Poster Session B
Systemic lupus erythematosus (SLE)
Session: (1442–1487) SLE – Diagnosis, Manifestations, & Outcomes Poster II
1465: Blood-dominant Disease in Older-onset Lupus: A Systematic Review and Meta-analysis
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- SA
Sarah Abi Doumeth, MD
Case Western Reserve University/University Hospitals Cleveland Medical Center
Cleveland Heights, OH, United StatesDisclosure information not submitted.
Abstract Poster Presenter(s)
Sarah Abi Doumeth1, Marina Nighat Magrey2 and Omer Pamuk3, 1Case Western Reserve University/University Hospitals Cleveland Medical Center, Cleveland, OH, 2Case Western Reserve University, University Hospitals, Cleveland, OH, 3University Hospitals Cleveland Medical Center, Cleveland, OH
Background/Purpose: Previous studies have shown that the clinical manifestations of systemic lupus erythematosus (SLE) differ based on age of onset. Late onset SLE has been shown to be milder, with lower frequency of lupus nephritis, cutaneous and neuropsychiatric presentations however with more prevalent pulmonary manifestations. There have been multiple retrospective or prospective studies comparing hematological manifestations in early-onset SLE patients (age< 50) with older onset SLE patients (age >50) with varying results. We performed a systematic review and meta-analysis to evaluate the differences in hematologic manifestations (autoimmune hemolytic anemia(AIHA),thrombocytopenia(TP), lymphopenia, leukopenia, lymphadenopathy and thrombosis) in late-onset SLE patients (ltSLE) compared to adult-onset SLE patients (aSLE).
Methods: Literature search was performed using PubMed, Web of Science and Cochrane Library. PRISMA 2020 guidelines and checklist were used. Studies were included if they investigated the frequency of hematological manifestations in ltSLE patients and excluded if they did not include aSLE as control group. The diagnosis of SLE was performed with ACR 1997 revised classification criteria for SLE. We included cohort, case-control, and population-based studies. Two authors independently reviewed all articles and evaluated the data for consistency between the abstracts, tables, and text to avoid a bias. Forest plot was used to compare odds ratios (95% CI) of hematological manifestations by age groups. Study heterogeneity was assessed using I2.All analyses were performed using R Statistical Software meta package (v4.2.1; R Core Team 2022).
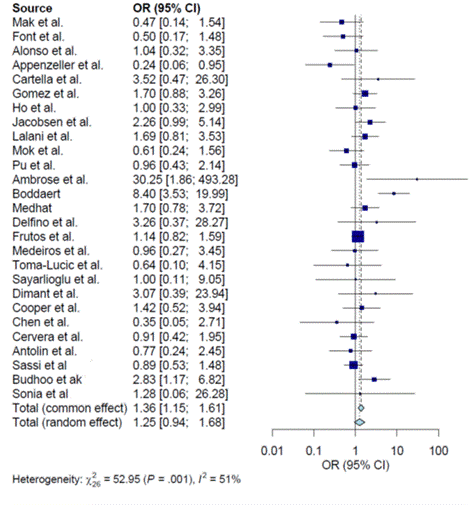
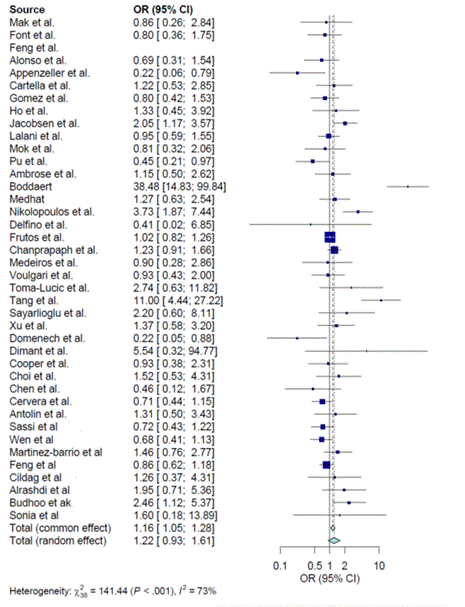
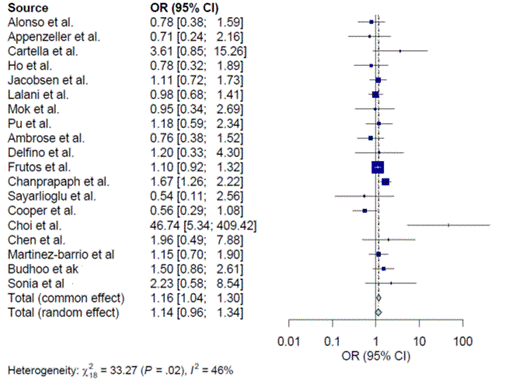
Results: 44 eligible studies comprising 20,508 SLE patients (17421 aSLE and 3087 ltSLE) were included in analysis. Among these studies, 27 reported the occurrence of AIHA which was found to be more frequent in the aSLE group compared to ltSLE (OR: 1.36, 95% CI: 1.15-1.61, p=0.0003) (Figure 1). Further analysis of 40 studies revealed a higher frequency of TP in the aSLE group (OR: 1.16, 95% CI: 1.05-1.28, p=0.0045) (Figure 2). 19 studies provided data on lymphopenia which was found to be more frequent in aSLE (OR: 1.16, 95%CI: 1.04-1.30, p=0.0082) (Figure 3). 31 studies included data for leukopenia and the frequency was higher in the aSLE (OR: 1.28, 95% CI: 1.17-1.41). Additionally, lymphadenopathy was more commonly seen in aSLE group (OR: 2.18, 95%CI: 1.47-3.24, p=0.0001). However, no significant difference was observed in the frequency of thrombosis between the two groups.
Conclusion: Attributing hematological findings to SLE may be challenging in older onset patients due to comorbidities and polypharmacy. In this study, the overall frequencies of AIHA, TP, lymphopenia, leukopenia and lymphadenopathy were more common in aSLE patients compared to ltSLE.
S. Abi Doumeth: None; M. Magrey: AbbVie, 2, Bristol Myers Squibb, 2, Eli Lilly, 2, Novartis, 2, Pfizer Inc, 2, UCB, 5; O. Pamuk: None.
Background/Purpose: Previous studies have shown that the clinical manifestations of systemic lupus erythematosus (SLE) differ based on age of onset. Late onset SLE has been shown to be milder, with lower frequency of lupus nephritis, cutaneous and neuropsychiatric presentations however with more prevalent pulmonary manifestations. There have been multiple retrospective or prospective studies comparing hematological manifestations in early-onset SLE patients (age< 50) with older onset SLE patients (age >50) with varying results. We performed a systematic review and meta-analysis to evaluate the differences in hematologic manifestations (autoimmune hemolytic anemia(AIHA),thrombocytopenia(TP), lymphopenia, leukopenia, lymphadenopathy and thrombosis) in late-onset SLE patients (ltSLE) compared to adult-onset SLE patients (aSLE).
Methods: Literature search was performed using PubMed, Web of Science and Cochrane Library. PRISMA 2020 guidelines and checklist were used. Studies were included if they investigated the frequency of hematological manifestations in ltSLE patients and excluded if they did not include aSLE as control group. The diagnosis of SLE was performed with ACR 1997 revised classification criteria for SLE. We included cohort, case-control, and population-based studies. Two authors independently reviewed all articles and evaluated the data for consistency between the abstracts, tables, and text to avoid a bias. Forest plot was used to compare odds ratios (95% CI) of hematological manifestations by age groups. Study heterogeneity was assessed using I2.All analyses were performed using R Statistical Software meta package (v4.2.1; R Core Team 2022).
Results: 44 eligible studies comprising 20,508 SLE patients (17421 aSLE and 3087 ltSLE) were included in analysis. Among these studies, 27 reported the occurrence of AIHA which was found to be more frequent in the aSLE group compared to ltSLE (OR: 1.36, 95% CI: 1.15-1.61, p=0.0003) (Figure 1). Further analysis of 40 studies revealed a higher frequency of TP in the aSLE group (OR: 1.16, 95% CI: 1.05-1.28, p=0.0045) (Figure 2). 19 studies provided data on lymphopenia which was found to be more frequent in aSLE (OR: 1.16, 95%CI: 1.04-1.30, p=0.0082) (Figure 3). 31 studies included data for leukopenia and the frequency was higher in the aSLE (OR: 1.28, 95% CI: 1.17-1.41). Additionally, lymphadenopathy was more commonly seen in aSLE group (OR: 2.18, 95%CI: 1.47-3.24, p=0.0001). However, no significant difference was observed in the frequency of thrombosis between the two groups.
Conclusion: Attributing hematological findings to SLE may be challenging in older onset patients due to comorbidities and polypharmacy. In this study, the overall frequencies of AIHA, TP, lymphopenia, leukopenia and lymphadenopathy were more common in aSLE patients compared to ltSLE.

Figure 1. Odd ratios for AIHA in early and late onset SLE patients

Figure 2. ORs for TP in early and late onset lupus groups.

Figure 3. ORs for lymphopenia in aSLE and ltSLE patients.
S. Abi Doumeth: None; M. Magrey: AbbVie, 2, Bristol Myers Squibb, 2, Eli Lilly, 2, Novartis, 2, Pfizer Inc, 2, UCB, 5; O. Pamuk: None.



