Poster Session C
Systemic lupus erythematosus (SLE)
Session: (2257–2325) SLE – Diagnosis, Manifestations, & Outcomes Poster III
2275: Lupus Low Disease Activity State Ameliorates the Poor Prognosis in Lupus Nephritis Patients with anti-Sm Autoantibody
Tuesday, November 14, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- CC
Chiu Wai Shirley Chan, MBBS
Division of Rheumatology and Clinial Immunology, Department of Medicine, the University of Hong Kong
Hong Kong, Hong Kong, ChinaDisclosure information not submitted.
Abstract Poster Presenter(s)
Chak Kwan Cheung1, Chak Sing Lau2 and Shirley Chiu Wai Chan3, 1Divison of Rheumatology and Clinical Immunology, Queen Mary Hospital, Department of Medicine, the University of Hong Kong, Hong Kong, Hong Kong, 2University of Hong Kong, Division of Rheumatology & Clinical Immunology, Department of Medicine, Queen Mary Hospital, Hong Kong, Hong Kong, 3Divison of Rheumatology and Clinical Immunology, Department of Medicine, Queen Mary Hospital, the University of Hong Kong, Hong Kong, Hong Kong
Background/Purpose:
Anti-Sm autoantibody has been a known specific biomarker of systemic lupus erythematosus (SLE). There have been reports about its correlation with higher disease activity, renal involvement, and lower lupus low disease activity state attainment (LLDAS) among SLE patients. However, its exact role in renal outcome among patients with known lupus nephritis (LN) has been uncertain. This study adds to the literature in the role of Anti-Sm in relation to its prognostic value among patients with lupus nephritis. We also investigate the effect of LLDAS among patients with anti-Sm.
Methods:
Patients with biopsy-proven LN during 2010-2020 were included. Baseline demographics, blood parameters and urinalysis results were recorded. Immunological markers such as autoantibodies profile were also documented. Complete or partial renal response (CRR/PRR) and LLDAS was assessed at 12 months post-LN, and any future relapses were recorded. LLDAS was attained by meeting: (1) SLE Disease Activity Index ≤4 with no major organ activity; (2) no new lupus disease; (3) physician global assessment ≤1; (4) prednisolone dose ≤7.5mg; (5) standard maintenance immunosuppressants. Relapse was a biopsy-proven LN after an initial treatment response of proteinuria reduction of ≥50% to sub-nephrotic range. Predictors of LLDAS and relapse were tested by logistic regression and COX regression respectively.
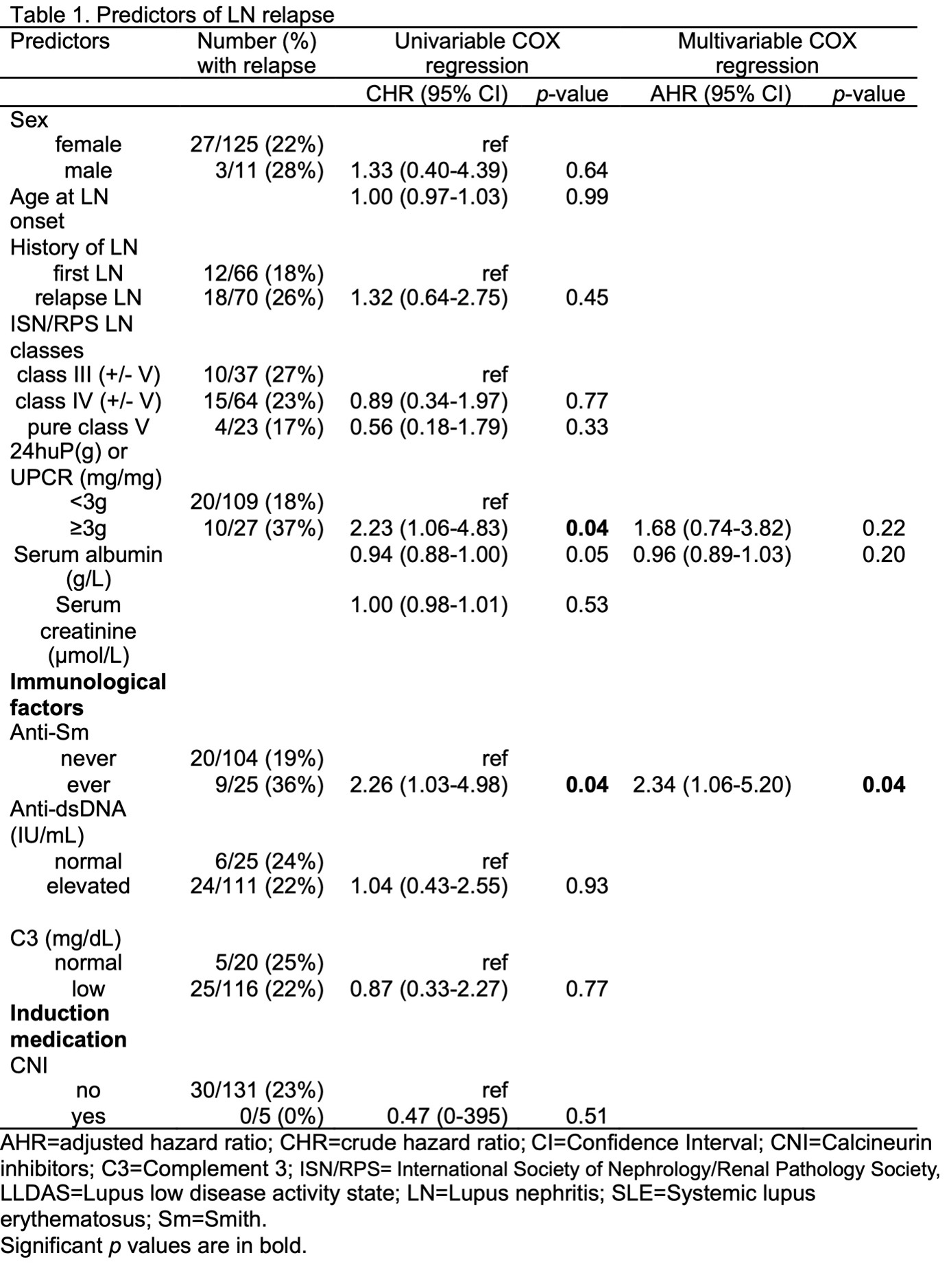
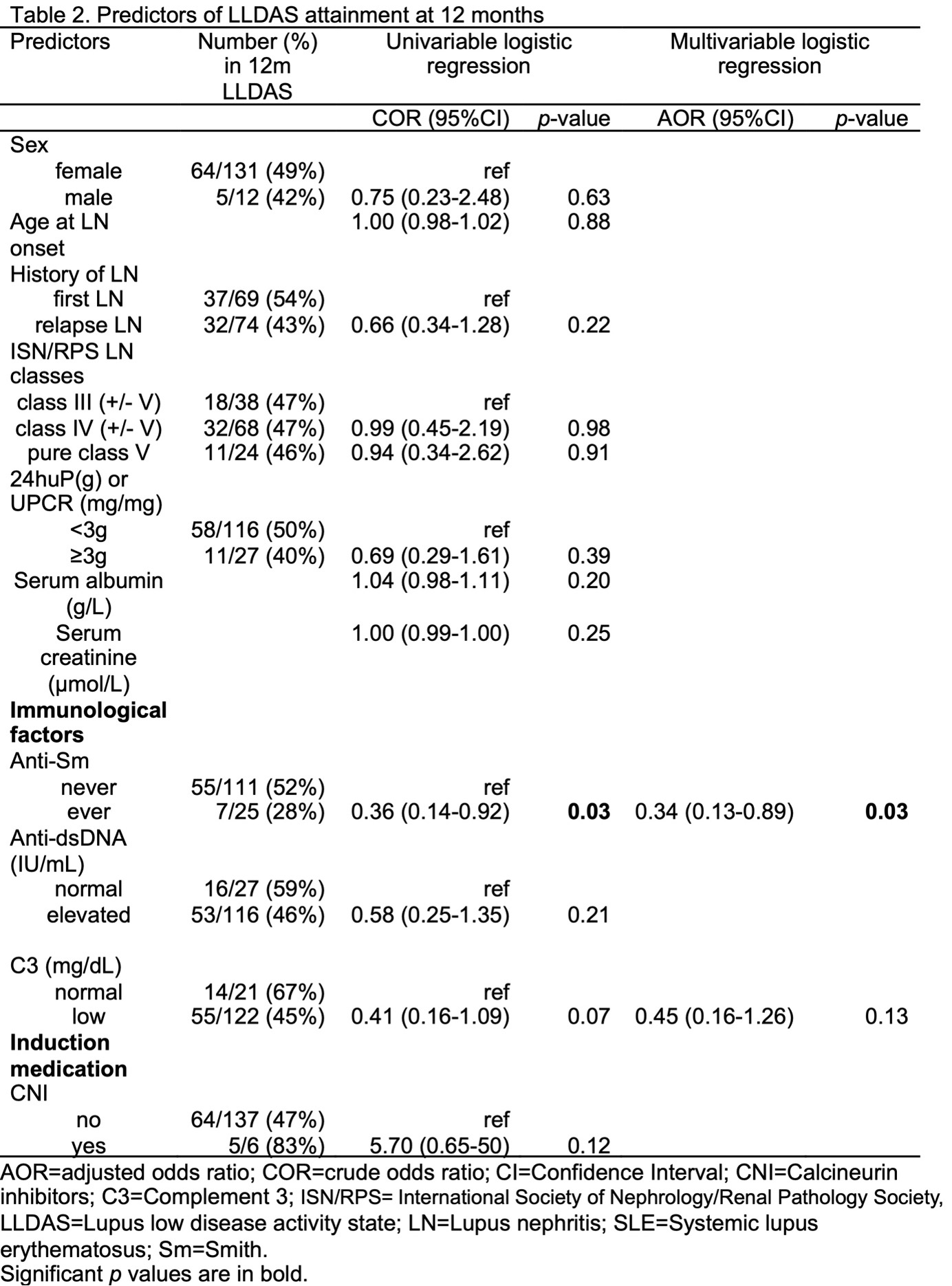
Results: A total 143 patients were included in this study. Anti-Sm positivity was present in 25 patients. Nephrotic range proteinuria and the presence of anti-Sm autoantibody were significant predictors of relapse in the univariable COX model. Only anti-Sm autoantibody was significant (p = 0.04) at the multivariable analysis. Anti-Sm autoantibody was the only variable found to predict LLDAS attainment (p = 0.03). Patients with anti-Sm had lower chance of LLDAS attainment (odds ratio = 0.34) with higher risk of subsequent relapse (hazard ratio = 2.34) compared to anti-Sm negative patients. Despite this, LLDAS attainment complementary to CRR/PRR was still found to be protective from future relapse (p < 0.001).
Conclusion:
Patients with anti-Sm belonged to a high-risk subgroup with worse prognosis, yet LLDAS attainment could still prevent subsequent relapse among them.
C. Cheung: None; C. Lau: AstraZeneca, 6, 12, external expert for SLE sterring committee 11.2022; S. Chan: None.
Background/Purpose:
Anti-Sm autoantibody has been a known specific biomarker of systemic lupus erythematosus (SLE). There have been reports about its correlation with higher disease activity, renal involvement, and lower lupus low disease activity state attainment (LLDAS) among SLE patients. However, its exact role in renal outcome among patients with known lupus nephritis (LN) has been uncertain. This study adds to the literature in the role of Anti-Sm in relation to its prognostic value among patients with lupus nephritis. We also investigate the effect of LLDAS among patients with anti-Sm.
Methods:
Patients with biopsy-proven LN during 2010-2020 were included. Baseline demographics, blood parameters and urinalysis results were recorded. Immunological markers such as autoantibodies profile were also documented. Complete or partial renal response (CRR/PRR) and LLDAS was assessed at 12 months post-LN, and any future relapses were recorded. LLDAS was attained by meeting: (1) SLE Disease Activity Index ≤4 with no major organ activity; (2) no new lupus disease; (3) physician global assessment ≤1; (4) prednisolone dose ≤7.5mg; (5) standard maintenance immunosuppressants. Relapse was a biopsy-proven LN after an initial treatment response of proteinuria reduction of ≥50% to sub-nephrotic range. Predictors of LLDAS and relapse were tested by logistic regression and COX regression respectively.
Results: A total 143 patients were included in this study. Anti-Sm positivity was present in 25 patients. Nephrotic range proteinuria and the presence of anti-Sm autoantibody were significant predictors of relapse in the univariable COX model. Only anti-Sm autoantibody was significant (p = 0.04) at the multivariable analysis. Anti-Sm autoantibody was the only variable found to predict LLDAS attainment (p = 0.03). Patients with anti-Sm had lower chance of LLDAS attainment (odds ratio = 0.34) with higher risk of subsequent relapse (hazard ratio = 2.34) compared to anti-Sm negative patients. Despite this, LLDAS attainment complementary to CRR/PRR was still found to be protective from future relapse (p < 0.001).
Conclusion:
Patients with anti-Sm belonged to a high-risk subgroup with worse prognosis, yet LLDAS attainment could still prevent subsequent relapse among them.

Table 1: Predictors of LN relapse

Table 2: Predictors of LLADAS attainment at 12 months
C. Cheung: None; C. Lau: AstraZeneca, 6, 12, external expert for SLE sterring committee 11.2022; S. Chan: None.



