Poster Session B
Systemic lupus erythematosus (SLE)
Session: (1442–1487) SLE – Diagnosis, Manifestations, & Outcomes Poster II
1473: Mortality from Diseases of the Nervous System in Patients with Lupus in the past Two Decades
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- AD
Ansaam Daoud, MD
Case Western Reserve University/University Hospitals
Akron, OH, United StatesDisclosure information not submitted.
Abstract Poster Presenter(s)
Ansaam Daoud1, Loai Dweik2, Marina Nighat Magrey3 and Omer Pamuk4, 1University Hospitals, Case Western Reserve University, Akron, OH, 2Cleveland Clinic Akron General, Akron, OH, 3Case Western Reserve University, University Hospitals, Cleveland, OH, 4University Hospitals Cleveland Medical Center, Cleveland, OH
Background/Purpose: SLE is a chronic autoimmune disease and affects many organ systems. Juvenile onset disease, male sex, renal involvement, and central nervous system involvement are poor prognostic factors in SLE. ACR defined some neuropsychiatric symptoms in SLE. However, their attribution to SLE is challenging due to confounding factors, especially in older populations. Atherosclerotic complications, including cardiovascular and cerebrovascular diseases, are important causes of mortality in patients with SLE. Until now, no study has evaluated nervous system mortality causes in SLE patients. This study investigated nervous system-related mortality in SLE in the past two decades in the USA.
Methods: This retrospective cohort study used the Multiple Cause of Death files maintained by the National Center for Health Statistics to investigate the direction of proportionate nervous system-related mortality in SLE, defined as the number of deaths from diseases of the nervous system (the underlying cause of death: International Classification of Diseases, version 10 [ICD10]: G00-G98), divided by the number of all-cause mortality in patients with SLE (defined in multiple causes of death: ICD10 code M32) from 1999-2020. The data set utilizes death certificate data for US residents. To analyze changes in mortality trends, we separated the study period into two decades, the first decade (1999-2009) and the last decade (2010-2020). Spearman's correlation test was used for trend analysis, and the Chi-square test was used for comparisons.
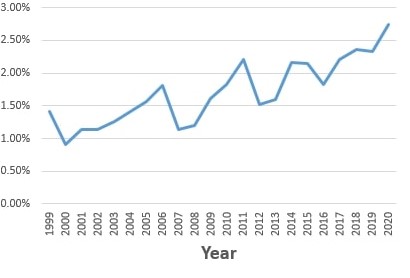
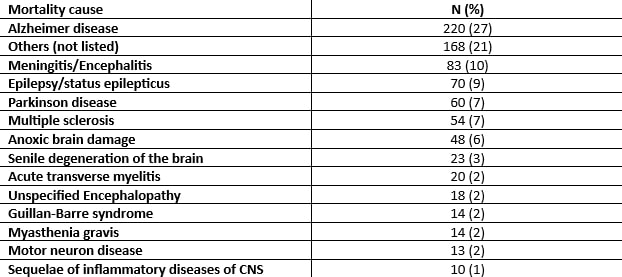
Results: 47,337 deaths in SLE occurred during the study period. 814 (1.72%) died of nervous system causes. The mean age for nervous system-related mortality was 69.3 years. Proportionate nervous system-related mortality in SLE was higher in women than men (1.79% vs. 1.34%, p=0.0087), significantly lower in African-American SLE patients than in other races (1.27% vs. 1.93%, p< 0.00001), and lower in Hispanic SLE patients than non-Hispanic patients (1.24% vs. 1.79%, p=0.0034). Proportionate mortality from nervous system disease increased from 1.33% in the first decade (1999-2009) to 2.11% in the second decade (p< 0.00001) (Figure 1). The most common nervous system cause of death in SLE was Alzheimer's Disease (27%). Table 1 shows other nervous system causes for mortality (Table 1).
Conclusion: This national data showed a significant increase in proportionate mortality from nervous system diseases in SLE. SLE patients in ethnic or racial minority groups seem protected from nervous system-related mortality. Prospective cohort studies are required to understand these trends.
A. Daoud: None; L. Dweik: None; M. Magrey: AbbVie, 2, Bristol Myers Squibb, 2, Eli Lilly, 2, Novartis, 2, Pfizer Inc, 2, UCB, 5; O. Pamuk: None.
Background/Purpose: SLE is a chronic autoimmune disease and affects many organ systems. Juvenile onset disease, male sex, renal involvement, and central nervous system involvement are poor prognostic factors in SLE. ACR defined some neuropsychiatric symptoms in SLE. However, their attribution to SLE is challenging due to confounding factors, especially in older populations. Atherosclerotic complications, including cardiovascular and cerebrovascular diseases, are important causes of mortality in patients with SLE. Until now, no study has evaluated nervous system mortality causes in SLE patients. This study investigated nervous system-related mortality in SLE in the past two decades in the USA.
Methods: This retrospective cohort study used the Multiple Cause of Death files maintained by the National Center for Health Statistics to investigate the direction of proportionate nervous system-related mortality in SLE, defined as the number of deaths from diseases of the nervous system (the underlying cause of death: International Classification of Diseases, version 10 [ICD10]: G00-G98), divided by the number of all-cause mortality in patients with SLE (defined in multiple causes of death: ICD10 code M32) from 1999-2020. The data set utilizes death certificate data for US residents. To analyze changes in mortality trends, we separated the study period into two decades, the first decade (1999-2009) and the last decade (2010-2020). Spearman's correlation test was used for trend analysis, and the Chi-square test was used for comparisons.
Results: 47,337 deaths in SLE occurred during the study period. 814 (1.72%) died of nervous system causes. The mean age for nervous system-related mortality was 69.3 years. Proportionate nervous system-related mortality in SLE was higher in women than men (1.79% vs. 1.34%, p=0.0087), significantly lower in African-American SLE patients than in other races (1.27% vs. 1.93%, p< 0.00001), and lower in Hispanic SLE patients than non-Hispanic patients (1.24% vs. 1.79%, p=0.0034). Proportionate mortality from nervous system disease increased from 1.33% in the first decade (1999-2009) to 2.11% in the second decade (p< 0.00001) (Figure 1). The most common nervous system cause of death in SLE was Alzheimer's Disease (27%). Table 1 shows other nervous system causes for mortality (Table 1).
Conclusion: This national data showed a significant increase in proportionate mortality from nervous system diseases in SLE. SLE patients in ethnic or racial minority groups seem protected from nervous system-related mortality. Prospective cohort studies are required to understand these trends.

Figure 1. Proportionate Nervous System Disease Mortality in SLE Patients Over the Past Two Decades

Table 1. Mortality in SLE Patients from Diseases of the Nervous System
A. Daoud: None; L. Dweik: None; M. Magrey: AbbVie, 2, Bristol Myers Squibb, 2, Eli Lilly, 2, Novartis, 2, Pfizer Inc, 2, UCB, 5; O. Pamuk: None.



