Poster Session C
Epidemiology, health policy and outcomes
Session: (1840–1861) Health Services Research Poster III
1861: Efficacy of Non-pharmacological Interventions: A Systematic Review Informing the 2023 EULAR Recommendations for the Management of Fatigue in People with Inflammatory Rheumatic and Musculoskeletal Diseases
Tuesday, November 14, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- BF
Bayram Farisogullari, MD
Hacettepe University, Faculty of Medicine, Department of Internal Medicine, Division of Rheumatology
Ankara, TurkeyDisclosure information not submitted.
Abstract Poster Presenter(s)
Eduardo Santos1, Bayram Farisogullari2, Emma Dures3, Rinie Geenen4 and Pedro Machado5, 1Health Sciences Research Unit: Nursing (UICISA: E), Nursing School of Coimbra (ESEnfC), Coimbra, Portugal, 2Hacettepe University, Faculty of Medicine, Department of Internal Medicine, Division of Rheumatology, Ankara, Turkey, 3Academic Rheumatology, Bristol Royal Infirmary; and Faculty of Health and Applied Sciences, University of the West of England, Bristol, United Kingdom, 4Utrecht University, Vorstenbosch, Netherlands, 5Centre for Rheumatology & Department of Neuromuscular Diseases, University College London, London, UK. Department of Rheumatology, Northwick Park Hospital, London North West University Healthcare NHS trust, London, UK., London, United Kingdom
Background/Purpose: To identify the best evidence on the efficacy of non-pharmacological interventions in reducing fatigue in people with I-RMDs and to summarise their safety in the identified studies to inform EULAR recommendations for the management of fatigue in people with inflammatory rheumatic and musculoskeletal disease (I-RMD).
Methods: Systematic review of adults with I-RMD conducted according to the Cochrane Handbook. Search strategy ran in Medline, Embase, Cochrane Library, CINAHL Complete, PEDro, OTseeker and PsycINFO. Assessment of risk of bias, data extraction, and synthesis performed by two reviewers independently. Data pooled in statistical meta-analyses.
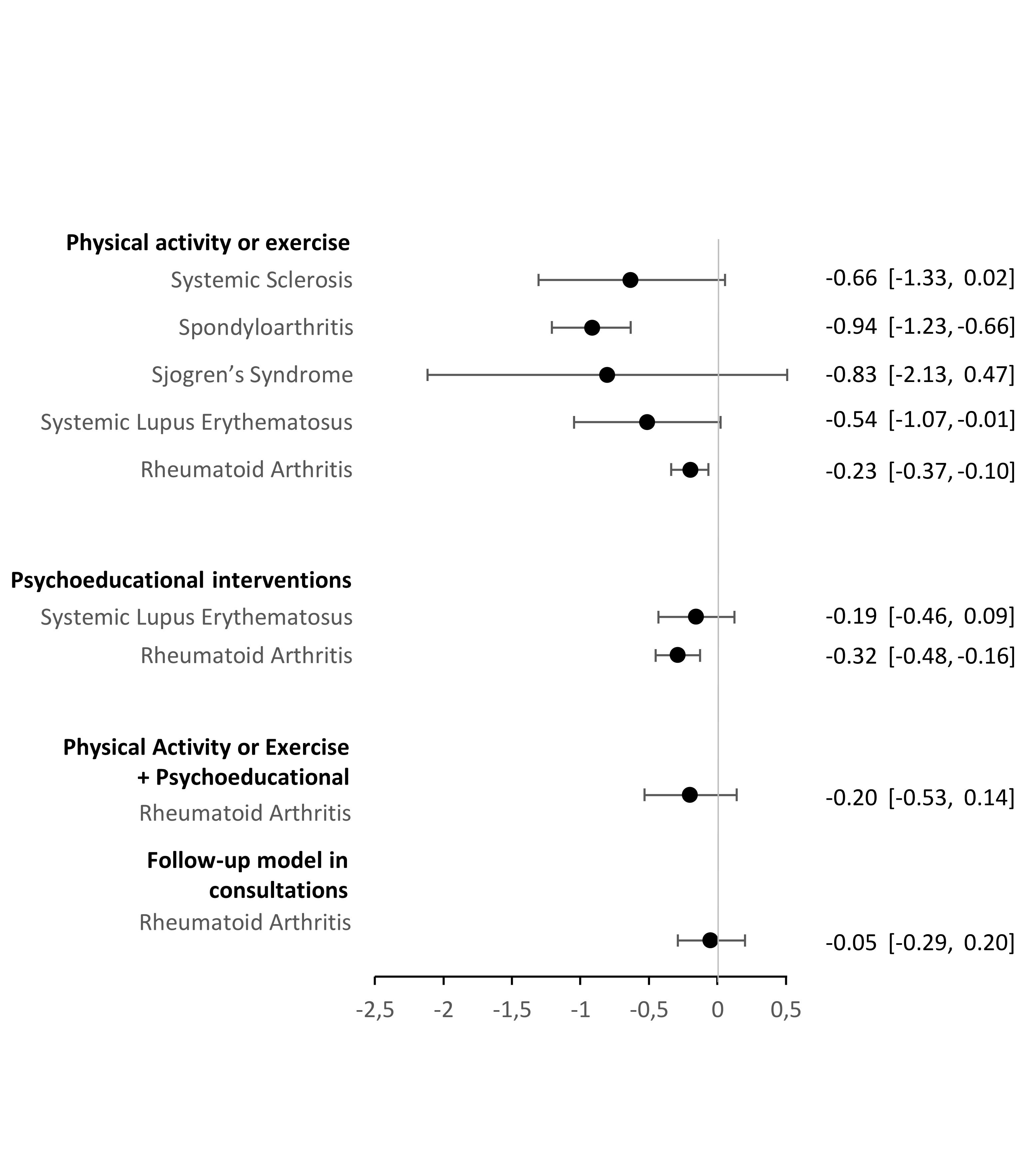
Results: From a total of 4,150 records, 454 were selected for full-text review, 82 fulfilled the inclusion criteria, and 55 RCTs were included in meta-analyses. Physical activity or exercise were efficacious in reducing fatigue in rheumatoid arthritis (RA) (SMD=-0.23, p< 0.001), systemic lupus erythematosus (SLE) (SMD=-0.54, p=0.04) and spondyloarthritis (SpA) (SMD=-0.94, p< 0.001). A reduction in fatigue was also observed in Sjögren's syndrome and systemic sclerosis, although not statistically significant (SMD=-0.83, p=0.21; SMD=-0.66, p=0.06, respectively). Psychoeducational interventions were efficacious in reducing fatigue in RA (SMD=-0.32, p< 0.001), but not in SLE (SMD=-0.19, p=0.18). Follow-up models in consultations and multicomponent interventions reduced fatigue in RA, although the effect was not statistically significant (SMD=-0.05, p=0.71; SMD=-0.20, p=0.24, respectively) (Figure). The narrative results of the RCTs not included in the meta-analysis indicated that several other non-pharmacological interventions were efficacious in reducing fatigue, with reassuring safety results.
Conclusion: Non-pharmacological interventions are efficacious and safe for the management of fatigue in people with I-RMD.
E. Santos: None; B. Farisogullari: None; E. Dures: None; R. Geenen: None; P. Machado: AbbVie/Abbott, 2, 6, Bristol-Myers Squibb(BMS), 2, 6, Celgene, 2, 6, Eli Lilly, 2, 6, Galapagos, 2, 6, Janssen, 2, 6, Merck/MSD, 2, 6, Novartis, 2, 6, Orphazyme, 2, 6, Pfizer, 2, 6, Roche, 2, 6, UCB, 2, 6.
Background/Purpose: To identify the best evidence on the efficacy of non-pharmacological interventions in reducing fatigue in people with I-RMDs and to summarise their safety in the identified studies to inform EULAR recommendations for the management of fatigue in people with inflammatory rheumatic and musculoskeletal disease (I-RMD).
Methods: Systematic review of adults with I-RMD conducted according to the Cochrane Handbook. Search strategy ran in Medline, Embase, Cochrane Library, CINAHL Complete, PEDro, OTseeker and PsycINFO. Assessment of risk of bias, data extraction, and synthesis performed by two reviewers independently. Data pooled in statistical meta-analyses.
Results: From a total of 4,150 records, 454 were selected for full-text review, 82 fulfilled the inclusion criteria, and 55 RCTs were included in meta-analyses. Physical activity or exercise were efficacious in reducing fatigue in rheumatoid arthritis (RA) (SMD=-0.23, p< 0.001), systemic lupus erythematosus (SLE) (SMD=-0.54, p=0.04) and spondyloarthritis (SpA) (SMD=-0.94, p< 0.001). A reduction in fatigue was also observed in Sjögren's syndrome and systemic sclerosis, although not statistically significant (SMD=-0.83, p=0.21; SMD=-0.66, p=0.06, respectively). Psychoeducational interventions were efficacious in reducing fatigue in RA (SMD=-0.32, p< 0.001), but not in SLE (SMD=-0.19, p=0.18). Follow-up models in consultations and multicomponent interventions reduced fatigue in RA, although the effect was not statistically significant (SMD=-0.05, p=0.71; SMD=-0.20, p=0.24, respectively) (Figure). The narrative results of the RCTs not included in the meta-analysis indicated that several other non-pharmacological interventions were efficacious in reducing fatigue, with reassuring safety results.
Conclusion: Non-pharmacological interventions are efficacious and safe for the management of fatigue in people with I-RMD.

E. Santos: None; B. Farisogullari: None; E. Dures: None; R. Geenen: None; P. Machado: AbbVie/Abbott, 2, 6, Bristol-Myers Squibb(BMS), 2, 6, Celgene, 2, 6, Eli Lilly, 2, 6, Galapagos, 2, 6, Janssen, 2, 6, Merck/MSD, 2, 6, Novartis, 2, 6, Orphazyme, 2, 6, Pfizer, 2, 6, Roche, 2, 6, UCB, 2, 6.



