Poster Session B
Fibrosing rheumatic diseases (scleroderma, MCTD, IgG4-related disease, scleroderma mimics)
Session: (0934–0964) Systemic Sclerosis & Related Disorders – Basic Science Poster
0960: MiR-3606-3p Alleviates Skin Fibrosis by Suppressing Fibroblast Inflammation and Migration via Inhibiting GAB1 and ITGAV
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- YC
Abstract Poster Presenter(s)
yahui chen1, Mengkun shi1, Wei Wang1, Chenyi Shi1, Xueyi Xia1, wenyu Wu2, Jiucun Wang3 and Xiangguang Shi3, 1Fudan University, Shanghai, China, 2Huashan Hospital, Shanghai, China, 3Shanghai, Shanghai, China
Background/Purpose: Systemic sclerosis (SSc) and keloid are typical skin fibrotic diseases with unclear epigenetic mechanisms and clinical targets. As an important epigenetic regulatory factor, microRNAs play an important role in the occurrence and development of fibrosis in recent studies. This study aimed to assess the role of miR-3606-3p in skin fibrosis and the therapeutic potential.
Methods: The levels of miR-3606-3p were detected in SSc and keloid patients by qPCR and in situ hybridization. RNA-seq, in silico software and luciferase were performed to investigate the targets of miR-3606-3p. The effects of miR-3606-3p, GAB1 and ITGAV on fibroblast fibrogenesis, inflammation and migration were assessed in primary dermal fibroblasts by qPCR, western blotting, wound healing scratch assay. Histology, immunofluorescence analysis and in vivo imaging techniques were used to evaluate the effect of miR-3606-3p on alleviating skin fibrosis in keloid-bearing mice.
Results: MiR-3606-3p was reduced in the skin tissues and fibroblasts from both SSc and keloid patients and negatively correlated with disease severity. RNA-seq analysis and in silico prediction indicated GRB2 associated binding protein 1 (GAB1) and integrin subunit alpha V (ITGAV) were potential targets of miR-3606-3p. We then found that miR-3606-3p downregulated both GAB1 and ITGAV by directly targeting their 3′-UTRs, and further reduced p-AKT and p-ERK activities to inhibit collagen synthesis and NF-κB induced fibroblast inflammation. Furthermore, miR-3606-3p inhibited fibroblast migration in primary fibroblasts and keloid-bearing nude miceby wound healing scratch assay and in vivoimaging techniques respectively. In contrast, GAB1 and ITGAV were upregulated in SSc and keloid patients, and siRNA-mediated GAB1 or ITGAV knockdown replicated the phenotypes observed in miR-3606-3p-overexpressing fibroblasts, including inflammation, migration and fibrogenesis (Figure 1). Finally, by constructing the humanized mouse model of transplanted keloid graft, we found that miR-3606-3p treatment inhibits GAB1 and ITGAV leading to significantly alleviate skin fibrosis (Figure 2).
Conclusion: Our results indicated miR-3606-3p inhibits ECM deposition, inflammation, and migration of fibroblasts by downregulating GAB1 and ITGAV. miR-3606-3p-enhancing strategies may have beneficial effects on skin fibrosis through lowing p-AKT/p-ERK activity.
.jpg)
.jpg)
y. chen: None; M. shi: None; W. Wang: None; C. Shi: None; X. Xia: None; w. Wu: None; J. Wang: None; X. Shi: None.
Background/Purpose: Systemic sclerosis (SSc) and keloid are typical skin fibrotic diseases with unclear epigenetic mechanisms and clinical targets. As an important epigenetic regulatory factor, microRNAs play an important role in the occurrence and development of fibrosis in recent studies. This study aimed to assess the role of miR-3606-3p in skin fibrosis and the therapeutic potential.
Methods: The levels of miR-3606-3p were detected in SSc and keloid patients by qPCR and in situ hybridization. RNA-seq, in silico software and luciferase were performed to investigate the targets of miR-3606-3p. The effects of miR-3606-3p, GAB1 and ITGAV on fibroblast fibrogenesis, inflammation and migration were assessed in primary dermal fibroblasts by qPCR, western blotting, wound healing scratch assay. Histology, immunofluorescence analysis and in vivo imaging techniques were used to evaluate the effect of miR-3606-3p on alleviating skin fibrosis in keloid-bearing mice.
Results: MiR-3606-3p was reduced in the skin tissues and fibroblasts from both SSc and keloid patients and negatively correlated with disease severity. RNA-seq analysis and in silico prediction indicated GRB2 associated binding protein 1 (GAB1) and integrin subunit alpha V (ITGAV) were potential targets of miR-3606-3p. We then found that miR-3606-3p downregulated both GAB1 and ITGAV by directly targeting their 3′-UTRs, and further reduced p-AKT and p-ERK activities to inhibit collagen synthesis and NF-κB induced fibroblast inflammation. Furthermore, miR-3606-3p inhibited fibroblast migration in primary fibroblasts and keloid-bearing nude miceby wound healing scratch assay and in vivoimaging techniques respectively. In contrast, GAB1 and ITGAV were upregulated in SSc and keloid patients, and siRNA-mediated GAB1 or ITGAV knockdown replicated the phenotypes observed in miR-3606-3p-overexpressing fibroblasts, including inflammation, migration and fibrogenesis (Figure 1). Finally, by constructing the humanized mouse model of transplanted keloid graft, we found that miR-3606-3p treatment inhibits GAB1 and ITGAV leading to significantly alleviate skin fibrosis (Figure 2).
Conclusion: Our results indicated miR-3606-3p inhibits ECM deposition, inflammation, and migration of fibroblasts by downregulating GAB1 and ITGAV. miR-3606-3p-enhancing strategies may have beneficial effects on skin fibrosis through lowing p-AKT/p-ERK activity.

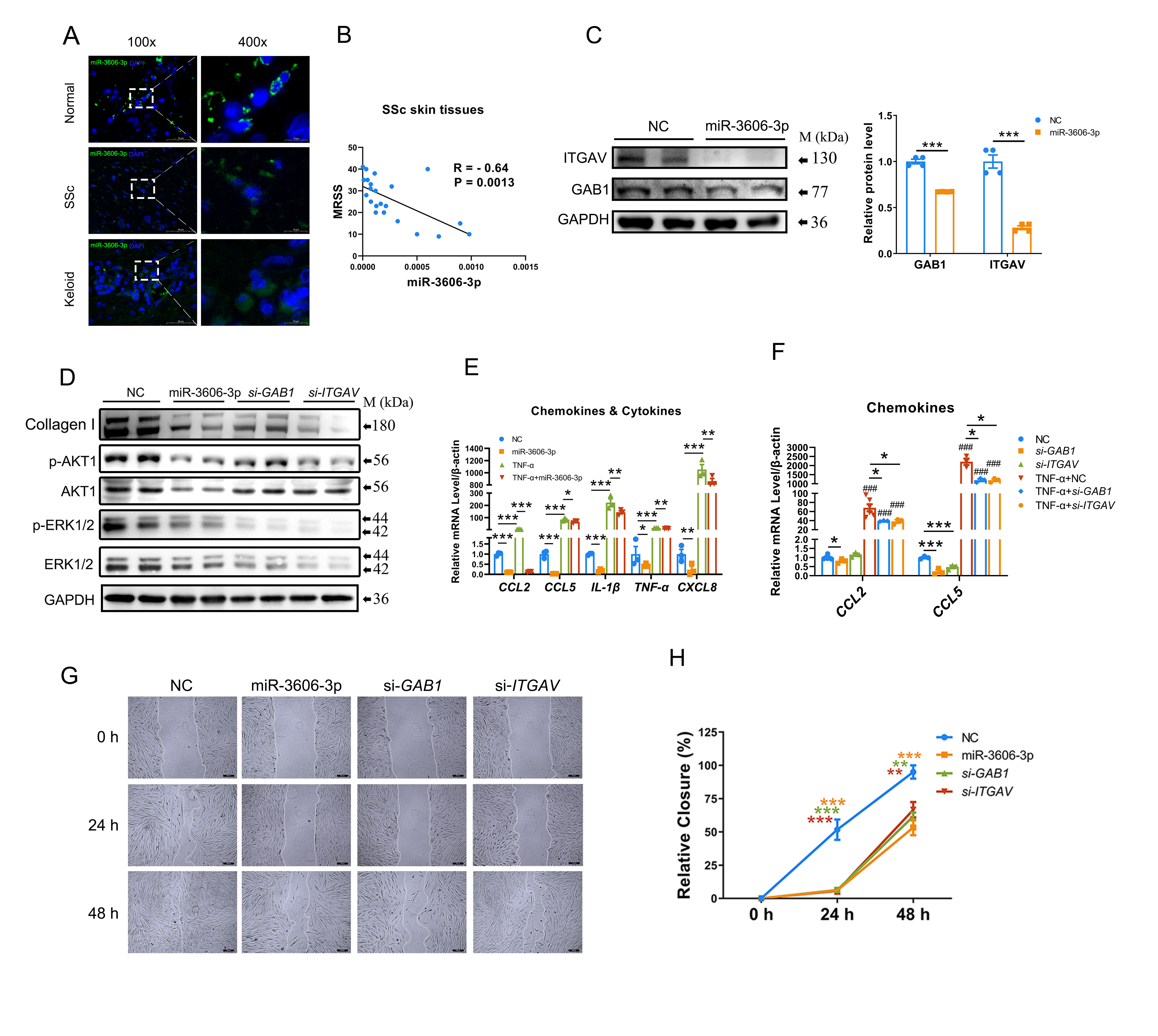
Figure 1. miR-3606-3p decreased in fibrosis skin tissue, while upregulating miR-3606-3p or inhibiting GAB1 and ITGAV supressed collagen production, inflammation and cell migration. (A) miR-3606-3p decreased in fibrosis skin tissue by in situ hybridization. (B) The relationship between MRSS and miR-3606-3p in SSc skin tissues. (C) miR-3606-3p inhibited GAB1 and ITGAV by western blotting. (D) Downregulation of type I collagen, p-AKT, AKT, p-ERK1/2, and ERK1/2 levels in SSc primary fibroblast with NC, miR-3606-3p mimics, si-GAB1 and si-ITGAV. (E) Downregulated chemokines and cytokines in miR-3606-3p overexpressing and TNF-α treated fibroblasts. (F) The effects of GAB1 siRNA and ITGAV siRNA on CCL2 and CCL5 expression in fibroblasts with or without TNF-α treatment. (G) Cell migration assay results by morphology in primary fibroblast with miR-3606-3p overexpression or GAB1 knockdown or ITGAV knockdown. N=3. (H) Relative closure distance of cell migration in fibroblasts with miR-3606-3p overexpression or GAB1 knockdown or ITGAV knockdown. N=3. *P < 0.05; **P < 0.01; ***P < 0.001.
.jpg)
Figure 2. miR-3606-3p treatment inhibits migration of fibroblasts and alleviates skin fibrosis in keloid-bearing mice. (A) Diagram and (B) live imaging of assessing cell migration rate in vivo. N=6. (C) The construction of a keloid-bearing mouse model. (D) Morphological evaluation and (E) quantitative analysis of subcutaneous keloid grafts (5 NC vs. 5 miR-3606-3p). (F) Quantitative analysis of collagen content in Masson’s staining. *P < 0.05; **P < 0.01; ***P < 0.001.
.jpg)
Graphical Abstract. The mechanism of miR-3606-3p on anti-inflammatory and anti-fibrotic effects. ① miR-3606-3p targeted the 3'-UTRs of GAB1 and ITGAV mRNA and subsequently inhibited their protein expression, then attenuated the phosphorylation of AKT and ERK1/2. MiR-3606-3p and knockdown of GAB1 and ITGAV exert an inhibitory effect on inflammation, migration, and collagen deposition as follows: ② Two important negative regulators of fibroblast migration, named ADA1 and NID2, were inhibited by p-AKT/ERK1/2 resulting in collagen deposition and cell migration. ③ p-AKT/ERK1/2 triggered inflammatory responses by activating p-p65 of the NF-κB signalling pathway and releasing the inflammatory factors, including CCL2 and CCL5. Collectively, miR-3606-3p repressed the expression of GAB1, and ITGAV, eventually leading to attenuation of collagen deposition, cell migration and inflammation.
y. chen: None; M. shi: None; W. Wang: None; C. Shi: None; X. Xia: None; w. Wu: None; J. Wang: None; X. Shi: None.



