Poster Session C
Vasculitis
Session: (2387–2424) Vasculitis – Non-ANCA-Associated & Related Disorders Poster III
2404: Subclinical Giant Cell Arteritis in Polimialgia Rheumatica: A Biomarker of High Relapse Risk
Tuesday, November 14, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- ED
Eugenio De Miguel, MD, PhD
Hospital Universitario La Paz
Madrid, SpainDisclosure information not submitted.
Abstract Poster Presenter(s)
Eugenio De Miguel1, Rositsa Karalilova2, PIERLUIGI MACCHIONI3, Cristina Ponte4, Edoardo Conticini5, Alessandro Tomelleri6, Sara Monti7, Irene Monjo1, Zguro Batalov2, Giulia Klinowski8, Paolo Falsetti9, David Kane10, Corrado Campochiaro11 and Alojzija Hocevar12, 1Hospital Universitario La Paz, Madrid, Spain, 2Medical University of Plovdiv, University Hospital Kaspela, Plovdiv, Bulgaria, 3Azienda USL -IRCCS di Reggio Emilia, Reggio Emilia, Italy, 4Department of Rheumatology, Centro Hospitalar Universitário Lisboa Norte, Centro Académico de Medicina de Lisboa, Lisbon, Portugal; Rheumatology Research Unit, Instituto de Medicina Molecular, Faculdade de Medicina, Universidade de Lisboa, Centro Académico de Medicina de Lisboa, Lisbon, Portugal, 5Tallaght University Hospital, Dublin, Ireland, 6Unit of Immunology, Rheumatology, Allergy and Rare Diseases, San Raffaele Scientific Institute, Milano, Italy, 7Division of Rheumatology, Fondazione IRCCS Policlinico San Matteo, Pavia, Italy; Department of Internal Medicine and Therapeutics, Università di Pavia, Pavia, Italy, 8IRCCS-S.Maria Nuova, Reggio Emilia, Italy, 9San Raffaele Scientific Institute, Siena, Italy, 10Tallaght University Hospital & Trinity College Dublin, Dublin, Ireland, 11IRCCS San Raffaele Hospital, Unit of Immunology, Rheumatology, Allergy and Rare Disease. Vita-Salute San Raffaele University, Milan, Italy, 12Department of Rheumatology, Universitiy Medical Centre Ljubljana, Ljubljana, Slovenia
Background/Purpose: Around 20% of polymyalgia rheumatica (PMR) patients without clinical symptoms of giant cell arteritis (GCA) have subclinical GCA by image or byopsy1. However, there is not data about its natural evolution and how these patients should be treated.Our main objective was to compare the outcomes of patients with PMR and subclinical GCA with those with isolated PMR over a 2-year period.
Methods: We included PMR patients with a complete vascular ultrasound examination at basal visit, recruited from nine European rheumatology centers. We analyzed longitudinal data from baseline, 3, 6, 12, 18 and 24 months. Only patients followed for at least one year were included. All patients fulfilled the 2012 EULAR/ACR Provisional Classification Criteria for PMR. Patients were stratified into two groups: isolated PMR and PMR with subclinical GCA with ultrasound positive halo sign. The outcomes (relapses, prednisone use and treatments needed) were compared between groups, using Chi2, student t test and logistic regression analysis. PMR relapse was defined as clinical and/or laboratory worsening after initial remission requiring change in treatment after excluding other causes. Relapses were classified as minor or major according to the EULAR definition2.
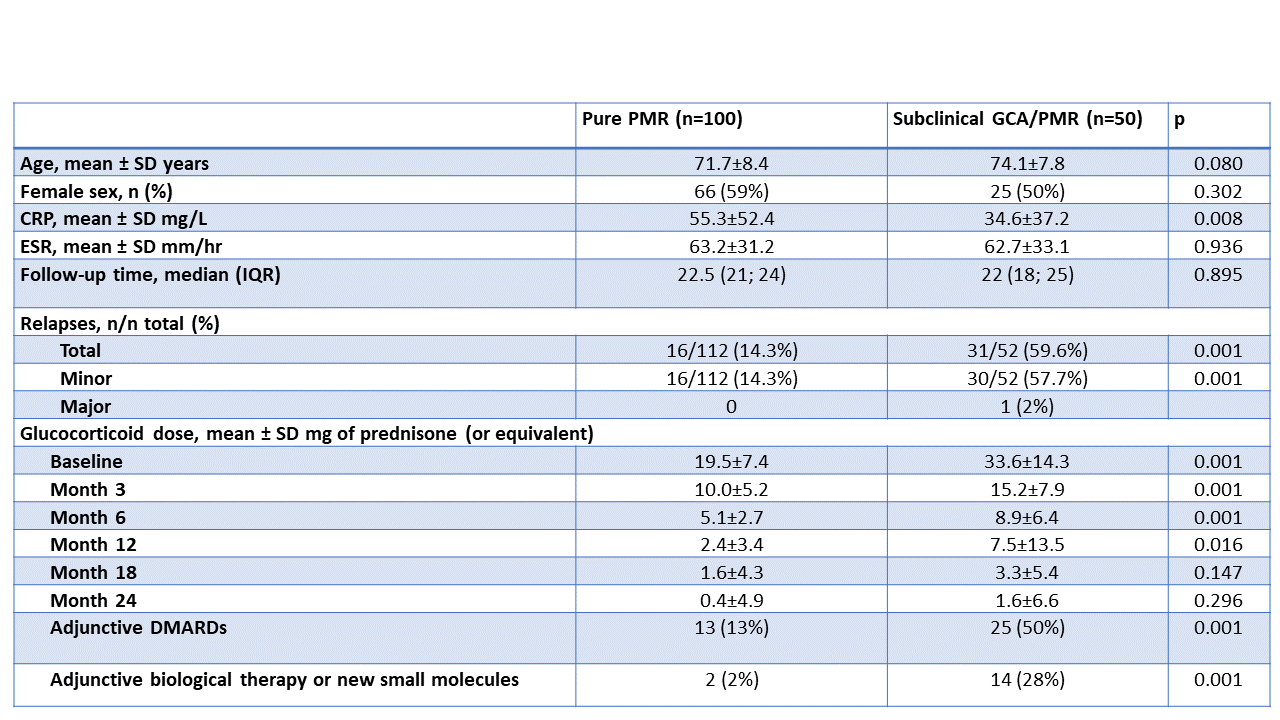
Results: We included 150 PMR patients (50 with subclinical GCA, 100 withisolated PMR) with a median (IQR) follow-up of 22 (20; 24) months without significant differences betweenisolated PMR and subclinical GCA. 47 patients (29%) had a relapse, 31 (62%) in the PMR with subclinical GCA group and 16 (14.3%)in the isolated PMR group (p< 0.001).In patients with pure PMR all relapses were minor, whereas in patients with subclinical GCA there was one major relapse. Prednisone starting dose was significantly higher in patients with PMR with subclinical GCA than in patients with isolated PMR (Table 1). Among patients with subclinical GCA, no differences were found in the prednisone starting dose between those who relapsed and those who did not (mean, 32.4±15.6 vs 35.5±12.1 mg, p=0.722). Patients who relapsed had a faster prednisone dose reduction in the first 3 months in compared to the non-relapsing patients (mean dose at 3 months, 13.0±7.4 vs 18.8±7.5 mg, p< 0.01). Five patients in the PMR with subclinical GCA group received tozilizumab therapy at diagnosis; one of them had a minor relapse. No differences were found between relapsing and non-relapsing patients with subclinical GCA regarding age, sex, CPR and ESR.
Conclusion: Patients with PMR and subclinical GCA had a significantly higher number of relapses during a 24-month follow-up than patients with isolated PMR (62 vs 16%). Our results suggest that patients with PMR with subclinical GCA should be treated in the same manner as patients with clinically overt GCA without ischemic symptoms.
References. 1 De Miguel et al.Prevalence and characteristics of subclinical giant cell arteritis in polymyalgia rheumatica. Rheumatology (Oxford). 2023 May 2:kead189. doi: 10.1093/rheumatology/kead189. Online ahead of print. 2 Hellmich B et al. 2018 Update of the EULAR recommendations for the management of large vessel vasculitis. Ann Rheum Dis. 2020 Jan;79:19-30. Acknowledgements:To the GCA/PMR study group
E. De Miguel: None; R. Karalilova: None; P. MACCHIONI: None; C. Ponte: None; E. Conticini: None; A. Tomelleri: Novartis, 1; S. Monti: CSL Vifor, 6; I. Monjo: None; Z. Batalov: None; G. Klinowski: None; P. Falsetti: None; D. Kane: None; C. Campochiaro: Boehringer Ingelheim, 1, 6, Janssen, 1, 6, Novartis, 1, 6; A. Hocevar: None.
Background/Purpose: Around 20% of polymyalgia rheumatica (PMR) patients without clinical symptoms of giant cell arteritis (GCA) have subclinical GCA by image or byopsy1. However, there is not data about its natural evolution and how these patients should be treated.Our main objective was to compare the outcomes of patients with PMR and subclinical GCA with those with isolated PMR over a 2-year period.
Methods: We included PMR patients with a complete vascular ultrasound examination at basal visit, recruited from nine European rheumatology centers. We analyzed longitudinal data from baseline, 3, 6, 12, 18 and 24 months. Only patients followed for at least one year were included. All patients fulfilled the 2012 EULAR/ACR Provisional Classification Criteria for PMR. Patients were stratified into two groups: isolated PMR and PMR with subclinical GCA with ultrasound positive halo sign. The outcomes (relapses, prednisone use and treatments needed) were compared between groups, using Chi2, student t test and logistic regression analysis. PMR relapse was defined as clinical and/or laboratory worsening after initial remission requiring change in treatment after excluding other causes. Relapses were classified as minor or major according to the EULAR definition2.
Results: We included 150 PMR patients (50 with subclinical GCA, 100 withisolated PMR) with a median (IQR) follow-up of 22 (20; 24) months without significant differences betweenisolated PMR and subclinical GCA. 47 patients (29%) had a relapse, 31 (62%) in the PMR with subclinical GCA group and 16 (14.3%)in the isolated PMR group (p< 0.001).In patients with pure PMR all relapses were minor, whereas in patients with subclinical GCA there was one major relapse. Prednisone starting dose was significantly higher in patients with PMR with subclinical GCA than in patients with isolated PMR (Table 1). Among patients with subclinical GCA, no differences were found in the prednisone starting dose between those who relapsed and those who did not (mean, 32.4±15.6 vs 35.5±12.1 mg, p=0.722). Patients who relapsed had a faster prednisone dose reduction in the first 3 months in compared to the non-relapsing patients (mean dose at 3 months, 13.0±7.4 vs 18.8±7.5 mg, p< 0.01). Five patients in the PMR with subclinical GCA group received tozilizumab therapy at diagnosis; one of them had a minor relapse. No differences were found between relapsing and non-relapsing patients with subclinical GCA regarding age, sex, CPR and ESR.
Conclusion: Patients with PMR and subclinical GCA had a significantly higher number of relapses during a 24-month follow-up than patients with isolated PMR (62 vs 16%). Our results suggest that patients with PMR with subclinical GCA should be treated in the same manner as patients with clinically overt GCA without ischemic symptoms.
References. 1 De Miguel et al.Prevalence and characteristics of subclinical giant cell arteritis in polymyalgia rheumatica. Rheumatology (Oxford). 2023 May 2:kead189. doi: 10.1093/rheumatology/kead189. Online ahead of print. 2 Hellmich B et al. 2018 Update of the EULAR recommendations for the management of large vessel vasculitis. Ann Rheum Dis. 2020 Jan;79:19-30. Acknowledgements:To the GCA/PMR study group

E. De Miguel: None; R. Karalilova: None; P. MACCHIONI: None; C. Ponte: None; E. Conticini: None; A. Tomelleri: Novartis, 1; S. Monti: CSL Vifor, 6; I. Monjo: None; Z. Batalov: None; G. Klinowski: None; P. Falsetti: None; D. Kane: None; C. Campochiaro: Boehringer Ingelheim, 1, 6, Janssen, 1, 6, Novartis, 1, 6; A. Hocevar: None.



