Poster Session B
Osteoarthritis (OA) and related disorders
Session: (1183–1199) Osteoarthritis – Clinical Poster II
1184: A Wearable-Sensor for Assessment of Gait and Chair Stand Patterns in People with Knee Osteoarthritis: Validation and Responsiveness to Treatment of a Potential Digital Biomarker
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- DK
Deepak Kumar, PhD, PT
Boston University
Boston, MA, United StatesDisclosure(s): Eli Lilly: Grant/Research Support (Ongoing); Pfizer: Grant/Research Support (Ongoing)
Abstract Poster Presenter(s)
Deepak Kumar1, Lukas Adamowicz2, Benjamin Senderling1, Mary Gheller1, Michael LaValley3, Kathryn Bacon1, Pirinka Georgiev2, Charmaine Demanuele2, Paul Wacnik2 and Tuhina Neogi4, 1Boston University, Boston, MA, 2Pfizer Inc., Cambridge, MA, 3Boston University School of Public Health, Arlington, MA, 4Boston University School of Medicine, Boston, MA
Background/Purpose: The objectives of this study in people with knee osteoarthritis (OA) were to (a) examine the agreement between measures of gait and chair stand patterns derived from a wearable-sensor and those from gold-standard motion capture, (b) assess the correlation between wearable-sensor derived measures and standard functional measures, and (c) examine the responsiveness of wearable-sensor derived measures to an exercise-based physical therapy intervention.
Methods: We conducted a single-arm clinical trial (NCT04243096) of a 12-week exercise intervention in people with symptomatic knee OA (n = 60, age = 66.3±7.4 years; 75% women; BMI = 29.0±4.8 kg/m2). Participants received 18 sessions of an exercise-based physical therapy intervention over 12 weeks. Spatiotemporal gait parameters and measures of chair stand mechanics (Table 2) were extracted from an inertial sensor worn on the lower back as well as from optical motion capture during walking at self-selected pace and chair stand tasks. Agreement between sensor and motion capture measures was examined using intraclass coefficients (ICC [2,1]). Participants also completed standard functional tests including a walking test (28-meters), 5 times chair stand test, and a 6-minute walk test, while wearing the inertial sensor and correlations between sensor derived measures and functional measures were assessed. The wearable sensor measures with excellent agreement with motion capture and standard measures during functional tests were evaluated with mixed model repeated measures (MMRM) models with visit as a categorical factor adjusting for age, sex, BMI, and presence of comorbidities.
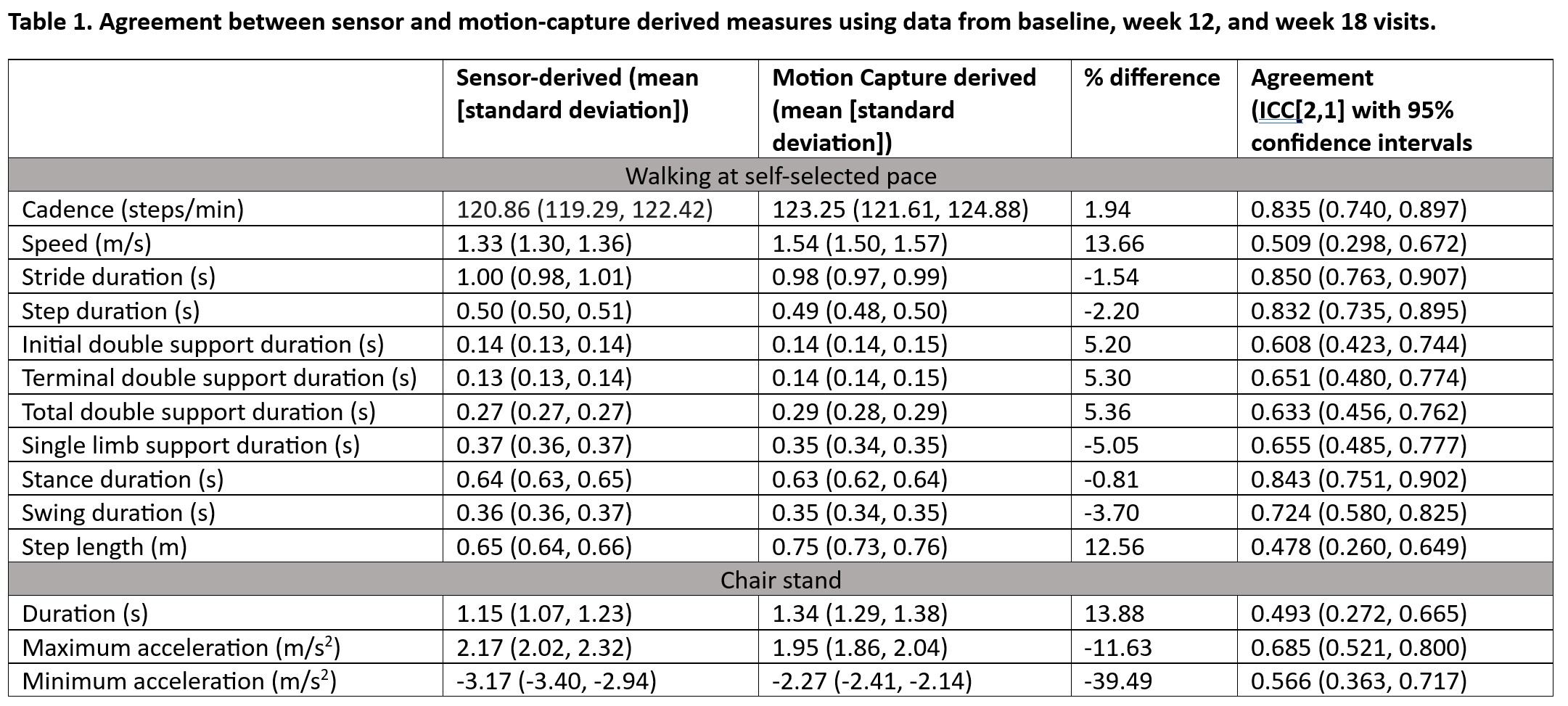
Results: The agreement between sensor and motion capture derived measures was excellent (ICC ≥ 0.75) for cadence, stride duration, step duration, and stance duration, good (0.6≤ICC≤0.74) for initial double support duration, terminal double support duration, total double support duration, and swing time, and moderate (0.4≤ICC≤0.59) for step length and gait speed (Table 1). Sensor derived measures and functional measures were significantly correlated in the expected directions with somewhat stronger correlations during 6-minute walk (range 0.68-0.90) vs. and 5-time chair stand (range 0.67-0.70) vs. 28-meter walk (range 0.46-0.65). With the intervention, all sensor derived measures showed significant improvements in all functional tests with the improvement maintained from 12- to 18-weeks (Figure 1 and 2).
Conclusion: Multiple measures of gait and chair stand patterns derived using a single inertial sensor demonstrate good agreement with gold-standard measures derived from motion capture. Spatial measures (step length, speed) performed worse than temporal measures. Sensor derived measures are moderately correlated with standard functional outcomes and may provide additional information not captured by standard measures. Sensor derived measures are responsive to change with an effective treatment and potentially could serve as digital biomarker for monitoring or treatment response.
D. Kumar: Eli Lilly, 5, Pfizer, 5; L. Adamowicz: Pfizer, 3; B. Senderling: None; M. Gheller: None; M. LaValley: None; K. Bacon: None; P. Georgiev: Pfizer, 3, 11; C. Demanuele: Pfizer, 3, 11; P. Wacnik: Pfizer, 11; T. Neogi: None.
Background/Purpose: The objectives of this study in people with knee osteoarthritis (OA) were to (a) examine the agreement between measures of gait and chair stand patterns derived from a wearable-sensor and those from gold-standard motion capture, (b) assess the correlation between wearable-sensor derived measures and standard functional measures, and (c) examine the responsiveness of wearable-sensor derived measures to an exercise-based physical therapy intervention.
Methods: We conducted a single-arm clinical trial (NCT04243096) of a 12-week exercise intervention in people with symptomatic knee OA (n = 60, age = 66.3±7.4 years; 75% women; BMI = 29.0±4.8 kg/m2). Participants received 18 sessions of an exercise-based physical therapy intervention over 12 weeks. Spatiotemporal gait parameters and measures of chair stand mechanics (Table 2) were extracted from an inertial sensor worn on the lower back as well as from optical motion capture during walking at self-selected pace and chair stand tasks. Agreement between sensor and motion capture measures was examined using intraclass coefficients (ICC [2,1]). Participants also completed standard functional tests including a walking test (28-meters), 5 times chair stand test, and a 6-minute walk test, while wearing the inertial sensor and correlations between sensor derived measures and functional measures were assessed. The wearable sensor measures with excellent agreement with motion capture and standard measures during functional tests were evaluated with mixed model repeated measures (MMRM) models with visit as a categorical factor adjusting for age, sex, BMI, and presence of comorbidities.
Results: The agreement between sensor and motion capture derived measures was excellent (ICC ≥ 0.75) for cadence, stride duration, step duration, and stance duration, good (0.6≤ICC≤0.74) for initial double support duration, terminal double support duration, total double support duration, and swing time, and moderate (0.4≤ICC≤0.59) for step length and gait speed (Table 1). Sensor derived measures and functional measures were significantly correlated in the expected directions with somewhat stronger correlations during 6-minute walk (range 0.68-0.90) vs. and 5-time chair stand (range 0.67-0.70) vs. 28-meter walk (range 0.46-0.65). With the intervention, all sensor derived measures showed significant improvements in all functional tests with the improvement maintained from 12- to 18-weeks (Figure 1 and 2).
Conclusion: Multiple measures of gait and chair stand patterns derived using a single inertial sensor demonstrate good agreement with gold-standard measures derived from motion capture. Spatial measures (step length, speed) performed worse than temporal measures. Sensor derived measures are moderately correlated with standard functional outcomes and may provide additional information not captured by standard measures. Sensor derived measures are responsive to change with an effective treatment and potentially could serve as digital biomarker for monitoring or treatment response.

Table 1. Agreement between sensor and motion-capture derived measures using data from baseline, week 12, and week 18 visits.

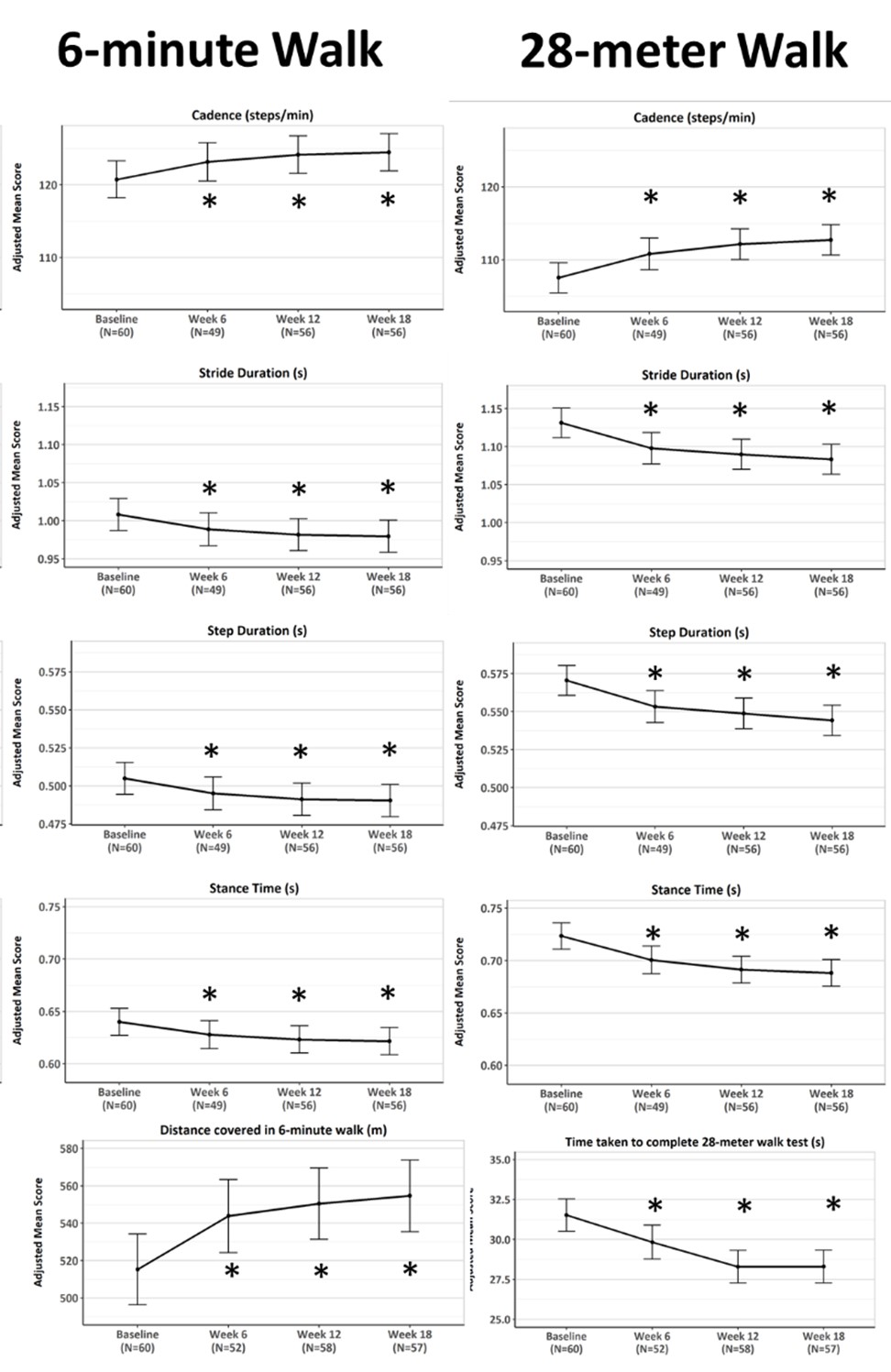
Figure 1. Adjusted means for sensor-derived measures (with excellent agreement) and standard functional measures at baseline, week 6, week 12, and week 18 during the 6-minute walk test (left) and 28-meter walk test (right). * indicates significant change compared to baseline.

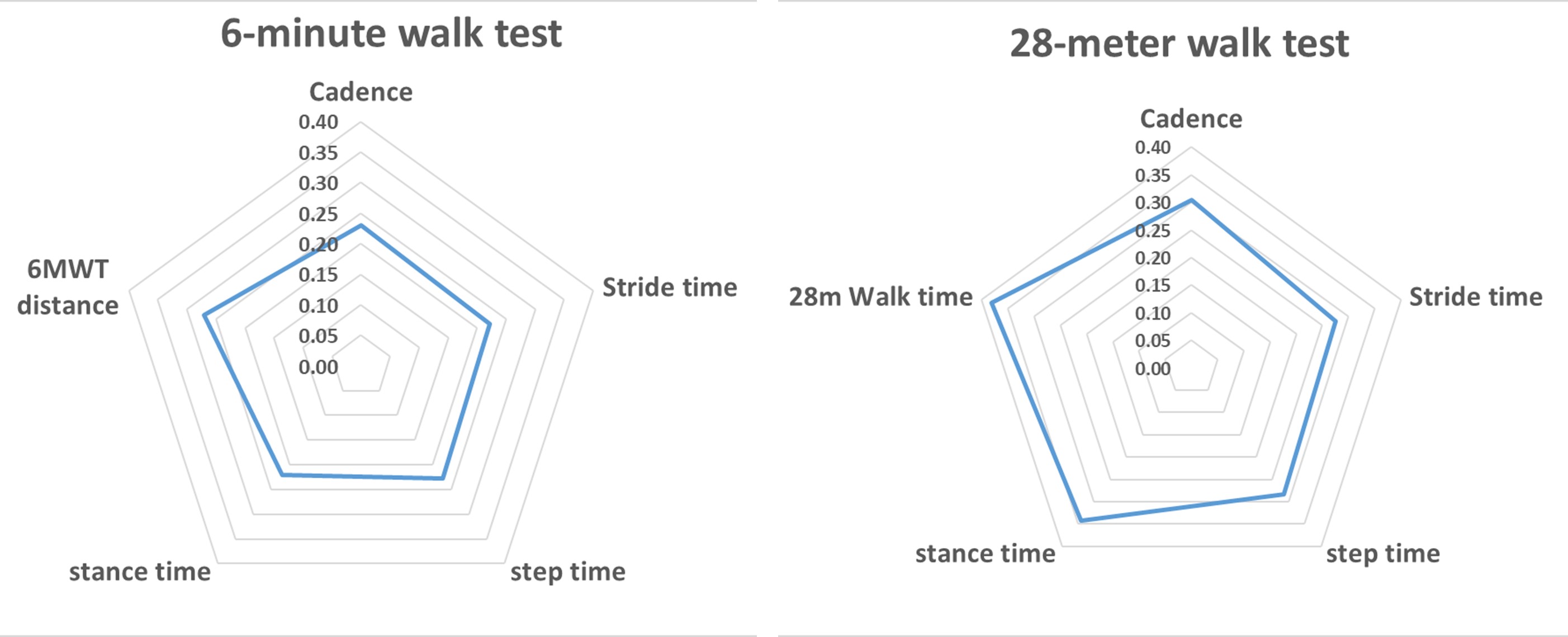
Figure 2. Standardized response means for change from baseline to week 12 in sensor-derived measures (with excellent agreement) and standard functional measures during 6-minute walk test (left) and 28-meter walk test (right)
D. Kumar: Eli Lilly, 5, Pfizer, 5; L. Adamowicz: Pfizer, 3; B. Senderling: None; M. Gheller: None; M. LaValley: None; K. Bacon: None; P. Georgiev: Pfizer, 3, 11; C. Demanuele: Pfizer, 3, 11; P. Wacnik: Pfizer, 11; T. Neogi: None.



