Poster Session A
Fibrosing rheumatic diseases (scleroderma, MCTD, IgG4-related disease, scleroderma mimics)
Session: (0609–0672) Systemic Sclerosis & Related Disorders – Clinical Poster I: Research
0633: Prediction of Progressive Fibrosing Interstitial Lung Disease in Systemic Sclerosis Patients: Insight from the CRDC Cohort Study
Sunday, November 12, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- MH
Min Hui, MD
Department of Rheumatology, Peking Union Medical College Hospital
Beijing, ChinaDisclosure information not submitted.
Abstract Poster Presenter(s)
Min Hui1, Xinwang Duan2, Jiaxin Zhou3, Mengtao Li3, Qian Wang4, Jiuliang Zhao1, Yong Hou1, Dong Xu5 and xiaofeng Zeng4, 1Department of Rheumatology, Peking Union Medical College Hospital, Beijing, China, 2Department of Rheumatology, The Second Affiliated Hospital of Nanchang University, Beijing, China, 3Peking Union Medical College Hospital, Beijing, China, 4Department of Rheumatology, Peking Union Medical College Hospital, Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing, China, 5Department of Rheumatology, Peking Union Medical College, Beijing, China
Background/Purpose: Systemic sclerosis (SSc) patients can develop progressive fibrosing interstitial lung disease (PF-ILD), linked to a poor outcome. This study aims to establish a reliable prediction model of PF-ILD in SSc-ILD patients, to achieve early risk stratification, and to help better preventing disease progression.
Methods: Three hundred and four SSc-ILD patients registered on Chinese Rheumatism Data Center (CRDC) database since January 2008, with no less than three pulmonary function tests within 6-24 months, were included. The major outcome was development of PF-ILD, which was defined as an absolute annualized forced vital capacity (FVC) decline ≥5% predicted. We collected data at baseline and compared differences between SSc patients with PF-ILD (SSc PF-ILD) group and SSc patients without PF-ILD (SSc non-PF-ILD) group. Lasso regularization regression was performed for further screening. Multivariable Cox regression were used to construct the prediction model, which were presented as nomogram and forest plot.
Results: SSc-ILD patients were divided into SSc PF-ILD group (n=154) and SSc non-PF-ILD group (n=150). Compared with SSc non-PF-ILD group patients at baseline, SSc PF-ILD patients were at older age (48.5±11.9 years vs 44.9±11.3 years, p< 0.001), had more male patients (9.7% vs 6.0%, p=0.012), more diffused SSc (dcSSc) subtype (58.4% vs 32.7%, p< 0.001), and a significant higher incidence of hyperlipidemia (31.2% vs 8.7%, p< 0.001), smoking history (18.2% vs 5.3%, p< 0.001), arthritis (38.3% vs 24.7%, p< 0.001), shortness of breath (84.4% vs 80.0%, p< 0.001) and anti Scl-70 antibody positivity (53.2% vs 40.0%, p< 0.001), as well as more serum IgA deficiency (11.0% vs 5.3%, p< 0.001). The use of cyclophosphamide (CYC) and/or mycophenolate mofetil (MMF) were less common in SSc PF-ILD group compared with SSc non-PF-ILD group (58.4% vs 68.7%, p< 0.001). Based on the results of univariable Cox analysis and Lasso regularization regression, a 9-variable prediction model was constructed, including age≥50 years, hyperlipidemia, smoking history, dcSSc subtype, arthritis, shortness of breath, serum IgA deficiency, positive anti-Scl70 antibody and usage of CYC/MMF. C-index for the model was 0.874, while the Brier scores were 0.144 after bootstrap resampling internal validation.
Conclusion: This study developed the first prediction model for PF-ILD in SSc-ILD patients based on data from CRDC database, and internal validation showed favorable accuracy and stability of the model.
.jpg)
.jpg)
M. Hui: None; X. Duan: None; J. Zhou: None; M. Li: None; Q. Wang: None; J. Zhao: None; Y. Hou: None; D. Xu: None; x. Zeng: None.
Background/Purpose: Systemic sclerosis (SSc) patients can develop progressive fibrosing interstitial lung disease (PF-ILD), linked to a poor outcome. This study aims to establish a reliable prediction model of PF-ILD in SSc-ILD patients, to achieve early risk stratification, and to help better preventing disease progression.
Methods: Three hundred and four SSc-ILD patients registered on Chinese Rheumatism Data Center (CRDC) database since January 2008, with no less than three pulmonary function tests within 6-24 months, were included. The major outcome was development of PF-ILD, which was defined as an absolute annualized forced vital capacity (FVC) decline ≥5% predicted. We collected data at baseline and compared differences between SSc patients with PF-ILD (SSc PF-ILD) group and SSc patients without PF-ILD (SSc non-PF-ILD) group. Lasso regularization regression was performed for further screening. Multivariable Cox regression were used to construct the prediction model, which were presented as nomogram and forest plot.
Results: SSc-ILD patients were divided into SSc PF-ILD group (n=154) and SSc non-PF-ILD group (n=150). Compared with SSc non-PF-ILD group patients at baseline, SSc PF-ILD patients were at older age (48.5±11.9 years vs 44.9±11.3 years, p< 0.001), had more male patients (9.7% vs 6.0%, p=0.012), more diffused SSc (dcSSc) subtype (58.4% vs 32.7%, p< 0.001), and a significant higher incidence of hyperlipidemia (31.2% vs 8.7%, p< 0.001), smoking history (18.2% vs 5.3%, p< 0.001), arthritis (38.3% vs 24.7%, p< 0.001), shortness of breath (84.4% vs 80.0%, p< 0.001) and anti Scl-70 antibody positivity (53.2% vs 40.0%, p< 0.001), as well as more serum IgA deficiency (11.0% vs 5.3%, p< 0.001). The use of cyclophosphamide (CYC) and/or mycophenolate mofetil (MMF) were less common in SSc PF-ILD group compared with SSc non-PF-ILD group (58.4% vs 68.7%, p< 0.001). Based on the results of univariable Cox analysis and Lasso regularization regression, a 9-variable prediction model was constructed, including age≥50 years, hyperlipidemia, smoking history, dcSSc subtype, arthritis, shortness of breath, serum IgA deficiency, positive anti-Scl70 antibody and usage of CYC/MMF. C-index for the model was 0.874, while the Brier scores were 0.144 after bootstrap resampling internal validation.
Conclusion: This study developed the first prediction model for PF-ILD in SSc-ILD patients based on data from CRDC database, and internal validation showed favorable accuracy and stability of the model.

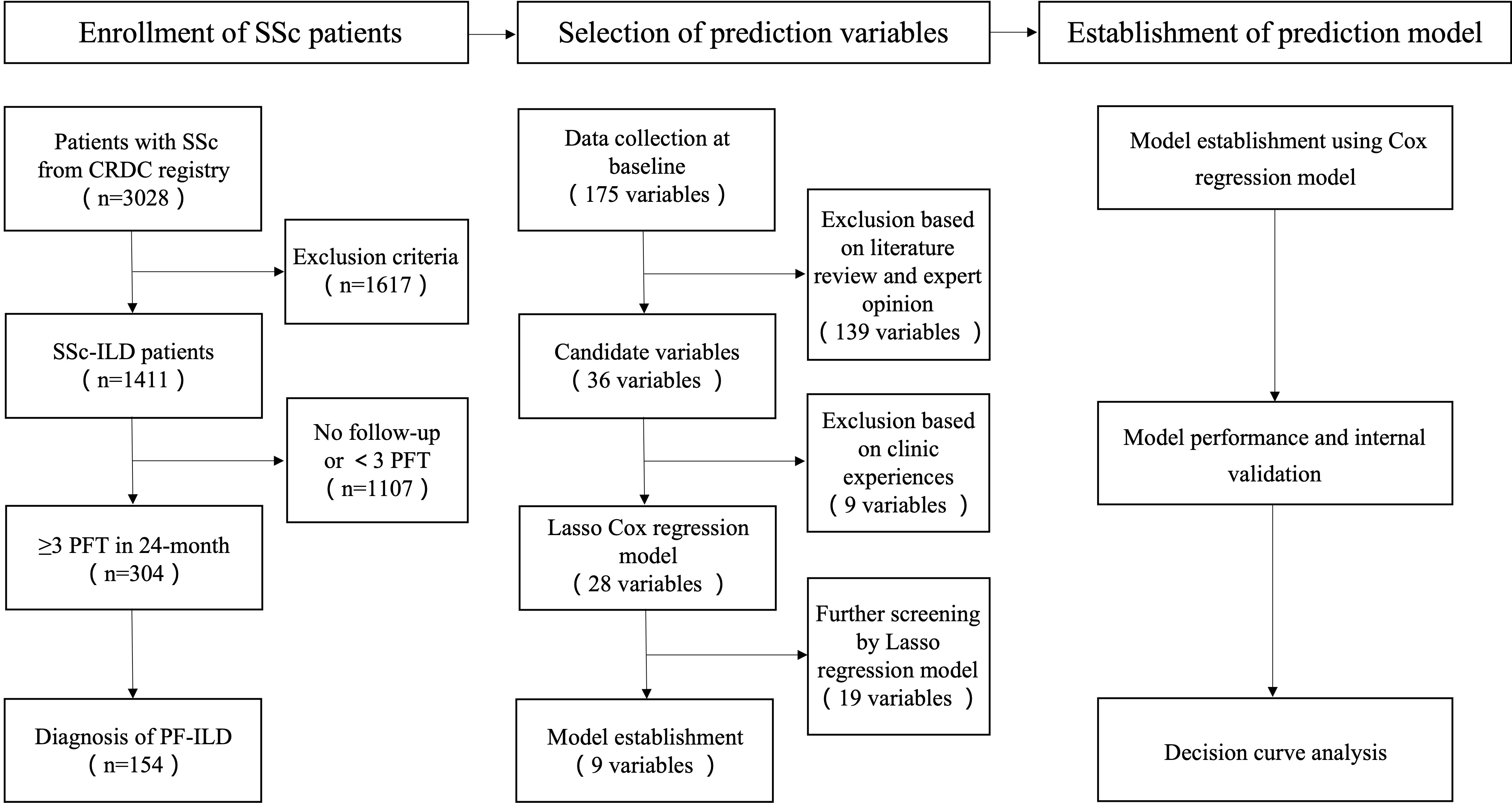
Flow chart showing the study design
.jpg)
Baseline demographic and clinical characteristics of the SSc-ILD patients analyzed for PF-ILD risk in univariate Cox proportional hazards regression analysis
.jpg)
Nomogram predicting the probability that a systemic sclerosis patient with interstitial lung disease (ILD) will develop PF-ILD
M. Hui: None; X. Duan: None; J. Zhou: None; M. Li: None; Q. Wang: None; J. Zhao: None; Y. Hou: None; D. Xu: None; x. Zeng: None.



