Poster Session B
Epidemiology, health policy and outcomes
Session: (0993–1012) Health Services Research Poster II
0998: Barriers and Facilitators for Osteoporosis and Sarcopenia Care for Persons Living with HIV in Peru: HIV Physician and Coordinator Perspectives
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- RS
Rebecca Slotkin, MD (she/her/hers)
Yale University, Department of Medicine, Section of Rheumatology
New Haven, CT, United StatesDisclosure information not submitted.
Abstract Poster Presenter(s)
Rebecca Slotkin1, Daniel Granda Calderón2, Joselito Malca Hernandez2, Diego Cabrera3, Carlos Manuel Benites Villafane4, Patricia Jannet García5 and Evelyn Hsieh6, 1Yale University, Department of Medicine, Section of Rheumatology; Yale School of Public Health, New Haven, CT, 2Facultad de Medicina Alberto Hurtado de la Universidad Peruana Cayetano Heredia, Lima, Peru, 3Yale University, Department of Medicine, Section of Rheumatology; Department of Internal Medicine, Waterbury Hospital, New Haven, CT, 4Ministerio de Salud, Peru, Lima, Peru, 5Epidemiology, STD, and HIV Unit, School of Public Health, Universidad Peruana Cayetano Heredia, Lima, Peru, 6Yale University, Department of Medicine, Section of Rheumatology; Yale School of Public Health; Section of Rheumatology, VA Connecticut Healthcare System, Westport, CT
Background/Purpose: Persons living with HIV (PLWH) have a higher risk of developing age-related non-communicable diseases (NCDs), such as osteoporosis and sarcopenia. In Peru, HIV providers are the primary point of medical care for PLWH. Using a qualitative approach, we examined health system barriers and facilitators for osteoporosis and sarcopenia care for PLWH in Peru from the perspective of HIV physicians and coordinators.
Methods: HIV regional program coordinators and physicians affiliated with Peru's National HIV, STI and Hepatitis Program were recruited from the Program's physician and coordinator registry and by peer referral. All coordinators (N=31) were contacted for a semi-structured in-depth interview over Zoom by a trained Peruvian research assistant. Physicians were purposefully sampled to ensure adequate regional representation. Interviews continued until thematic saturation was reached in both groups. The interviews were recorded and transcribed using Sonix.ai and checked for accuracy. Transcripts were translated to English following a standardized protocol by a team of bilingual translators, and then coded in English by two independent coders, one of which was Peruvian to ensure culturally appropriate codes. All codes were discussed, and discrepancies were resolved by consensus. The emerging themes and sub-themes were visualized using an adapted socioecological framework.
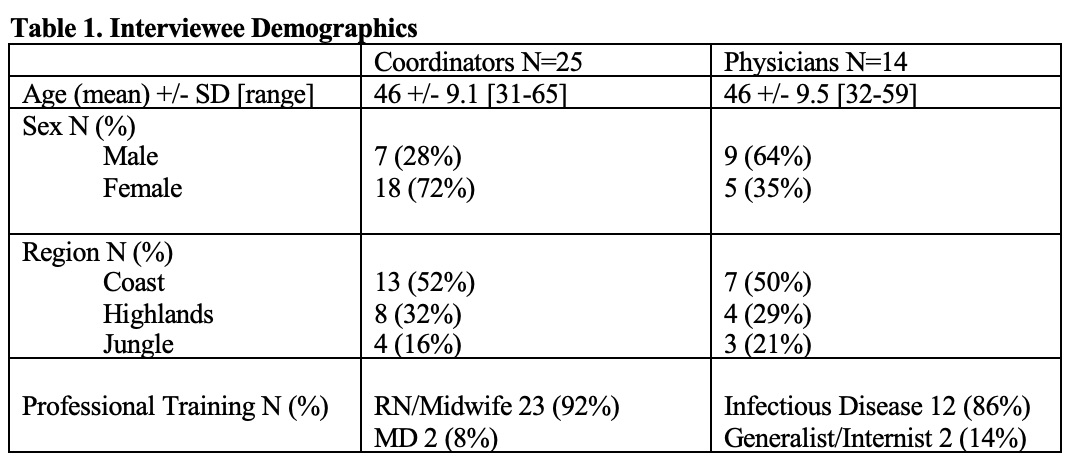
Results: Twenty-five regional coordinators and 14 physicians were interviewed to reach thematic saturation (Table 1). Barriers and facilitators discussed by both groups were organized into major themes following a socioecological model: patient, provider, local clinic/hospital, regional, and national health system (Figure 1). Coordinators highlighted health system components such as budget, resources, the impact of the pandemic, existing NCD programs, lack of epidemiologic data on NCDs, and a motivation to improve care for PLWH. While some physicians were enthusiastic about learning more and providing osteoporosis/sarcopenia care themselves or were already providing some direct management, others felt that the patient was better served by referral to a specialist. Physicians noted barriers of knowledge/training, interest, time, workload, lack of guidelines, available medications and DXA, and an inclination to stay within the scope of their specialty, which is encouraged by their health system at the local and national levels. Physicians reported that they were aware of the growing burden of NCDs in patients aging with HIV. They described a unique position of trust with their patients, who preferred their HIV provider to manage their NCDs to simplify their care and avoid stigma, especially in areas lacking access to NCD-trained specialists.
Conclusion: This study highlights the complex interplay between patient, provider, local, regional, and national factors that influence care delivery to PLWH in Peru. Addressing the barriers of osteoporosis and sarcopenia management in PLWH will require support from HIV physicians and coordinators as well as health system level interventions such as national guidelines, training, and increased access to screening resources.
R. Slotkin: None; D. Granda Calderón: None; J. Malca Hernandez: None; D. Cabrera: None; C. Benites Villafane: None; P. García: None; E. Hsieh: None.
Background/Purpose: Persons living with HIV (PLWH) have a higher risk of developing age-related non-communicable diseases (NCDs), such as osteoporosis and sarcopenia. In Peru, HIV providers are the primary point of medical care for PLWH. Using a qualitative approach, we examined health system barriers and facilitators for osteoporosis and sarcopenia care for PLWH in Peru from the perspective of HIV physicians and coordinators.
Methods: HIV regional program coordinators and physicians affiliated with Peru's National HIV, STI and Hepatitis Program were recruited from the Program's physician and coordinator registry and by peer referral. All coordinators (N=31) were contacted for a semi-structured in-depth interview over Zoom by a trained Peruvian research assistant. Physicians were purposefully sampled to ensure adequate regional representation. Interviews continued until thematic saturation was reached in both groups. The interviews were recorded and transcribed using Sonix.ai and checked for accuracy. Transcripts were translated to English following a standardized protocol by a team of bilingual translators, and then coded in English by two independent coders, one of which was Peruvian to ensure culturally appropriate codes. All codes were discussed, and discrepancies were resolved by consensus. The emerging themes and sub-themes were visualized using an adapted socioecological framework.
Results: Twenty-five regional coordinators and 14 physicians were interviewed to reach thematic saturation (Table 1). Barriers and facilitators discussed by both groups were organized into major themes following a socioecological model: patient, provider, local clinic/hospital, regional, and national health system (Figure 1). Coordinators highlighted health system components such as budget, resources, the impact of the pandemic, existing NCD programs, lack of epidemiologic data on NCDs, and a motivation to improve care for PLWH. While some physicians were enthusiastic about learning more and providing osteoporosis/sarcopenia care themselves or were already providing some direct management, others felt that the patient was better served by referral to a specialist. Physicians noted barriers of knowledge/training, interest, time, workload, lack of guidelines, available medications and DXA, and an inclination to stay within the scope of their specialty, which is encouraged by their health system at the local and national levels. Physicians reported that they were aware of the growing burden of NCDs in patients aging with HIV. They described a unique position of trust with their patients, who preferred their HIV provider to manage their NCDs to simplify their care and avoid stigma, especially in areas lacking access to NCD-trained specialists.
Conclusion: This study highlights the complex interplay between patient, provider, local, regional, and national factors that influence care delivery to PLWH in Peru. Addressing the barriers of osteoporosis and sarcopenia management in PLWH will require support from HIV physicians and coordinators as well as health system level interventions such as national guidelines, training, and increased access to screening resources.


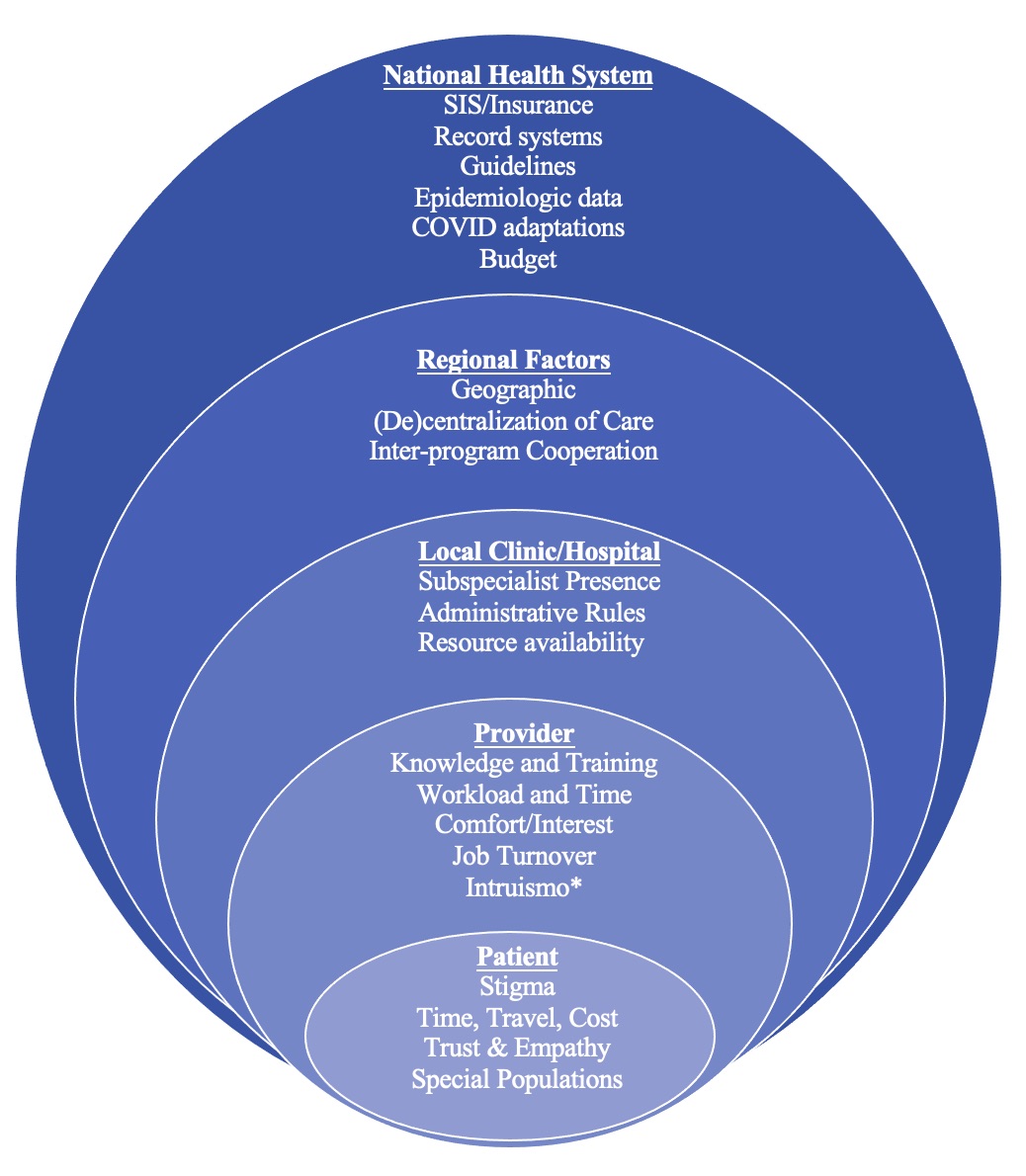
Figure 1. Socioecological Model Applied to Barriers and Facilitators of Osteoporosis and Sarcopenia Care for Persons Living with HIV. Emerging themes and sub-themes from physician and coordinator interviews were visualized using this adapted socioecological model. *Translates to the idea that one should not overstep the boundaries of their specialty.
R. Slotkin: None; D. Granda Calderón: None; J. Malca Hernandez: None; D. Cabrera: None; C. Benites Villafane: None; P. García: None; E. Hsieh: None.



