Poster Session A
Myopathic rheumatic diseases (polymyositis, dermatomyositis, inclusion body myositis)
Session: (0283–0307) Muscle Biology, Myositis & Myopathies – Basic & Clinical Science Poster I
0305: Prevalence and Clinical Significance of anti-Ro52 Antibodies in Antisynthetase Syndrome
Sunday, November 12, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- JN
Javier Narvaez, MD, PhD
Hospital Universitario de Bellvitge
Barcelona, SpainDisclosure information not submitted.
Abstract Poster Presenter(s)
Javier Narvaez1, Paola Vidal-Montal2, Elena Cañadillas-Sanchez3, Pol Maymó2, Judith Palacios2, Martí Aguilar2, Montserrat Roig2 and Joan Miquel Nolla2, 1Hospital Universitario de Bellvitge, Barcelona, Spain, 2Department of Rheumatology, Hospital Universitario de Bellvitge, Barcelona, Spain, 3Department of Rheumatology, Hospital Clínico Universitario Lozano Blesa, Zaragoza, Spain
Background/Purpose: Antisynthetase syndrome (ASSD) is a systemic autoimmune condition characterized by the positivity of anti-aminoacyl-transfer-RNA synthetases antibodies (ARS) and the occurrence of the classic triad, encompassing myositis, arthritis, and interstitial lung disease (ILD).
There is a higher prevalence and increased severity of ILD in patients with ASSD compared to other idiopathic inflammatory myopathies (IIM). The leading prognostic role of ILD in ASSD prompted a focused search for laboratory markers able to predict lung involvement occurrence and progression. ARS specificities have been associated with phenotypically distinct subgroups at disease onset. However, it doesn't seem to be significant differences among the groups in the clinical spectrum, time course and prognosis.
Anti-Ro52 antibodies (anti-Ro52) are systemic autoantibodies addressed against the Tripartite motif-containing protein 21 found in several connective tissue diseases and up to 50% of ASSD patients. In patients with other IIM, anti-Ro52 positivity has been associated with a rapid progression (RP) of ILD and a poorer prognosis, whereas its role in ASSD is still uncertain. Our objective was to to assess the prevalence and clinical significance of anti-Ro52 antibodies in a cohort of patients with ASSD.
Methods: Ambispective analysis of clinical, imaging and laboratory characteristics, therapeutic approaches, and outcome of 56 ASSD patients progressively enrolled at our hospital.
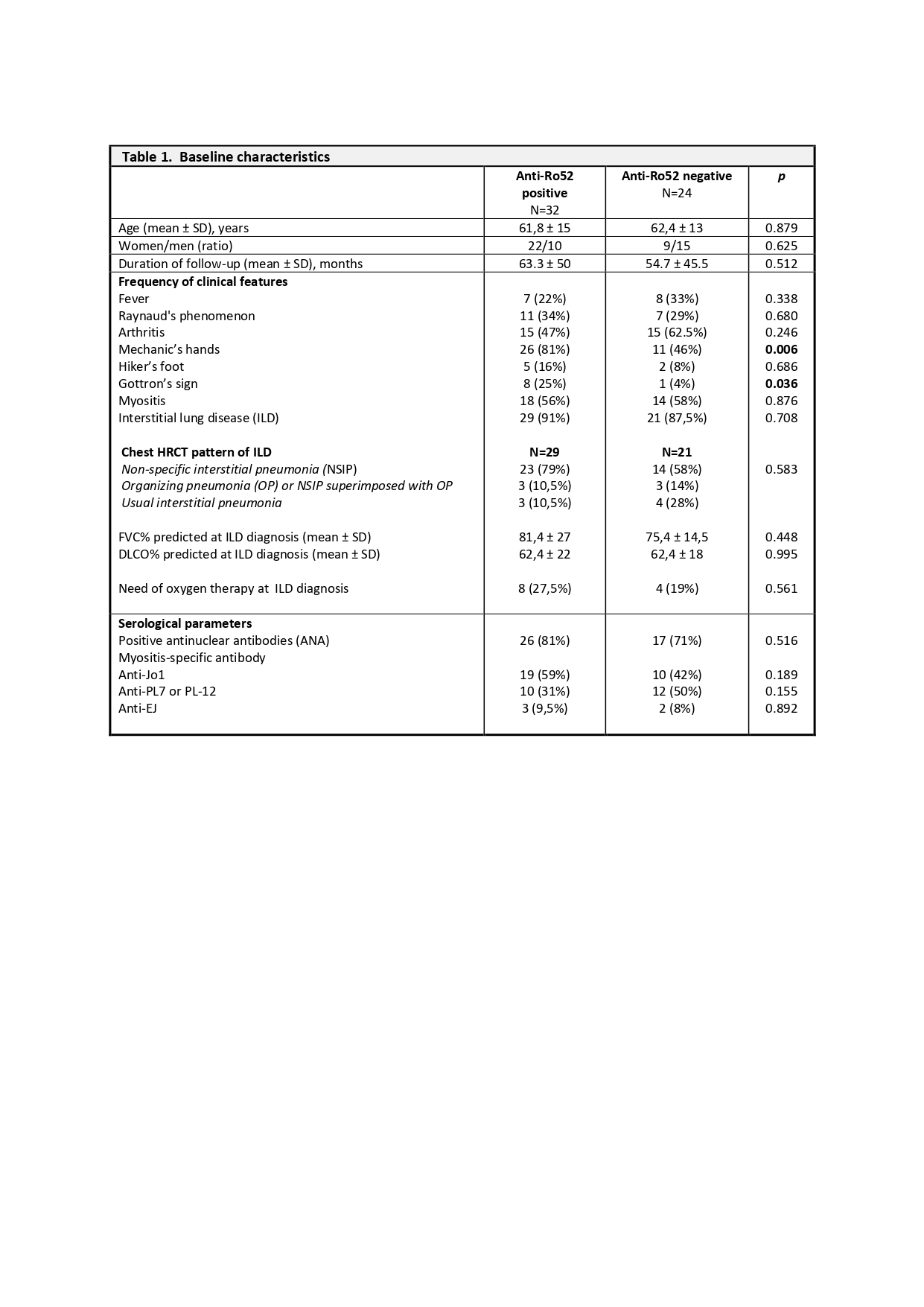
Results: We identified 32 anti-Ro52 positive and 24 anti-Ro negative ASSD patients. The prevalence of ILD and myositis at baseline were similar between the two groups. In contrast, some skin lesions (mechanic's hands and Gottron's papules/sign) were significantly more prevalent in anti-Ro52+, whereas arthritis was more frequently seen in anti-Ro negative patients (see Table 1). We did not observe a strong association of co-occurring anti-Ro52 antibodies with any of the ARS.
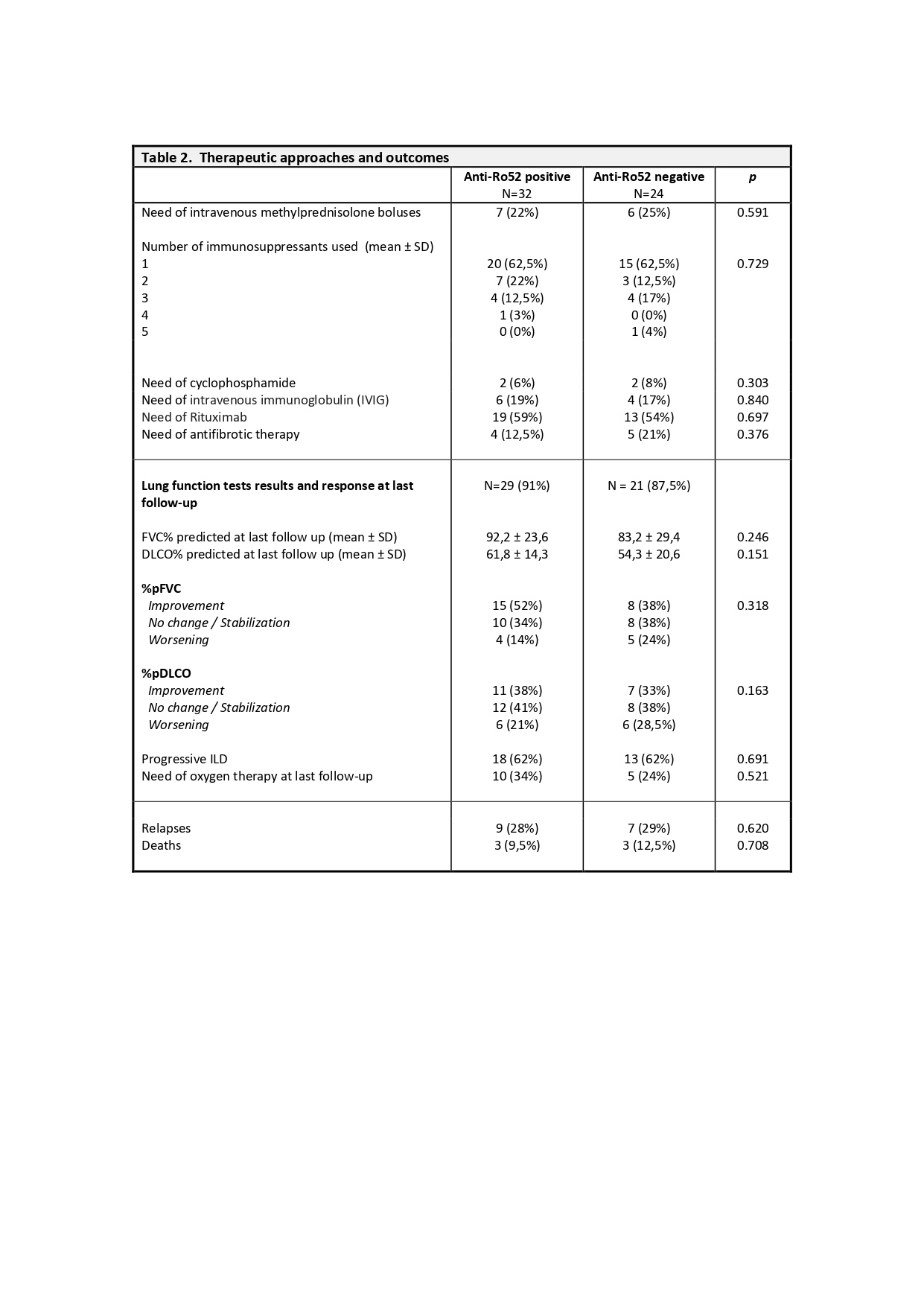
No differences in oxygen need and ILD patterns, therapeutic approaches, outcome measures, and prognosis were observed (Table 2). Overall mortality was 11% (6 subjects). No differences in mortality, overall and disease-related, between anti-Ro52+ and anti-Ro52- patients were observed. Survival curves were not different at any time point (Log-rank test, p-value 0.608).
Conclusion: Overall, the presence of anti-Ro52 antibodies seems to be related to a higher prevalence of skin lesions, but not with ILD. Although they could affect the clinical characteristics of ASSD, they do not seem to influence the prognosis. No differences in relapses, RP-ILD, or mortality were observed when compared to anti-Ro52 negative patients
J. Narvaez: None; P. Vidal-Montal: None; E. Cañadillas-Sanchez: None; P. Maymó: None; J. Palacios: None; M. Aguilar: None; M. Roig: None; J. Nolla: None.
Background/Purpose: Antisynthetase syndrome (ASSD) is a systemic autoimmune condition characterized by the positivity of anti-aminoacyl-transfer-RNA synthetases antibodies (ARS) and the occurrence of the classic triad, encompassing myositis, arthritis, and interstitial lung disease (ILD).
There is a higher prevalence and increased severity of ILD in patients with ASSD compared to other idiopathic inflammatory myopathies (IIM). The leading prognostic role of ILD in ASSD prompted a focused search for laboratory markers able to predict lung involvement occurrence and progression. ARS specificities have been associated with phenotypically distinct subgroups at disease onset. However, it doesn't seem to be significant differences among the groups in the clinical spectrum, time course and prognosis.
Anti-Ro52 antibodies (anti-Ro52) are systemic autoantibodies addressed against the Tripartite motif-containing protein 21 found in several connective tissue diseases and up to 50% of ASSD patients. In patients with other IIM, anti-Ro52 positivity has been associated with a rapid progression (RP) of ILD and a poorer prognosis, whereas its role in ASSD is still uncertain. Our objective was to to assess the prevalence and clinical significance of anti-Ro52 antibodies in a cohort of patients with ASSD.
Methods: Ambispective analysis of clinical, imaging and laboratory characteristics, therapeutic approaches, and outcome of 56 ASSD patients progressively enrolled at our hospital.
Results: We identified 32 anti-Ro52 positive and 24 anti-Ro negative ASSD patients. The prevalence of ILD and myositis at baseline were similar between the two groups. In contrast, some skin lesions (mechanic's hands and Gottron's papules/sign) were significantly more prevalent in anti-Ro52+, whereas arthritis was more frequently seen in anti-Ro negative patients (see Table 1). We did not observe a strong association of co-occurring anti-Ro52 antibodies with any of the ARS.
No differences in oxygen need and ILD patterns, therapeutic approaches, outcome measures, and prognosis were observed (Table 2). Overall mortality was 11% (6 subjects). No differences in mortality, overall and disease-related, between anti-Ro52+ and anti-Ro52- patients were observed. Survival curves were not different at any time point (Log-rank test, p-value 0.608).
Conclusion: Overall, the presence of anti-Ro52 antibodies seems to be related to a higher prevalence of skin lesions, but not with ILD. Although they could affect the clinical characteristics of ASSD, they do not seem to influence the prognosis. No differences in relapses, RP-ILD, or mortality were observed when compared to anti-Ro52 negative patients


J. Narvaez: None; P. Vidal-Montal: None; E. Cañadillas-Sanchez: None; P. Maymó: None; J. Palacios: None; M. Aguilar: None; M. Roig: None; J. Nolla: None.



