Poster Session A
Rheumatoid arthritis (RA)
Session: (0380–0422) RA – Diagnosis, Manifestations, and Outcomes Poster I
0403: Disease Activity Is Associated with Frailty in Veterans with Rheumatoid Arthritis
Sunday, November 12, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- CL
Courtney Loecker, MSN, NP, APRN
University of Nebraska
Lincoln, NE, United StatesDisclosure information not submitted.
Abstract Poster Presenter(s)
Courtney Loecker1, Bryant England2, Punyasha Roul2, Namrata Singh3, Kaleb Michaud2, Lani Zimmerman4, Myra Schmaderer4, Grant Cannon5, Ted R Mikuls6, Gary Kunkel7, Ariela Orkaby8, Joshua Baker9 and K Wysham10, 1University of Nebraska Medical Center;VA Nebraska-Western Iowa Health Care System, Lincoln, NE, 2University of Nebraska Medical Center, Omaha, NE, 3University of Washington, Bellevue, WA, 4University of Nebraska Medical Center, Lincoln, NE, 5University of Utah and Salt Lake City VA, Salt Lake City, UT, 6Division of Rheumatology and Immunology, University of Nebraska Medical Center, Omaha, NE, 7VA Salt Lake City & University of Utah, Salt Lake City, UT, 8Veterans Affairs Boston Healthcare System & Brigham and Women’s Hospital, Harvard Medical School, Boston, MA; VA Geriatric Research Education and Clinical Center, Boston, MA, 9University of Pennsylvania, Philadelphia, PA, 10VA Puget Sound/University of Washington, Seattle, WA
Background/Purpose: Frailty, defined as an increased vulnerability to stressors and adverse health outcomes, is an emerging concept in RA. Active RA disease gives rise to inflammation, pain, and joint damage leading to functional impairment and morbidity, which cumulatively influences frailty status. However, the association between frailty and RA disease activity is incompletely understood. Given that RA disease activity may impact frailty status but could also be confounded by other health factors, we examined the relationship of disease activity and frailty in a large RA cohort with robust co-variable adjustment.
Methods: A cross-sectional descriptive study was performed on baseline data from the VA Rheumatoid Arthritis (VARA) Registry, a multi-center prospective cohort which began enrolling in January 2003. All participants met ACR criteria for RA. Frailty was measured using the 31-item VA-Frailty Index (VA-FI) which includes diagnostic and procedure codes linked to health-related deficits encompassing morbidity, functional status, cognition and mood, sensory impairment, and other geriatric syndromes from the 3 years prior to enrollment. The VA-FI is a ratio of all deficits and ranges from 0 to 1 with scores >0.2 considered frail. RA disease activity was measured during routine clinical care using the DAS28-ESR. Multivariable logistic regression was used to evaluate the association between frailty and disease activity adjusting for age, sex, disease duration, smoking status, BMI, prednisone use, conventional synthetic DMARD use, and biologic DMARD use, obtained from the registry and linked VA data. Due to collinearity the Rheumatic Disease Comorbidity Index (RDCI) and MDHAQ were not included in the multivariable model.
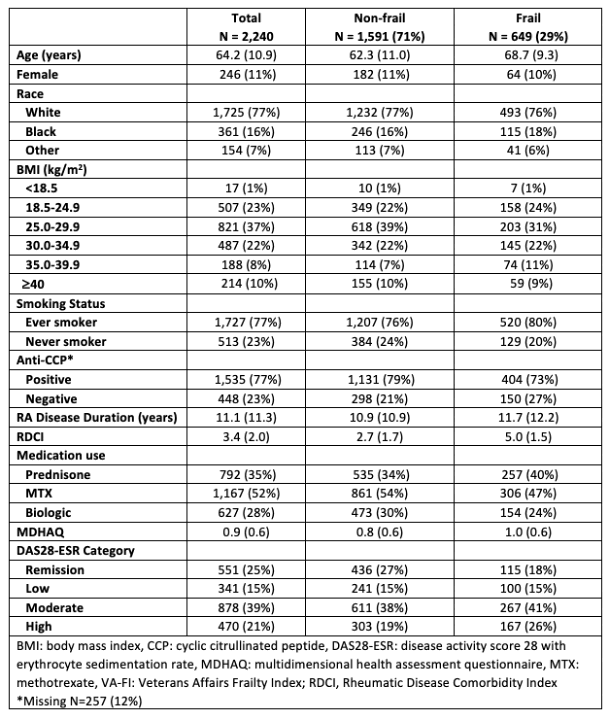
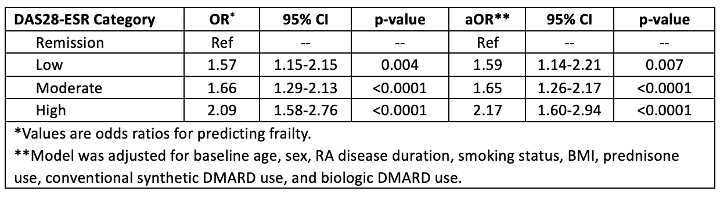
Results: Of the 2,240 participants studied, 89% were male, mean age was 64.2±10.9 years, mean RA disease duration was 11.1±11.3 years, majority were White (77%), and had moderate RA disease activity (39%). Frailty was observed in 29% of participants at enrollment. Those categorized as frail were older (68.7 vs. 62.3 years), had longer RA disease duration (11.7 vs. 10.9 years), had higher RDCI scores (5.0 vs. 2.7), and higher MDHAQ scores (1.0 vs. 0.8) compared to non-frail participants (Table 1). In the multivariable model, with remission as the reference group, RA disease activity was significantly associated with frailty with the following odds ratios: low disease activity 1.59 (95% CI 1.14-2.21), moderate disease activity 1.65 (95% CI 1.26-2.17) and high disease activity 2.17 (95% CI 1.60-2.94) (p-values all < 0.01) (Table 2). These associations were not attenuated in the adjusted model.
Conclusion: RA disease activity has a strong, independent association with frailty in Veterans with RA. Point estimates remained consistent between unadjusted and adjusted models suggesting a robust association. Future studies evaluating the longitudinal relationship between these two measures are needed to understand the causal relationships underlying this association and to determine if improving disease activity can impact frailty status.
C. Loecker: None; B. England: Boehringer-Ingelheim, 2, 5; P. Roul: None; N. Singh: None; K. Michaud: None; L. Zimmerman: None; M. Schmaderer: None; G. Cannon: None; T. Mikuls: Elsevier, 9, Horizon Therapeutics, 2, 5, Pfizer, 2, Sanofi, 2, UCB Pharma, 2, Wolters Kluwer Health (UpToDate), 9; G. Kunkel: None; A. Orkaby: Anthos therapeutics, 2; J. Baker: Bristol-Myers Squibb(BMS), 2, Burns-White, LLC, 2, CorEvitas, LLC, 2, Pfizer, 2; K. Wysham: None.
Background/Purpose: Frailty, defined as an increased vulnerability to stressors and adverse health outcomes, is an emerging concept in RA. Active RA disease gives rise to inflammation, pain, and joint damage leading to functional impairment and morbidity, which cumulatively influences frailty status. However, the association between frailty and RA disease activity is incompletely understood. Given that RA disease activity may impact frailty status but could also be confounded by other health factors, we examined the relationship of disease activity and frailty in a large RA cohort with robust co-variable adjustment.
Methods: A cross-sectional descriptive study was performed on baseline data from the VA Rheumatoid Arthritis (VARA) Registry, a multi-center prospective cohort which began enrolling in January 2003. All participants met ACR criteria for RA. Frailty was measured using the 31-item VA-Frailty Index (VA-FI) which includes diagnostic and procedure codes linked to health-related deficits encompassing morbidity, functional status, cognition and mood, sensory impairment, and other geriatric syndromes from the 3 years prior to enrollment. The VA-FI is a ratio of all deficits and ranges from 0 to 1 with scores >0.2 considered frail. RA disease activity was measured during routine clinical care using the DAS28-ESR. Multivariable logistic regression was used to evaluate the association between frailty and disease activity adjusting for age, sex, disease duration, smoking status, BMI, prednisone use, conventional synthetic DMARD use, and biologic DMARD use, obtained from the registry and linked VA data. Due to collinearity the Rheumatic Disease Comorbidity Index (RDCI) and MDHAQ were not included in the multivariable model.
Results: Of the 2,240 participants studied, 89% were male, mean age was 64.2±10.9 years, mean RA disease duration was 11.1±11.3 years, majority were White (77%), and had moderate RA disease activity (39%). Frailty was observed in 29% of participants at enrollment. Those categorized as frail were older (68.7 vs. 62.3 years), had longer RA disease duration (11.7 vs. 10.9 years), had higher RDCI scores (5.0 vs. 2.7), and higher MDHAQ scores (1.0 vs. 0.8) compared to non-frail participants (Table 1). In the multivariable model, with remission as the reference group, RA disease activity was significantly associated with frailty with the following odds ratios: low disease activity 1.59 (95% CI 1.14-2.21), moderate disease activity 1.65 (95% CI 1.26-2.17) and high disease activity 2.17 (95% CI 1.60-2.94) (p-values all < 0.01) (Table 2). These associations were not attenuated in the adjusted model.
Conclusion: RA disease activity has a strong, independent association with frailty in Veterans with RA. Point estimates remained consistent between unadjusted and adjusted models suggesting a robust association. Future studies evaluating the longitudinal relationship between these two measures are needed to understand the causal relationships underlying this association and to determine if improving disease activity can impact frailty status.

Table 1. Characteristics of the whole cohort and by frailty status measured by the VA Frailty Index. Reported as N (%) or mean (SD).

Table 2. Unadjusted (N=2,240) and adjusted (N=2,186) logistic regression models evaluating the relationship between frailty and RA disease activity.
C. Loecker: None; B. England: Boehringer-Ingelheim, 2, 5; P. Roul: None; N. Singh: None; K. Michaud: None; L. Zimmerman: None; M. Schmaderer: None; G. Cannon: None; T. Mikuls: Elsevier, 9, Horizon Therapeutics, 2, 5, Pfizer, 2, Sanofi, 2, UCB Pharma, 2, Wolters Kluwer Health (UpToDate), 9; G. Kunkel: None; A. Orkaby: Anthos therapeutics, 2; J. Baker: Bristol-Myers Squibb(BMS), 2, Burns-White, LLC, 2, CorEvitas, LLC, 2, Pfizer, 2; K. Wysham: None.



