Poster Session B
Epidemiology, health policy and outcomes
Session: (0993–1012) Health Services Research Poster II
0994: Narrative Medicine and Pediatric Rheumatology: Addressing Burnout and Bias
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall

Aviya Lanis, MD (she/her/hers)
Seattle Children's Hospital
Seattle, WA, United StatesDisclosure(s): No financial relationships with ineligible companies to disclose
Abstract Poster Presenter(s)
Aviya Lanis, Natalie Rosenwasser and Esi Morgan, Seattle Children's Hospital, Seattle, WA
Background/Purpose: Burnout, a syndrome of emotional exhaustion and depersonalization, adversely impacts healthcare and results in mood disturbances, poor patient and provider satisfaction and high turnover. Studies have shown burnout also plays a critical role in physician bias, with increased bias among those with higher rates of burnout. The SARS-CoV-2 pandemic increased levels of burnout and exposed the high prevalence of racial bias in healthcare. There is a critical need for methods to address burnout and bias in healthcare. Narrative medicine (NM) incorporates the stories of human experience into the medical realm and has been proven to strengthen relationships and increase empathy. To date, limited data investigating narrative medicine's impact on burnout and bias has been promising. This pilot study aims to investigate the use of NM as a tool to address burnout and explore bias amongst a pediatric rheumatology division.
Methods: Physicians, nurses, medical assistants and staff at a single center enrolled in a series of six monthly 1-hour video-based sessions lead by co-facilitators (AL, and a NM-trained facilitator) after informed consent. Sessions utilized poetry, photography, paintings, and spoken word to inspire writing prompts around the medical experience. A Plan-Do-Study-Act approach was used to guide intervention adjustments based on participant post-session feedback. Demographics were collected, and standard surveys were administered at baseline, and after the third and sixth sessions, specifically: Mini Z Burnout, Copenhagen Burnout Inventory (CBI), Provider Health Questionnaire-9 (PHQ-9) as well as Implicit Association Testing (IAT) and explicit bias Feeling Thermometer (FT).Survey data were assessed for differences with a Wilcoxon signed rank test.
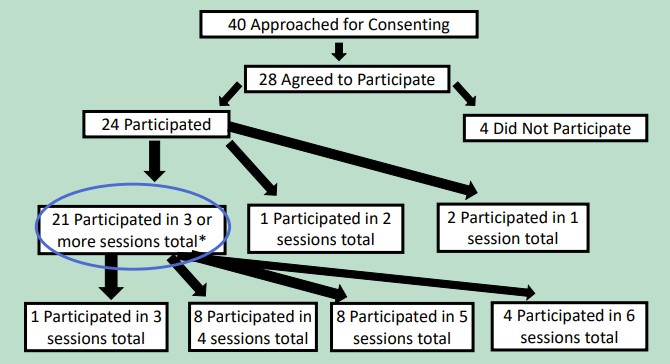
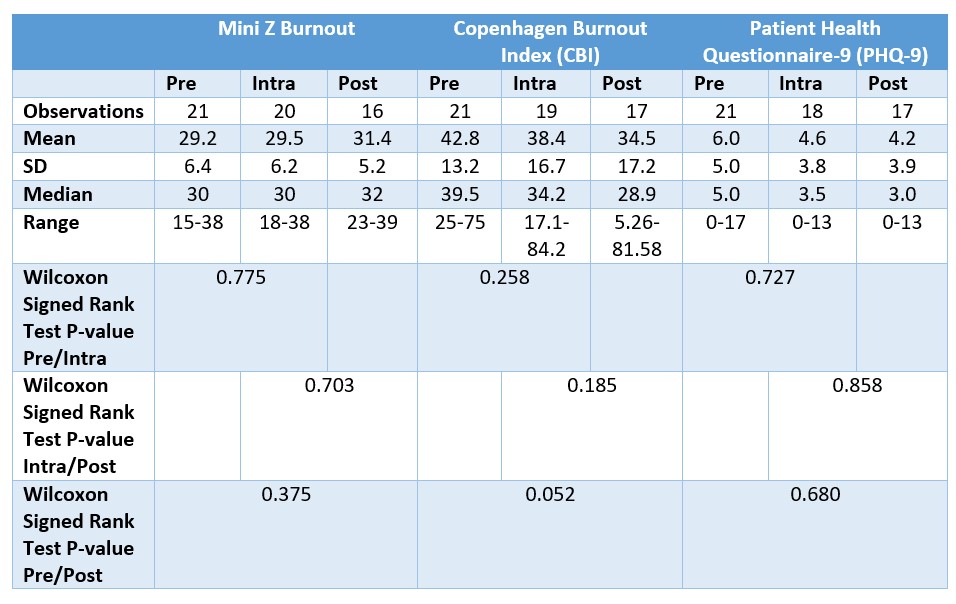
Results: Twenty-four participants with 21 females, 2 males and one non-binary were divided amongst 6 narrative medicine groups for the 6 total sessions. Data analysis was completed for those who attended 3 or more sessions (n=21) (See Figure 1). Self-identified race included 18 White, 4 Asian, 1 Black, and 1 who preferred not to answer. Participants included 8 attendings, 4 fellows, 2 nurses, 2 medical assistants, and 8 staff members. While no statistical significance was seen when evaluating questionnaires for the Mini Z Burnout, CBI, or PHQ-9 when comparing questionnaires from baseline and after 6 months into participation, there was a trend toward improvement with median CBI improved from 39.5 to 28.9, and median PHQ-9 score improved from 5 to 3. (Table 1). IAT showed a statistically significant shift towards positive association with African Americans following participation (p-value= 0.012), while FT showed a non-statistically significant explicit bias shift away from positive association with European Americans (p=0.096).
Conclusion: Narrative medicine is a feasible intervention that warrants further study as a means to address bias. Additional long-term analysis is needed to understand if these changes are durable.
A. Lanis: None; N. Rosenwasser: None; E. Morgan: None.
Background/Purpose: Burnout, a syndrome of emotional exhaustion and depersonalization, adversely impacts healthcare and results in mood disturbances, poor patient and provider satisfaction and high turnover. Studies have shown burnout also plays a critical role in physician bias, with increased bias among those with higher rates of burnout. The SARS-CoV-2 pandemic increased levels of burnout and exposed the high prevalence of racial bias in healthcare. There is a critical need for methods to address burnout and bias in healthcare. Narrative medicine (NM) incorporates the stories of human experience into the medical realm and has been proven to strengthen relationships and increase empathy. To date, limited data investigating narrative medicine's impact on burnout and bias has been promising. This pilot study aims to investigate the use of NM as a tool to address burnout and explore bias amongst a pediatric rheumatology division.
Methods: Physicians, nurses, medical assistants and staff at a single center enrolled in a series of six monthly 1-hour video-based sessions lead by co-facilitators (AL, and a NM-trained facilitator) after informed consent. Sessions utilized poetry, photography, paintings, and spoken word to inspire writing prompts around the medical experience. A Plan-Do-Study-Act approach was used to guide intervention adjustments based on participant post-session feedback. Demographics were collected, and standard surveys were administered at baseline, and after the third and sixth sessions, specifically: Mini Z Burnout, Copenhagen Burnout Inventory (CBI), Provider Health Questionnaire-9 (PHQ-9) as well as Implicit Association Testing (IAT) and explicit bias Feeling Thermometer (FT).Survey data were assessed for differences with a Wilcoxon signed rank test.
Results: Twenty-four participants with 21 females, 2 males and one non-binary were divided amongst 6 narrative medicine groups for the 6 total sessions. Data analysis was completed for those who attended 3 or more sessions (n=21) (See Figure 1). Self-identified race included 18 White, 4 Asian, 1 Black, and 1 who preferred not to answer. Participants included 8 attendings, 4 fellows, 2 nurses, 2 medical assistants, and 8 staff members. While no statistical significance was seen when evaluating questionnaires for the Mini Z Burnout, CBI, or PHQ-9 when comparing questionnaires from baseline and after 6 months into participation, there was a trend toward improvement with median CBI improved from 39.5 to 28.9, and median PHQ-9 score improved from 5 to 3. (Table 1). IAT showed a statistically significant shift towards positive association with African Americans following participation (p-value= 0.012), while FT showed a non-statistically significant explicit bias shift away from positive association with European Americans (p=0.096).
Conclusion: Narrative medicine is a feasible intervention that warrants further study as a means to address bias. Additional long-term analysis is needed to understand if these changes are durable.

Figure 1: Breakdown of individuals consented compared to those who participated.

Table 1: Pre-, intra- and post-participation questionnaire results including observations, mean, standard deviation (SD), median, range, and Wilcoxon signed-rank test p-values. For Mini Z Burnout, a score of 20 or higher is considered to be a joyful work environment. For the CBI, a score of 50-74 is concerning for moderate burnout, 75-99 with high burnout, and a score of 100 shows severe burnout. For the PHQ-9, a score of 1-4 demonstrates minimal depression, 5-9 demonstrates mild depression, 10-14 demonstrates moderate depression and 20-27 demonstrates severe depression.
A. Lanis: None; N. Rosenwasser: None; E. Morgan: None.



