younger patients with ILD. Death certification was available in 7,159 cases. IIM was recognized as a contributory factor in 39%, and ILD in 10.6%. Malignancy was the most reported ‘underlying cause of death’ (24.7%), then cardiovascular disease (19.9%) and respiratory disease (15.8%). Asian and Black ethnicities were less likely to have malignancy mentioned on death certificates (IRR 0.48 and 0.61 respectively).
Conclusion: We have defined national incidence, prevalence and SMR estimates for IIM and IIM-ILD. Incidence is higher in females, Black, Asian and Other ethnicities. Mortality is higher in White ethnicities, increased deprivation and males. Increased mortality in White ethnicities may partially relate to increased malignancy-associated disease.
.jpg)
.jpg)
J. Hannah: None; F. Pearce: Vifor Pharma, 5; M. Odingo: None; M. Rutter: None; J. Aston: None; J. Lai: None; M. Grainge: None; S. Mcphail: None; P. Lanyon: Pfizer, 5; M. Bythell: None; J. Galloway: AbbVie, 2, 5, 6, AstraZeneca, 5, Biogen, 6, Eli Lilly, 2, 5, 6, Galapagos, 2, 5, 6, Janssen, 2, 5, 6, Pfizer, 2, 5, 6, UCB, 2, 5, 6; P. Gordon: Celltrion, 12, Support to attend EULAR conference 2023, Galapagos, 1.
Background/Purpose: Ethnicity, sex, age & socioeconomic deprivation can all lead to health inequity. Impact of these factors in epidemiology of Idiopathic Inflammatory Myopathies (IIM) has not been widely researched.In collaboration with National Congenital Anomaly & Rare Disease Registration Service (NCARDRS), we described national incidence, prevalence & mortality in IIM and associated Interstitial Lung Disease (IIM-ILD) according to demographics.
Methods: Hospital Episode Statistics (HES) collected at every NHS hospital admission in England, were used to create a national cohort of patients with IIM & IIM-ILD associated ICD-10 codes between 2006-2022. Cases were identified according to pre-validated methods (Hannah, 2022). Age, sex, ethnicity, Index of Multiple Deprivation (IMD) and death certification were collated. Denominator populations were extracted from Office of National Statistics publications. Incidence rates were calculated by multivariate Poisson regression, standardized mortality ratio (SMR) by indirect standardization, and survival analysis by multivariate Cox models. Incidence Rate Ratios (IRR) were mutually adjusted for age, sex & IMD (Ethnicity IRR was not adjusted for IMD due to lack of suitable denominator data). Cox models were adjusted for age, sex, ethnicity, IMD and ILD status.
Results: 14,891 incident IIM cases were identified giving an incidence rate of 1.72/100,000 person-years. Point prevalence was 17.9/100,000 in 2022. Mean age was 59.7 years with incidence peaking at 70-80 years. Multivariate models (Table) showed IIM incidence was higher in females IRR 1.30 (95%CI 1.25, 1.34), but mortality was lower (hazard ratio (HR) 0.78 (95%CI 0.74, 0.82)). Incidence was higher in Asian and Black ethnicities than White (IRR 1.56 and 2.77 respectively). Mortality was higher in White ethnicity (Asian HR 0.80 and Black HR 0.78). The most deprived population quintile had similar incidence IRR 1.06 (95%CI 1.02, 1.11), but higher mortality HR 1.34 (95%CI 1.25, 1.44) than less deprived populations. 17.2% of IIM cases had ILD. IIM-ILD incidence did not vary largely by socioeconomic deprivation, but was substantially higher in Black, Other and Asian populations compared to White (IRR 5.11, 4.07, 2.48). Mortality of IIM-ILD was also lower in Asian HR 0.76 (95%CI 0.61, 0.95) and Black HR 0.73 (95%CI 0.57, 0.93) patients. SMR was 5.13 for IIM and 7.92 for IIM-ILD. Crude mortality increases with age, but standardized mortality is highest in younger patients with ILD. Death certification was available in 7,159 cases. IIM was recognized as a contributory factor in 39%, and ILD in 10.6%. Malignancy was the most reported ‘underlying cause of death’ (24.7%), then cardiovascular disease (19.9%) and respiratory disease (15.8%). Asian and Black ethnicities were less likely to have malignancy mentioned on death certificates (IRR 0.48 and 0.61 respectively).
Conclusion: We have defined national incidence, prevalence and SMR estimates for IIM and IIM-ILD. Incidence is higher in females, Black, Asian and Other ethnicities. Mortality is higher in White ethnicities, increased deprivation and males. Increased mortality in White ethnicities may partially relate to increased malignancy-associated disease.
.jpg)
SMR for IIM and subgroup of IIM-ILD compared to the population of England demonstrating increased SMR across all age categories
.jpg)
Incidence Rate Ratios and mortality Hazard Ratio according to demographics. *Incidence rate ratios are adjusted for age, sex and socioeconomic status †Adjusted hazard ratios for age, sex, socioeconomic status, ethnicity and presence of ILD are mutually adjusted.

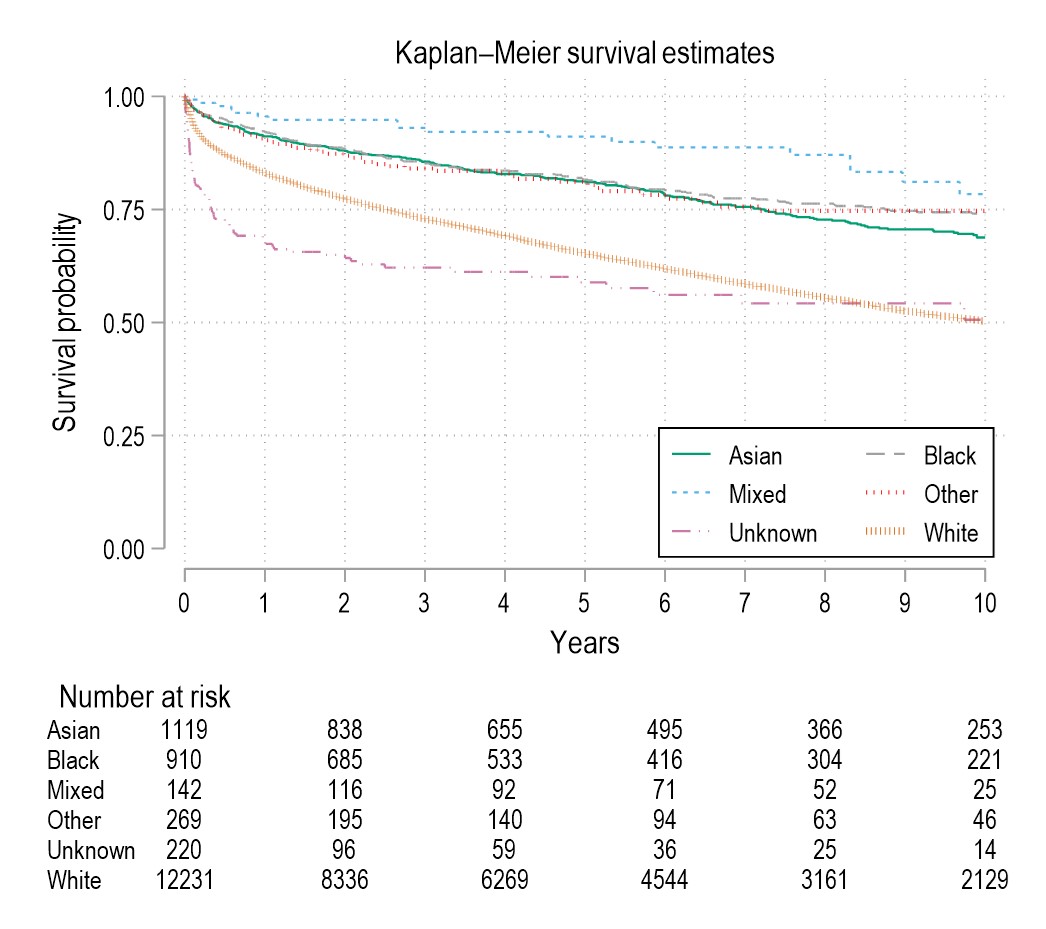
Kaplan-Meier survival curve showing increased mortality in Unknown and White ethnicity categories
J. Hannah: None; F. Pearce: Vifor Pharma, 5; M. Odingo: None; M. Rutter: None; J. Aston: None; J. Lai: None; M. Grainge: None; S. Mcphail: None; P. Lanyon: Pfizer, 5; M. Bythell: None; J. Galloway: AbbVie, 2, 5, 6, AstraZeneca, 5, Biogen, 6, Eli Lilly, 2, 5, 6, Galapagos, 2, 5, 6, Janssen, 2, 5, 6, Pfizer, 2, 5, 6, UCB, 2, 5, 6; P. Gordon: Celltrion, 12, Support to attend EULAR conference 2023, Galapagos, 1.



