Poster Session C
Vasculitis
Session: (2387–2424) Vasculitis – Non-ANCA-Associated & Related Disorders Poster III
2397: Impact of Exposure to Environmental Air Pollution on the Onset of Giant Cell Arteritis
Tuesday, November 14, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- MB
Milena Bond, MD
Azienda sanitaria dell'Alto Adige
Merano, Bolzano, ItalyDisclosure information not submitted.
Abstract Poster Presenter(s)
Milena Bond1, Alessandro Tomelleri2, Maria Antonietta Reatini3, Corrado Campochiaro4, Giorgio Cattani3, Lorenzo Dagna5, Maurizio Rossini6, Christian Dejaco7 and Giovanni Adami6, 1Azienda sanitaria dell'Alto Adige, Merano, Italy, 2Unit of Immunology, Rheumatology, Allergy and Rare Diseases, San Raffaele Scientific Institute, Milano, Italy, 3Italian Institute for Environmental Protection and Research, Rome, Italy, 4IRCCS San Raffaele Hospital, Unit of Immunology, Rheumatology, Allergy and Rare Disease. Vita-Salute San Raffaele University, Milan, Italy, 5Department of Internal Medicine, IRCCS San Raffaele Hospital and Vita-Salute San Raffaele University, Milan, Italy, 6Rheumatology Unit, Department of Medicine, University of Verona, Verona, Italy, 7Department of Rheumatology, Medical University Graz, Graz, Austria; Department of Rheumatology, Hospital of Bruneck (ASAA-SABES), Teaching Hospital of the Paracelsius Medical University, Brunico, Italy
Background/Purpose: Environmental air pollution (AP) has been found to affect vascular inflammation and to contribute to the risk of onset and flare of autoimmune diseases1,2. Giant cell arteritis (GCA) has been reported to be more prevalent in urban than in rural areas3, indicating a possible link between AP and disease onset. The objective of this study is to investigate whether there is an association between exposure to AP and the risk of developing GCA and its ischemic complications.
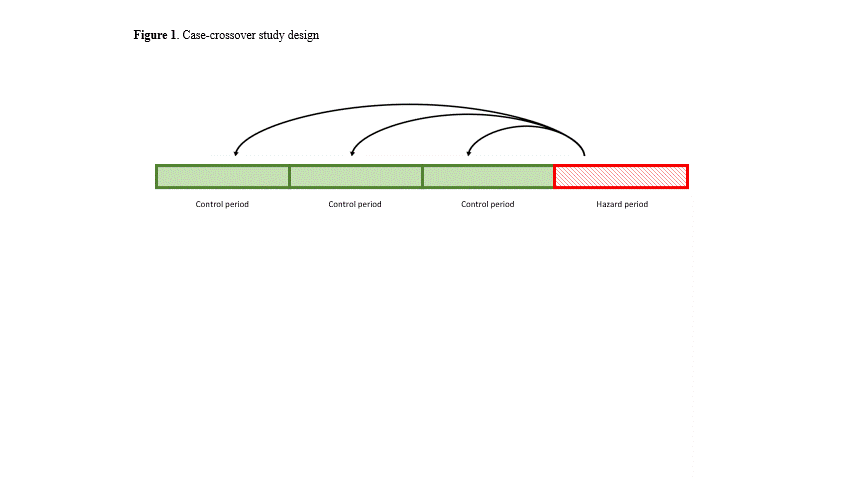
Methods: Charts of consecutive patients with GCA followed between June 2013 and December 2021 in three hospitals (Bozen, Milan, Verona) of Northern Italy were reviewed. Only patients who were resident in Italy at the time of diagnosis and who had confirmed GCA, a follow-up ≥ 6 months and precise information on disease onset were included. Data collection included demographics, clinical information, and ZIP code of residency. Patients were linked to their daily particulate matter (PM10, mass concentration, particles with aerodynamic diameter ≤10µm), exposure derived from a spatio-temporal interpolation process using a Bayesian hierarchical model that included 11 spatial and spatio-temporal predictors, such as meteorological variables and Aerosol Optical Depth. The model was cross-validated, showed good performance and provides a 1km x 1km spatial resolution for daily exposure to PM10. A case-crossover study with conditional logistic regression was conducted to investigate the acute effect of PM10 exposure on disease onset and the development of ischemic complications. Several lag exposures before symptoms onset were selected (hazard periods) and compared to 3 same-length periods prior to symptoms onset (control periods) (Figure 1).
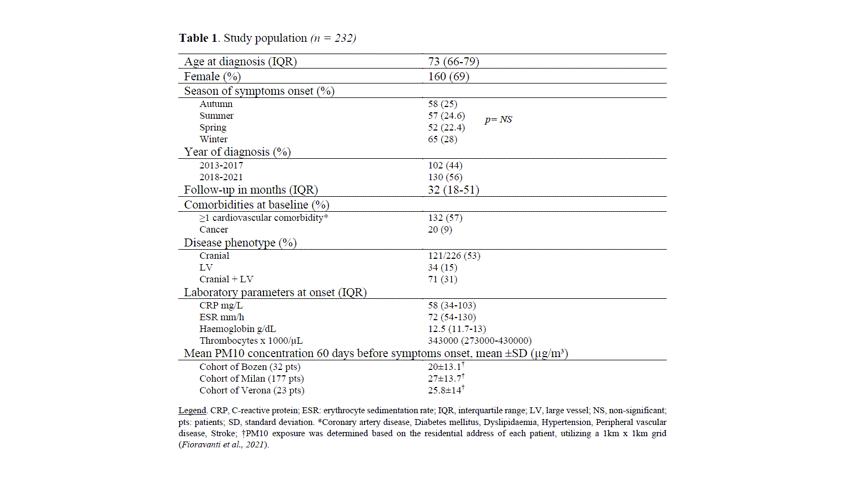
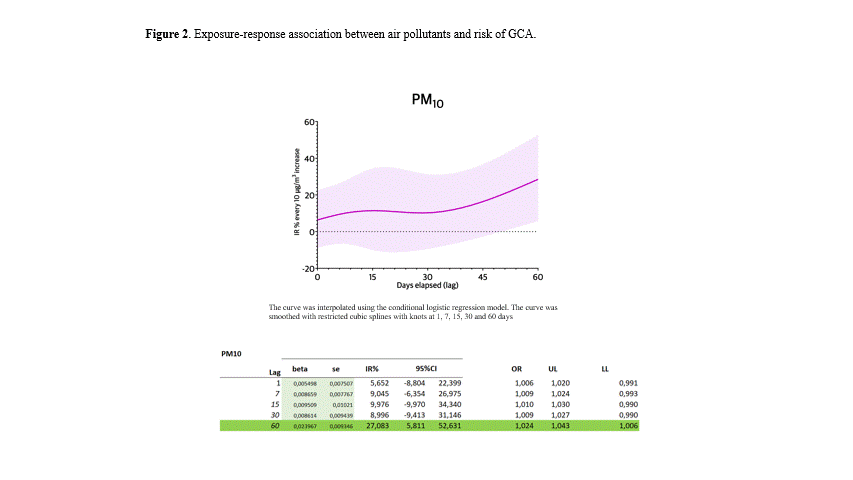
Results: Two hundred and thirty-two patients were included. Table 1 summarizes their main demographic and clinical features. Figure 2 shows the exposure-response association between air pollutants and the risk of developing GCA. Incremental odds (%) of GCA every 10 µg/m³ increase in PM10 concentration at different lag-exposure were found. Specifically, the incremental risk (every 10 µg/m³ increase in PM10) for 60-day lag was27,08 (95% CI 5,81-52,63); at shorter lags we found no significant association. There was no significant difference after adjusting for seasonality. Fifty-nine patients (25%) suffered from a GCA-related ischemic complication. No significant association between exposure to PM10 and ischemic complications was found (p=.198).
Conclusion: Conclusion. Acute exposure to environmental AP PM10 seems to be associated with a higher risk of developing GCA but not with GCA-related ischemic complications. Further studies on larger cohorts are needed to confirm these preliminary results.
Bibliography
Ke Wei, Gen Biol 2007; 2. Adami, Rheumatology 2021; 3. Reinhold-Keller, Rheumatology 2000
M. Bond: AbbVie/Abbott, 5; A. Tomelleri: Novartis, 1; M. Reatini: None; C. Campochiaro: Boehringer Ingelheim, 1, 6, Janssen, 1, 6, Novartis, 1, 6; G. Cattani: None; L. Dagna: AbbVie, 2, AstraZeneca, 2, Biogen, 2, BMS, 2, 5, Boehringer Ingelheim, 2, Celltrion, 5, Eli Lilly, 2, Galapagos, 2, GSK, 1, Janssen, 2, Kiniksa Pharmaceuticals, 2, 5, Novartis, 2, 6, Pfizer, 2, 5, Sobi, 2, 5, 6; M. Rossini: None; C. Dejaco: AbbVie/Abbott, 1, 5, 6, Eli Lilly, 6, Galapagos Pharma, 1, 6, Janssen, 1, 6, Novartis, 1, 6, Pfizer, 6, Sparrow, 1; G. Adami: None.
Background/Purpose: Environmental air pollution (AP) has been found to affect vascular inflammation and to contribute to the risk of onset and flare of autoimmune diseases1,2. Giant cell arteritis (GCA) has been reported to be more prevalent in urban than in rural areas3, indicating a possible link between AP and disease onset. The objective of this study is to investigate whether there is an association between exposure to AP and the risk of developing GCA and its ischemic complications.
Methods: Charts of consecutive patients with GCA followed between June 2013 and December 2021 in three hospitals (Bozen, Milan, Verona) of Northern Italy were reviewed. Only patients who were resident in Italy at the time of diagnosis and who had confirmed GCA, a follow-up ≥ 6 months and precise information on disease onset were included. Data collection included demographics, clinical information, and ZIP code of residency. Patients were linked to their daily particulate matter (PM10, mass concentration, particles with aerodynamic diameter ≤10µm), exposure derived from a spatio-temporal interpolation process using a Bayesian hierarchical model that included 11 spatial and spatio-temporal predictors, such as meteorological variables and Aerosol Optical Depth. The model was cross-validated, showed good performance and provides a 1km x 1km spatial resolution for daily exposure to PM10. A case-crossover study with conditional logistic regression was conducted to investigate the acute effect of PM10 exposure on disease onset and the development of ischemic complications. Several lag exposures before symptoms onset were selected (hazard periods) and compared to 3 same-length periods prior to symptoms onset (control periods) (Figure 1).
Results: Two hundred and thirty-two patients were included. Table 1 summarizes their main demographic and clinical features. Figure 2 shows the exposure-response association between air pollutants and the risk of developing GCA. Incremental odds (%) of GCA every 10 µg/m³ increase in PM10 concentration at different lag-exposure were found. Specifically, the incremental risk (every 10 µg/m³ increase in PM10) for 60-day lag was27,08 (95% CI 5,81-52,63); at shorter lags we found no significant association. There was no significant difference after adjusting for seasonality. Fifty-nine patients (25%) suffered from a GCA-related ischemic complication. No significant association between exposure to PM10 and ischemic complications was found (p=.198).
Conclusion: Conclusion. Acute exposure to environmental AP PM10 seems to be associated with a higher risk of developing GCA but not with GCA-related ischemic complications. Further studies on larger cohorts are needed to confirm these preliminary results.
Bibliography
Ke Wei, Gen Biol 2007; 2. Adami, Rheumatology 2021; 3. Reinhold-Keller, Rheumatology 2000



M. Bond: AbbVie/Abbott, 5; A. Tomelleri: Novartis, 1; M. Reatini: None; C. Campochiaro: Boehringer Ingelheim, 1, 6, Janssen, 1, 6, Novartis, 1, 6; G. Cattani: None; L. Dagna: AbbVie, 2, AstraZeneca, 2, Biogen, 2, BMS, 2, 5, Boehringer Ingelheim, 2, Celltrion, 5, Eli Lilly, 2, Galapagos, 2, GSK, 1, Janssen, 2, Kiniksa Pharmaceuticals, 2, 5, Novartis, 2, 6, Pfizer, 2, 5, Sobi, 2, 5, 6; M. Rossini: None; C. Dejaco: AbbVie/Abbott, 1, 5, 6, Eli Lilly, 6, Galapagos Pharma, 1, 6, Janssen, 1, 6, Novartis, 1, 6, Pfizer, 6, Sparrow, 1; G. Adami: None.



