Poster Session C
Myopathic rheumatic diseases (polymyositis, dermatomyositis, inclusion body myositis)
Session: (1945–1972) Muscle Biology, Myositis & Myopathies – Basic & Clinical Science Poster III
1957: Non-Linear Mendelian Randomization Analyses Support a Role for Low Vitamin D Status in Sarcopenia Risk
Tuesday, November 14, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- TS
Tingting Sha, PhD
Hunan Key Laboratory of Joint Degeneration and Injury
Changsha, ChinaDisclosure information not submitted.
Abstract Poster Presenter(s)
Tingting Sha1, Yilun Wang2, Yuqing Zhang3, Nancy Lane4, Changjun Li5, Jie Wei6, Chao Zeng2 and Guanghua Lei2, 1Hunan Key Laboratory of Joint Degeneration and Injury, Changsha, China, 2Department of Orthopaedics, Xiangya Hospital, Central South University, Changsha, China, 3Division of Rheumatology, Allergy, and Immunology, Department of Medicine, Massachusetts General Hospital, Boston, MA, 4University of California, Hillsborough, CA, 5National Clinical Research Center for Geriatric Disorders, Xiangya Hospital, Central South University, Changsha, China, 6Health Management Center, Xiangya Hospital Central South University, Changsha, China
Background/Purpose: Vitamin D deficiency is commonly associated with sarcopenia; however, the latest International Clinical Practice Guidelines for Sarcopenia do not recommend vitamin D supplementation for sarcopenia owing to a lack of an apparent therapeutic effect on the indices of sarcopenia among participants with replete vitamin D concentration (i.e., 25[OH]D >50 nmol/L) from randomized controlled trials. While there is consensus in all vitamin D guidelines that serum levels of 25(OH)D < 25 nmol/L should be corrected, approximately 30% of the world population's 25(OH)D levels range from 25 to 50 nmol/L, and it remains unclear whether such suboptimal levels of 25(OH)D can maintain optimal health, including the risk of sarcopenia.
Methods: Among 295,489 participants of unrelated European ancestry from the UK Biobank, we examined the causal association between genetic variants for serum 25(OH)D concentration and the sarcopenia risk. The primary outcome was sarcopenia, defined by the European Working Group on Sarcopenia in Older People. The secondary outcomes consisted of three sarcopenia indices, i.e., grip strength, appendicular lean mass index, and gait speed. We calculated a weighted genetic score using 35 single nucleotide polymorphisms as instrumental variables for serum 25(OH)D concentration and performed non-linear Mendelian randomization to estimate the effect of serum 25(OH)D on sarcopenia risk and its indices.
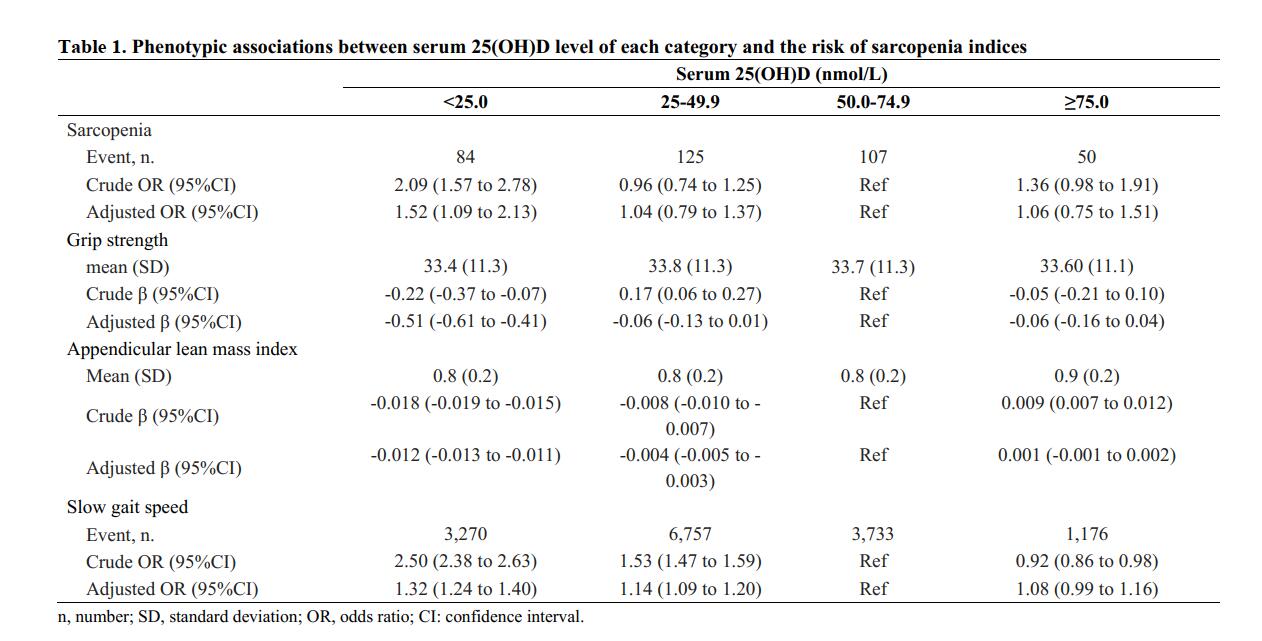
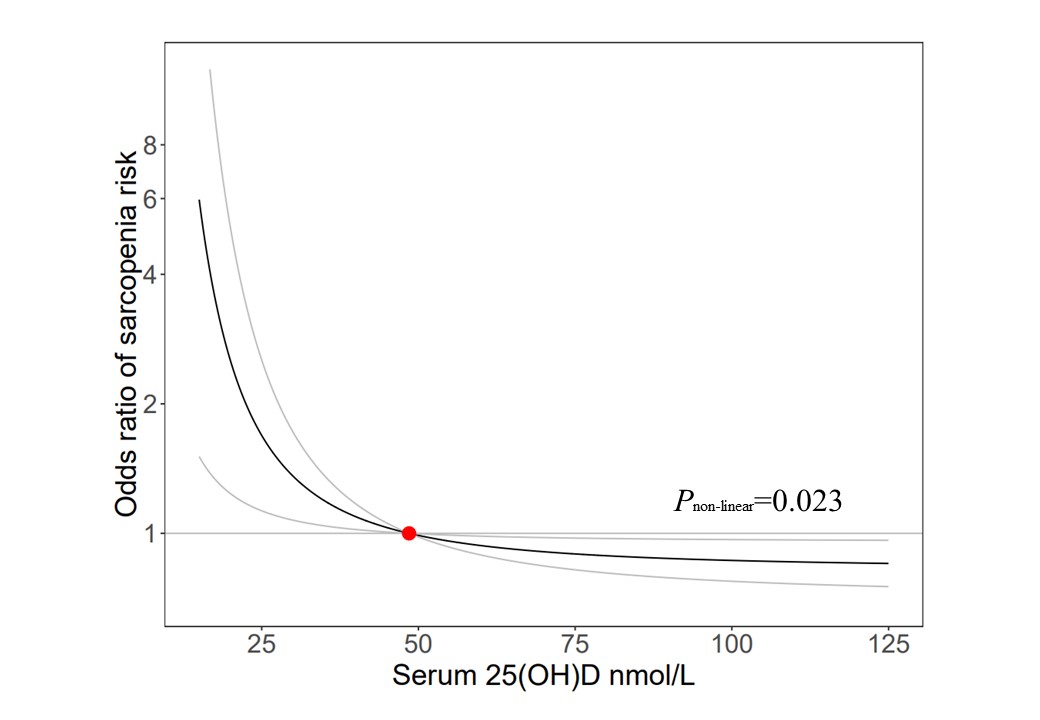
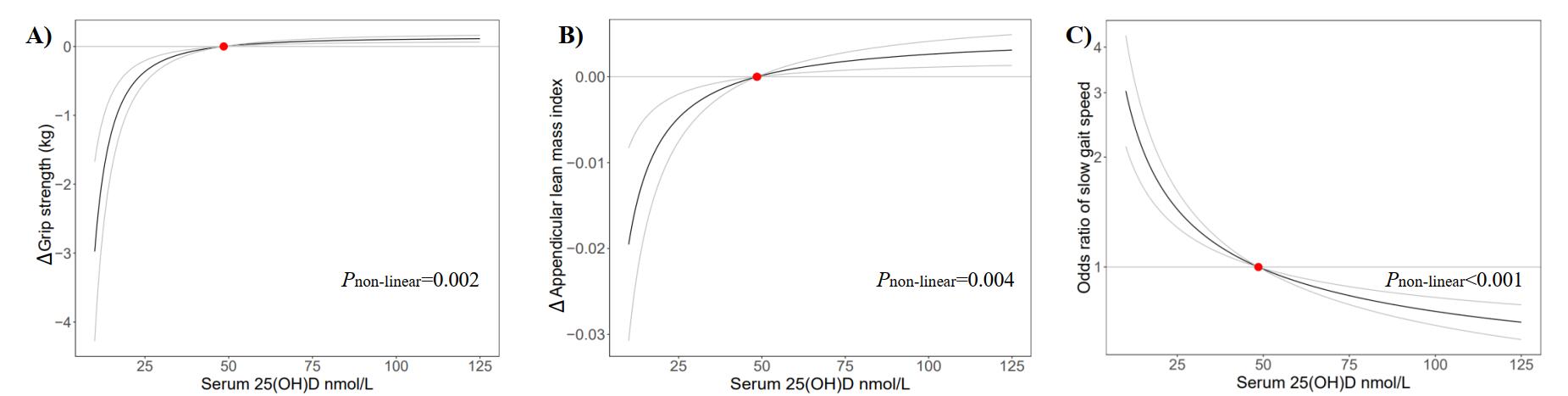
Results: In the phenotypic association analyses, compared with serum 25(OH)D 50-74.9 nmol/L category, serum 25(OH)D levels below 50 nmol/L adjusted for multivariable factors were inversely associated with each of the sarcopenia indices (Table 1). There was an L-shaped (Pnon-linear=0.023) association between genetically predicted serum 25(OH)D concentration and risk of sarcopenia (Fig. 1). The risk of sarcopenia decreased rapidly as serum 25(OH)D concentration increased until 50 nmol/L and then leveled off. The odds ratio of sarcopenia for serum 25(OH)D level of 25 nmol/L vs. 50 nmol/L was 1.69 (95% CI: 1.13 to 2.53). Similar patterns were also observed when the association between serum 25(OH)D concentration and risks of each of the sarcopenia indices were evaluated (Fig. 2).
Conclusion: Our study supports a causal relationship between suboptimal vitamin D levels and sarcopenia risk. These findings suggest that vitamin D supplementation needs to be considered for individuals with suboptimal vitamin D levels to reduce the burden of sarcopenia.
T. Sha: None; Y. Wang: None; Y. Zhang: None; N. Lane: None; C. Li: None; J. Wei: None; C. Zeng: None; G. Lei: None.
Background/Purpose: Vitamin D deficiency is commonly associated with sarcopenia; however, the latest International Clinical Practice Guidelines for Sarcopenia do not recommend vitamin D supplementation for sarcopenia owing to a lack of an apparent therapeutic effect on the indices of sarcopenia among participants with replete vitamin D concentration (i.e., 25[OH]D >50 nmol/L) from randomized controlled trials. While there is consensus in all vitamin D guidelines that serum levels of 25(OH)D < 25 nmol/L should be corrected, approximately 30% of the world population's 25(OH)D levels range from 25 to 50 nmol/L, and it remains unclear whether such suboptimal levels of 25(OH)D can maintain optimal health, including the risk of sarcopenia.
Methods: Among 295,489 participants of unrelated European ancestry from the UK Biobank, we examined the causal association between genetic variants for serum 25(OH)D concentration and the sarcopenia risk. The primary outcome was sarcopenia, defined by the European Working Group on Sarcopenia in Older People. The secondary outcomes consisted of three sarcopenia indices, i.e., grip strength, appendicular lean mass index, and gait speed. We calculated a weighted genetic score using 35 single nucleotide polymorphisms as instrumental variables for serum 25(OH)D concentration and performed non-linear Mendelian randomization to estimate the effect of serum 25(OH)D on sarcopenia risk and its indices.
Results: In the phenotypic association analyses, compared with serum 25(OH)D 50-74.9 nmol/L category, serum 25(OH)D levels below 50 nmol/L adjusted for multivariable factors were inversely associated with each of the sarcopenia indices (Table 1). There was an L-shaped (Pnon-linear=0.023) association between genetically predicted serum 25(OH)D concentration and risk of sarcopenia (Fig. 1). The risk of sarcopenia decreased rapidly as serum 25(OH)D concentration increased until 50 nmol/L and then leveled off. The odds ratio of sarcopenia for serum 25(OH)D level of 25 nmol/L vs. 50 nmol/L was 1.69 (95% CI: 1.13 to 2.53). Similar patterns were also observed when the association between serum 25(OH)D concentration and risks of each of the sarcopenia indices were evaluated (Fig. 2).
Conclusion: Our study supports a causal relationship between suboptimal vitamin D levels and sarcopenia risk. These findings suggest that vitamin D supplementation needs to be considered for individuals with suboptimal vitamin D levels to reduce the burden of sarcopenia.


Figure 1 Genetic association of serum 25(OH)D with risk of sarcopenia using 35 SNPs to the instrument. The red dot represents the reference point of serum 25(OH)D of 50 nmol/L. The gray lines represent the 95% confidence intervals. The adjustment includes age, sex, assessment center, birth location, top 20 genetic principal components, genotyping array in both stages, and nuisance factors, which could affect serum 25(OH)D measurements, including the month in which the blood sample was taken, fasting time before the blood sample was taken, and sample aliquots for measurement.

Figure 2 Genetic association of serum 25(OH)D with indices of sarcopenia using 35 SNPs to the instrument. (A) grip strength, (B) appendicular lean mass index, and (C) slow gait speed. The red dot represents the reference point of serum 25(OH)D of 50 nmol/L. The gray lines represent the 95% confidence intervals. The adjustment includes age, sex, assessment center, birth location, top 20 genetic principal components, genotyping array in both stages, and nuisance factors, which could affect serum 25(OH)D measurements, including the month in which the blood sample was taken, fasting time before the blood sample was taken, and sample aliquots for measurement.
T. Sha: None; Y. Wang: None; Y. Zhang: None; N. Lane: None; C. Li: None; J. Wei: None; C. Zeng: None; G. Lei: None.



