Poster Session A
Epidemiology, health policy and outcomes
0333: Ankylosing Spondylitis Patient Perspective on Living with Flares and Impact on Quality of Life
- EL
Elizabeth Luce, BS
MyHealthTeam
San Francisco, CA, United StatesDisclosure information not submitted.
Abstract Poster Presenter(s)
Background/Purpose: Ankylosing spondylitis (AS) leads to symptoms of pain, stiffness, swelling, and fatigue. Patients often report periods of increased symptoms (flares) followed by remission.The purpose of this study was to assess the experience of flares on quality of life from the patient perspective. Improved understanding of the experience of flares may contribute to better treatment and health outcomes.
Methods: In July 2022 an email invitation to an online survey was sent to members of MySpondylitisTeam, a social network of over 88,000 people. 253 members who self-report a doctor's diagnosis of ankylosing spondylitis (AS) completed the 25-question survey.
Results: 94% of members agreed that AS affects their quality of life and 87% agreed that AS makes it hard to do everyday activities. When asked to select the statement that best reflects flare activity in their AS, 44% selected "I have periods of increased symptoms (flares) on and off" and 43% selected "I have flares almost all the time." (Figure 1) Patients with almost constant flares indicated lower quality of life across a number of measures when compared with those whose flares were "on and off". Significant differences were evident for:
- Negatively affected their relationships with family (79% flares "almost all the time" vs. 48% flares "on and off")
- Made them feel isolated or alone (83% vs. 59%)
- Negatively affected their ability to have an active social life (93% vs. 74%)
- Made them feel stressed, anxious, or depressed (93% vs. 75%) (Figure 2)
Just 27% of those who flare "almost all the time" agreed that they "lead a full life despite having spondylitis", compared 49% for those with flares "on and off". Many also indicated that obstacles to managing AS included pain or feeling unwell, as well as relentless fatigue (82% and 76% respectively). For example, one respondent wrote, "Lots of pain, fatigue. It has had an impact on my family."
Additionally, differences also exist with respect to doctor satisfaction and treatment. Fewer were satisfied with the doctor who primarily treats their HS (31% "extremely" or "very" satisfied compared with 42% for those who flare "on and off"). Those who flare "almost all the time" were also less likely to say that doctor "addresses symptoms of spondylitis such as pain or fatigue" (45% compared with 33% for those who flare "on and off").
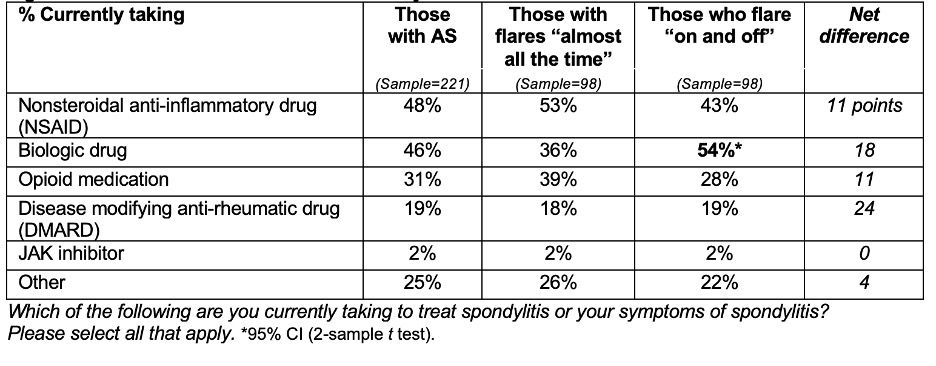
Interestingly, those who flares were near-constant were significantly less likely to have been prescribed biologics (36% vs. 54% flares "on and off"). Additionally, those with almost constant flares were more likely to be treated with NSAIDs (53% vs. 43% flares "on and off" or opioids (39% vs. 28% flares "on and off") (Figure 3).
Conclusion: The extensive impact that flares have on AS patients' quality of life suggests that managing symptoms remains an ongoing concern. The obvious physical, emotional, and interpersonal toll that AS has on the lives of patients, combined with ongoing usage of opioids, indicate the need for better disease management and improved health outcomes. Frequent or near-constant flares, combined with the perception that fatigue, pain and feeling unwell act as obstacles to managing AS, is a reminder that better disease control is needed for many patients with AS.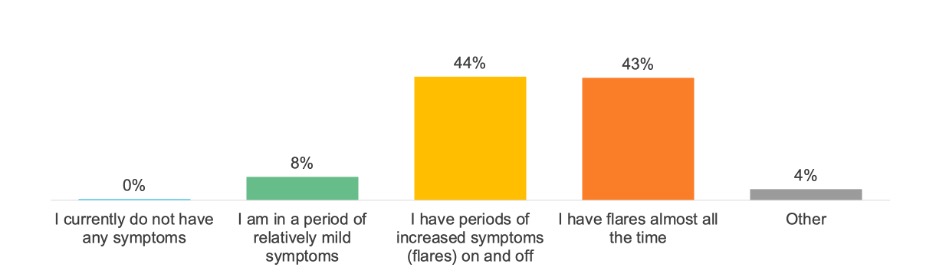
.jpg)
H. Lapidus Glassner: None; E. Luce: None.



