Poster Session C
Sjögren’s syndrome
Session: (2177–2194) Sjögren’s Syndrome – Basic & Clinical Science Poster II
2177: Characterization of Crevicular Fluid Microbiota in Primary Sjögren’s Syndrome
Tuesday, November 14, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- GH
Gabriela Hernandez-Molina, MD, MS
Instituto Nacional de Ciencias Medicas y Nutricion
Mexico City, Federal District, MexicoDisclosure information not submitted.
Abstract Poster Presenter(s)
Gabriela Hernandez-Molina1, Alberto Lopez-Reyes2, Carlos Hernandez-Hernandez3, Vanessa Ruiz3, Amaya Llorente-Chavez4, Vanessa Saavedra-González4, Luis llorente4 and Gabriela Martínez-Nava2, 1Department of Immunology and Rheumatology, Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán, Mexico City, Mexico, 2Laboratorio de Gerociencias, Instituto Nacional de Rehabilitación Luis Guillermo Ibarra Ibarra, Mexico City, Mexico, 3Servicio Dental. Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán, Mexico City, Mexico, 4Departamento de Inmunología y Reumatología, Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán, Mexico City, Mexico
Background/Purpose: To describe the taxonomic composition of the microbiota in the crevicular fluid of patients with primary Sjögren's syndrome (PSS), and to assess their association with parotid gland enlargement, periodontal disease, oral quality of life, and anti-Ro/SSA and anti-La/SSB antibodies.
Methods: We included 48 PSS patients according to the ACR/EULAR criteria. We excluded patients with concomitant connective tissue disease, diabetes mellitus, active neoplasia, antibiotic use in the two weeks before the study, or with current active infection. A single rheumatologist registered the following variables: demographics, disease duration, oral/ocular sicca symptoms, parotid enlargement and serology. We evaluated the non-stimulated whole salivary flow (NSWSF). Patients rated the ESSPRI and the Xerostomia-related Quality of Life Scale (XeQoLS). Two experienced periodontists systematically examined six sites per tooth of each patient, to determine the presence of periodontal disease. Crevicular fluid was collected from 6 teeth with the greatest periodontal pocket depth using filter paper (sterile paper points). Samples were immediately frozen at -86 °C until processing. We also included 17 control subjects from the same hospital's Dentistry department matched by gender and age (±5 years). Bacterial DNA was extracted from the crevicular fluid sample using a commercial kit. 16SrRNA V3-V4 region was sequenced using reversible adaptor technology. Sequences were pre-processed and analyzed with QIIME2 and phyloseq software programs. Functionality profiles were predicted using the Tax4Fun2 package.
Results: Most patients were women, the mean age was 52.4 years and the median disease duration was 9.3 years. We found that the microbiota of PSS patients contained more bacteria of the genera Prevotella, Streptococcus, Veillonella, Fusobacterium, and Leptotrichia genera and fewer bacteria of the genus Selenomonas than that of healthy subjects. We also found significant differences in microbiota taxonomy between patients with anti-Ro or anti-La positive antibodies, parotid gland enlargement ( Figure 1) , and periodontal disease severity ( Figure 2) . We found no correlation between microbiota and NSWSF, and oral quality of life. The predicted functional profile showed that the microbiota of PSS patients contained more genes encoding for accessory secretory proteins than healthy controls.
Conclusion: The composition of the crevicular fluid microbiota of PSS patients and healthy subjects differed significantly. Differences were found among patients with parotid gland enlargement as well as anti-Ro and anti-La antibody positivity, suggesting that autoimmunity per se may play an important role in the composition of the oral microbiota in PSS.
G. Hernandez-Molina: None; A. Lopez-Reyes: None; C. Hernandez-Hernandez: None; V. Ruiz: None; A. Llorente-Chavez: None; V. Saavedra-González: None; L. llorente: None; G. Martínez-Nava: None.
Background/Purpose: To describe the taxonomic composition of the microbiota in the crevicular fluid of patients with primary Sjögren's syndrome (PSS), and to assess their association with parotid gland enlargement, periodontal disease, oral quality of life, and anti-Ro/SSA and anti-La/SSB antibodies.
Methods: We included 48 PSS patients according to the ACR/EULAR criteria. We excluded patients with concomitant connective tissue disease, diabetes mellitus, active neoplasia, antibiotic use in the two weeks before the study, or with current active infection. A single rheumatologist registered the following variables: demographics, disease duration, oral/ocular sicca symptoms, parotid enlargement and serology. We evaluated the non-stimulated whole salivary flow (NSWSF). Patients rated the ESSPRI and the Xerostomia-related Quality of Life Scale (XeQoLS). Two experienced periodontists systematically examined six sites per tooth of each patient, to determine the presence of periodontal disease. Crevicular fluid was collected from 6 teeth with the greatest periodontal pocket depth using filter paper (sterile paper points). Samples were immediately frozen at -86 °C until processing. We also included 17 control subjects from the same hospital's Dentistry department matched by gender and age (±5 years). Bacterial DNA was extracted from the crevicular fluid sample using a commercial kit. 16SrRNA V3-V4 region was sequenced using reversible adaptor technology. Sequences were pre-processed and analyzed with QIIME2 and phyloseq software programs. Functionality profiles were predicted using the Tax4Fun2 package.
Results: Most patients were women, the mean age was 52.4 years and the median disease duration was 9.3 years. We found that the microbiota of PSS patients contained more bacteria of the genera Prevotella, Streptococcus, Veillonella, Fusobacterium, and Leptotrichia genera and fewer bacteria of the genus Selenomonas than that of healthy subjects. We also found significant differences in microbiota taxonomy between patients with anti-Ro or anti-La positive antibodies, parotid gland enlargement ( Figure 1) , and periodontal disease severity ( Figure 2) . We found no correlation between microbiota and NSWSF, and oral quality of life. The predicted functional profile showed that the microbiota of PSS patients contained more genes encoding for accessory secretory proteins than healthy controls.
Conclusion: The composition of the crevicular fluid microbiota of PSS patients and healthy subjects differed significantly. Differences were found among patients with parotid gland enlargement as well as anti-Ro and anti-La antibody positivity, suggesting that autoimmunity per se may play an important role in the composition of the oral microbiota in PSS.

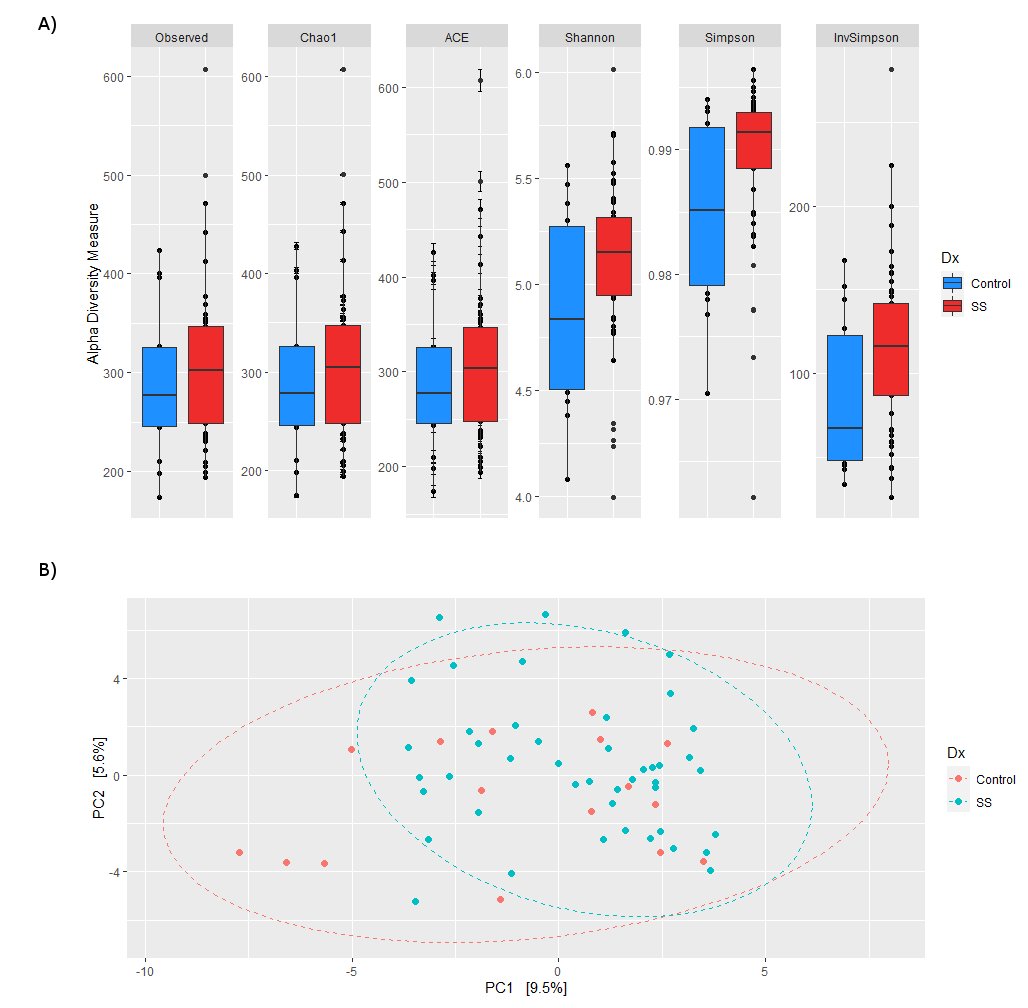
Figure 1 . Alfa diversity indexes stratified by the presence of (A) anti-Ro/SSA, (B) anti-La/SSB, and (C) parotid enlargement; and beta diversity compared between the presence of (D) anti-Ro/SSA , (E) anti-La/SSB, and (F) parotid enlargement.

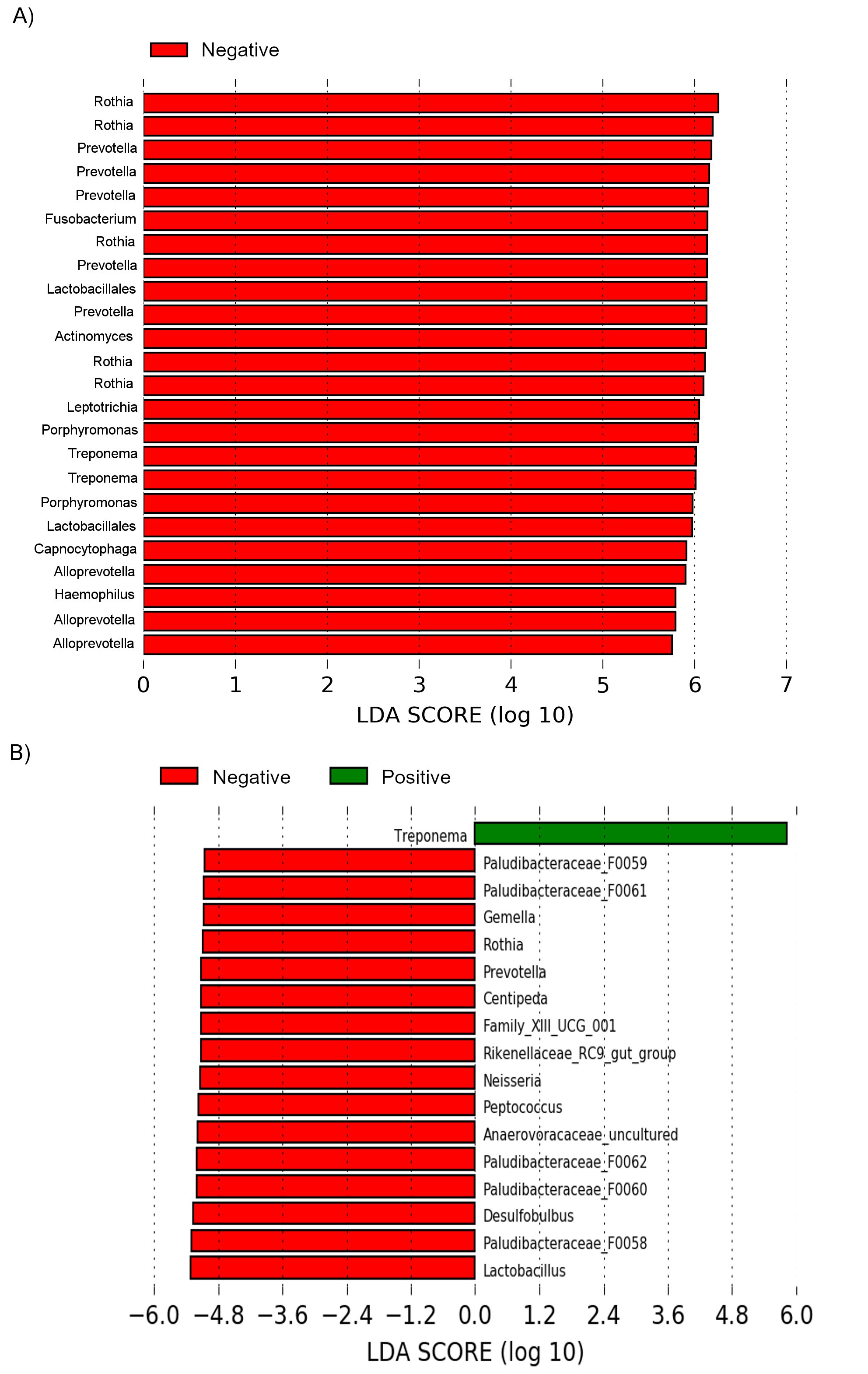
Figure 2 ASVs that best describe the crevicular fluid microbiota of SS patients and healthy controls (A) SS patients negative to anti-Ro/SSA or anti-La/SSB and (B) SS patients with and without parotid enlargement

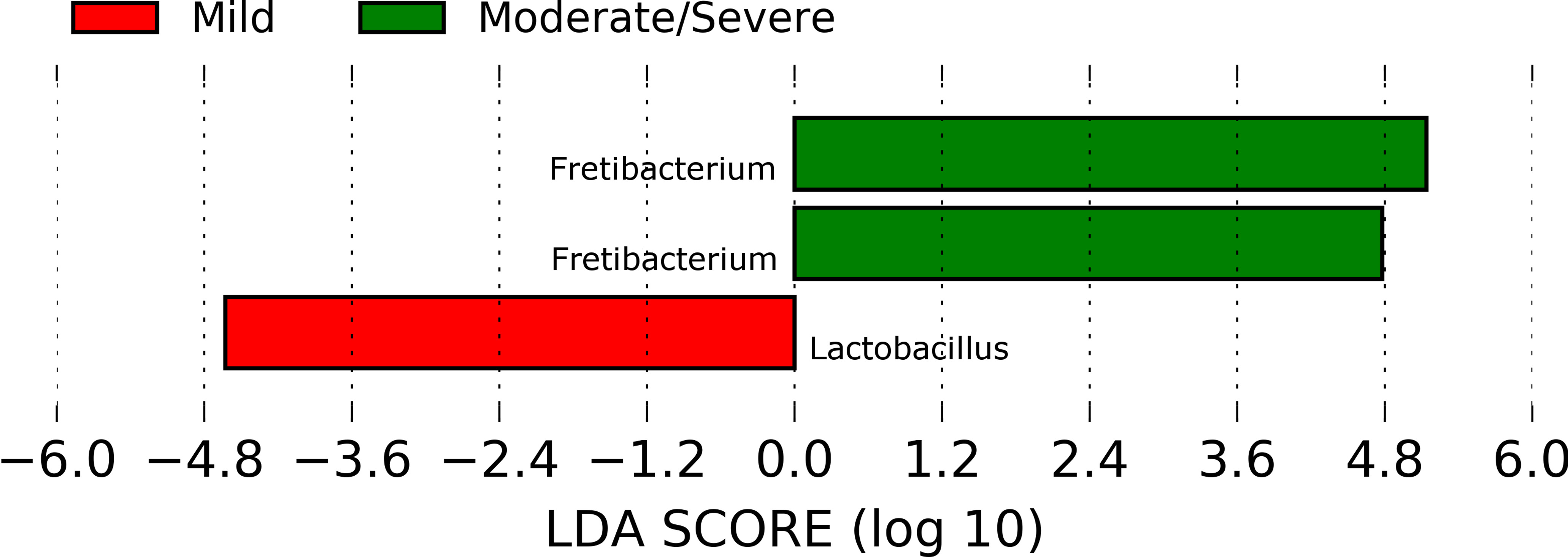
Figure 3 Bacteria genus ASVs whose relative abundance best describe the crevicular fluid microbiota of SS patients with mild and moderate or severe periodontal disease.
G. Hernandez-Molina: None; A. Lopez-Reyes: None; C. Hernandez-Hernandez: None; V. Ruiz: None; A. Llorente-Chavez: None; V. Saavedra-González: None; L. llorente: None; G. Martínez-Nava: None.



