Poster Session A
Fibrosing rheumatic diseases (scleroderma, MCTD, IgG4-related disease, scleroderma mimics)
Session: (0609–0672) Systemic Sclerosis & Related Disorders – Clinical Poster I: Research
0654: Comparison of Cardiovascular Risk in Patients with Systemic Sclerosis and the General Population
Sunday, November 12, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- MT
Michal Tomcik, MD, PhD
Institute of Rheumatology
Prague, Czech RepublicDisclosure information not submitted.
Abstract Poster Presenter(s)
Sabina Oreska1, Hana Storkanova1, Jaroslav Kudlicka2, Vladimir Tuka2, Ondrej Mikes2, Zdislava Krupickova2, Martin Satny2, Eva Chytilova2, Jan Kvasnicka2, Maja Spiritovic3, Barbora Hermankova4, Petr Cesak5, Marian Rybar6, Karel Pavelka7, Ladislav Senolt8, Radim Becvar9, Jiri Vencovsky1, Michal Vrablik2 and Michal Tomcik1, 1Institute of Rheumatology, Prague, Czech Republic, Department of Rheumatology, 1st Faculty of Medicine, Charles University, Prague, Czech Republic, 23rd Department of Internal Medicine, General University Hospital and 1st Faculty of Medicine, Charles University, Prague, Czech Republic, 3Institute of Rheumatology, Prague, Czech Republic, Department of Physiotherapy, Faculty of Physical Education and Sport, Charles University, Prague, Czech Republic, 4Department of Physiotherapy, Faculty of Physical Education and Sport, Charles University, Prague, Czech Republic, 5Department of Human Movement Laboratory, Faculty of Physical Education and Sport, Charles University, Prague, Czech Republic, 6Department of Biomedical Technology, Faculty of Biomedical Engineering, Czech Technical University in Prague, Kladno, Czech Republic, 7Institut of Rheumatology and Department of Rheumatology, First Faculty of Medicine, Charles University, Praha, Czech Republic, 8Institute of Rheumatology and Department of Rheumatology, First Faculty of Medicine, Praha, Czech Republic, 9Institute of Rheumatology, Prague, Czech Republic, Department of Rheumatology, 1st Faculty of Medicine, Charles University, Praha, Czech Republic
Background/Purpose: Patients with systemic sclerosis (SSc) may be burdened by increased cardiovascular (CV) risk due to accelerated atherosclerosis (ATS) due to systemic inflammation, and vascular impairment. This study aimed to evaluate CV risk in SSc patients SSc compared to healthy controls (HC) and to assess its association with disease-specific features.
Methods: 92 patients with SSc (81 females; mean age 52; mean disease duration 6.8 years; diffuse cutaneous (dc)SSc: n=28, limited cutaneous (lc)SSc: n=64) and 197 HC (147 females, mean age 56.7) were included, all with no history of CV disease (angina pectoris, myocardial infarction, cerebrovascular, and peripheral arterial vascular events). Comorbidities and current treatment were recorded. Disease activity and organ involvement were evaluated in SSc, including lung function tests and skin involvement (by mRSS). All participants underwent examinations of carotid intima-media thickness (CIMT), pulse wave velocity (PWV), ankle-brachial index (ABI), and body composition (by densitometry (DXA) and bioelectrical impedance analysis (BIA)). The risk of fatal CV events was evaluated by the Systematic COronary Risk Evaluation (SCORE, charts for the European population) and its modifications: SCORE multiplied by the coefficient 1.5 (mSCORE), and SCORE2.
Results: SSc patients had a trend to higher prevalence of dyslipidemia (p=0.063) and significantly more often prediabetes (p< 0.001) than HC, but a comparable prevalence of arterial hypertension, diabetes mellitus, and current smoking to HC. Nevertheless, SSc had significantly more frequent use of antihypertensive treatment compared to HC (p< 0.001), including calcium channel blockers (indicated for Raynaud's phenomenon).
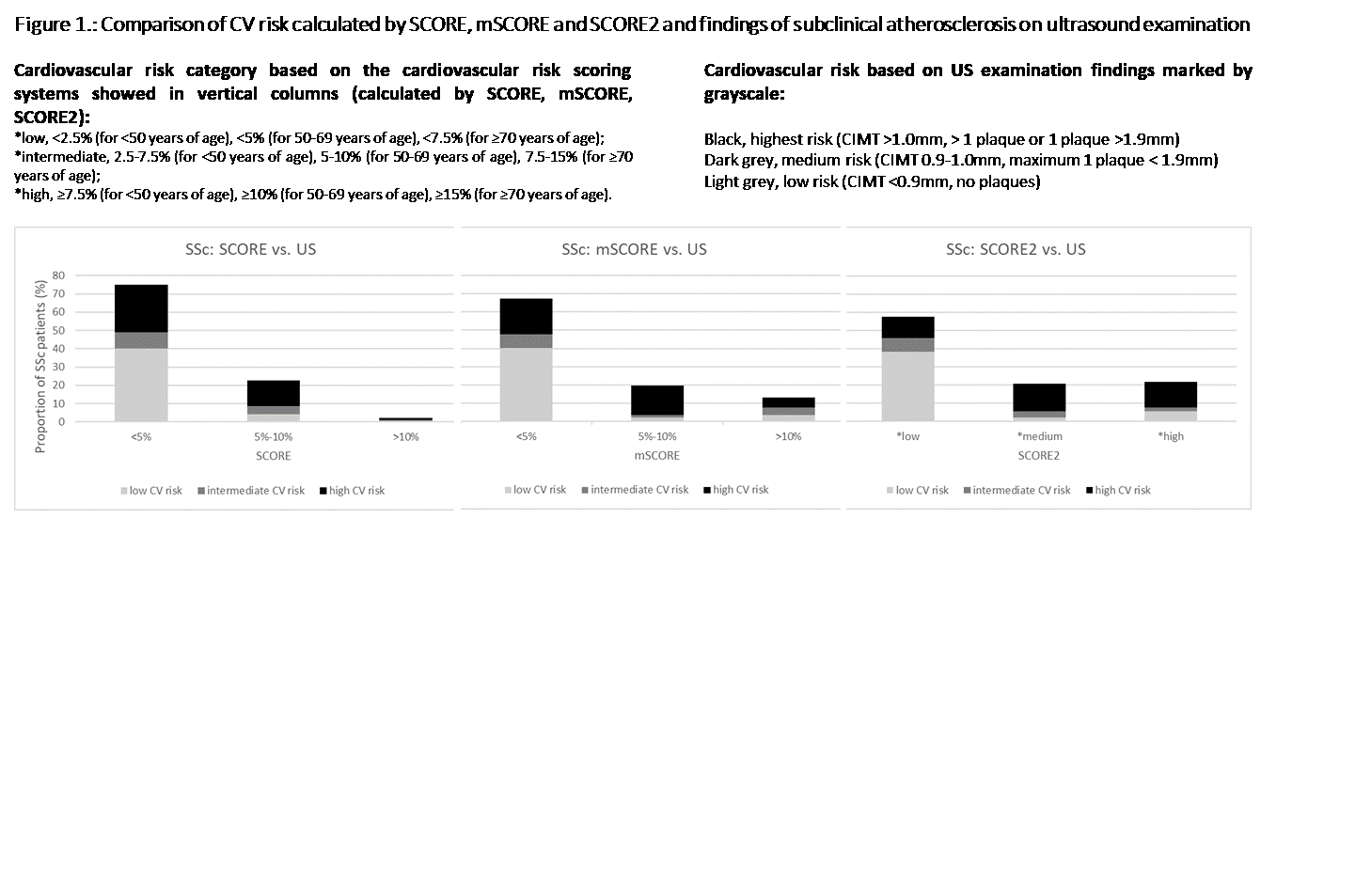
The prevalence of carotid artery disease was significantly increased in SSc compared to HC. SSc had significantly more unfavorable CIMT and ABI (p< 0.05 for both). There was only a trend to lower SCORE and overall CV risk based on SCORE in SSc compared to HC, but no significant difference in SCORE2. On the contrary, the overall CV risk based on US examination showed significantly higher CV risk in SSc. A comparison of CV risk with the findings of subclinical ATS on US examination showed that none of the CV risk scoring systems in SSc was exact in estimating the CV risk (Figure 1). Nevertheless, SCORE2 underestimated the real CV risk significantly less than SCORE (p=0.043), while SCORE2 vs. mSCORE and SCORE vs. mSCORE were comparable. In SSc, the CV risk and markers of subclinical ATS were associated especially with age, HbA1c, disease duration, and mean arterial pressure (p< 0.05 for all).
Conclusion: This cross-sectional case-control study in SSc patients demonstrated a significantly increased risk of subclinical ATS in SSc compared to HC, although there was an opposite trend in CV risk estimated by calculated SCORE. The CV risk in SSc was associated especially with age, disease duration, and HbA1c levels, among others. Scoring systems underestimated the CV risk (when compared to ultrasound findings), while SCORE2 was significantly more accurate than SCORE.
Supported by MHCR (023728; NV18-01-00161A; NU21-01-00146).
S. Oreska: None; H. Storkanova: None; J. Kudlicka: None; V. Tuka: None; O. Mikes: None; Z. Krupickova: None; M. Satny: None; E. Chytilova: None; J. Kvasnicka: None; M. Spiritovic: None; B. Hermankova: None; P. Cesak: None; M. Rybar: None; K. Pavelka: Abbvie, 2, 6, Amgen, 2, 6, Bristol-Myers Squibb(BMS), 2, 6, Egis, 2, 6, MSD, 2, 6, Pfizer, 2, 6, Roche, 2, 6, UCB, 2, 6; L. Senolt: None; R. Becvar: Boehringer-Ingelheim, 2, GlaxoSmithKlein(GSK), 2; J. Vencovsky: Argenx, 2, Eli Lilly, 6, Galapagos, 2, Horizon, 2, Merck, 2; M. Vrablik: None; M. Tomcik: None.
Background/Purpose: Patients with systemic sclerosis (SSc) may be burdened by increased cardiovascular (CV) risk due to accelerated atherosclerosis (ATS) due to systemic inflammation, and vascular impairment. This study aimed to evaluate CV risk in SSc patients SSc compared to healthy controls (HC) and to assess its association with disease-specific features.
Methods: 92 patients with SSc (81 females; mean age 52; mean disease duration 6.8 years; diffuse cutaneous (dc)SSc: n=28, limited cutaneous (lc)SSc: n=64) and 197 HC (147 females, mean age 56.7) were included, all with no history of CV disease (angina pectoris, myocardial infarction, cerebrovascular, and peripheral arterial vascular events). Comorbidities and current treatment were recorded. Disease activity and organ involvement were evaluated in SSc, including lung function tests and skin involvement (by mRSS). All participants underwent examinations of carotid intima-media thickness (CIMT), pulse wave velocity (PWV), ankle-brachial index (ABI), and body composition (by densitometry (DXA) and bioelectrical impedance analysis (BIA)). The risk of fatal CV events was evaluated by the Systematic COronary Risk Evaluation (SCORE, charts for the European population) and its modifications: SCORE multiplied by the coefficient 1.5 (mSCORE), and SCORE2.
Results: SSc patients had a trend to higher prevalence of dyslipidemia (p=0.063) and significantly more often prediabetes (p< 0.001) than HC, but a comparable prevalence of arterial hypertension, diabetes mellitus, and current smoking to HC. Nevertheless, SSc had significantly more frequent use of antihypertensive treatment compared to HC (p< 0.001), including calcium channel blockers (indicated for Raynaud's phenomenon).
The prevalence of carotid artery disease was significantly increased in SSc compared to HC. SSc had significantly more unfavorable CIMT and ABI (p< 0.05 for both). There was only a trend to lower SCORE and overall CV risk based on SCORE in SSc compared to HC, but no significant difference in SCORE2. On the contrary, the overall CV risk based on US examination showed significantly higher CV risk in SSc. A comparison of CV risk with the findings of subclinical ATS on US examination showed that none of the CV risk scoring systems in SSc was exact in estimating the CV risk (Figure 1). Nevertheless, SCORE2 underestimated the real CV risk significantly less than SCORE (p=0.043), while SCORE2 vs. mSCORE and SCORE vs. mSCORE were comparable. In SSc, the CV risk and markers of subclinical ATS were associated especially with age, HbA1c, disease duration, and mean arterial pressure (p< 0.05 for all).
Conclusion: This cross-sectional case-control study in SSc patients demonstrated a significantly increased risk of subclinical ATS in SSc compared to HC, although there was an opposite trend in CV risk estimated by calculated SCORE. The CV risk in SSc was associated especially with age, disease duration, and HbA1c levels, among others. Scoring systems underestimated the CV risk (when compared to ultrasound findings), while SCORE2 was significantly more accurate than SCORE.
Supported by MHCR (023728; NV18-01-00161A; NU21-01-00146).

Figure 1.: Comparison of CV risk calculated by SCORE, mSCORE and SCORE2 and findings of subclinical atherosclerosis on ultrasound examination
S. Oreska: None; H. Storkanova: None; J. Kudlicka: None; V. Tuka: None; O. Mikes: None; Z. Krupickova: None; M. Satny: None; E. Chytilova: None; J. Kvasnicka: None; M. Spiritovic: None; B. Hermankova: None; P. Cesak: None; M. Rybar: None; K. Pavelka: Abbvie, 2, 6, Amgen, 2, 6, Bristol-Myers Squibb(BMS), 2, 6, Egis, 2, 6, MSD, 2, 6, Pfizer, 2, 6, Roche, 2, 6, UCB, 2, 6; L. Senolt: None; R. Becvar: Boehringer-Ingelheim, 2, GlaxoSmithKlein(GSK), 2; J. Vencovsky: Argenx, 2, Eli Lilly, 6, Galapagos, 2, Horizon, 2, Merck, 2; M. Vrablik: None; M. Tomcik: None.



