Abstract Session
Diversity, inclusion and racial disparities
Session: Abstracts: Healthcare Disparities in Rheumatology (2455–2460)
2458: The Impact of Social Inequities on Presentation of Childhood-Onset Systemic Lupus Erythematosus (cSLE) at a Large Tertiary Center
Tuesday, November 14, 2023
2:45 PM - 2:55 PM PT
Location: Room 5A-B
- EB
Emily Beil, MD
Baylor College of Medicine
Houston, TX, United StatesDisclosure(s): No financial relationships with ineligible companies to disclose
Presenting Author(s)
Emily Beil1, Eyal Muscal2, Abiodun Oluyomi3, Omar Rosales3, Danielle Guffey4, Marietta DeGuzman1, Cagri Yildirim-Toruner5, Andrea Ramirez3 and Erin Peckham-Gregory3, 1Baylor College of Medicine / Texas Children's Hospital, Houston, TX, 2Division of Rheumatology, Department of Pediatrics, Baylor College of Medicine, Houston, TX, 3Baylor College of Medicine, Houston, TX, 4Institute for Clinical and Translational Research, Baylor College of Medicine, Houston, TX, 5Baylor College of Medicine, Texas Children's Hospital, Houston, TX
Background/Purpose: The prevalence of childhood-onset SLE (cSLE) differs by racial/ethnic group. Yet, the role of social determinants of health (SDoH) in disease severity is not understood. We hypothesized that in an urban center with a large, diverse catchment area, SDoH influence the severity of cSLE at diagnosis.
Methods: We completed an IRB-approved retrospective review of 136 children newly diagnosed with cSLE between 1/1/18-5/31/22 at Texas Children’s Hospital (TCH). We abstracted demographic, clinical severity characteristics (SLEDAI at diagnosis, inpatient or ICU admission, CNS, CYC therapy) and SDoH variables such as State Area Deprivation Index (ADI; higher quartiles indicate greater deprivation), insurance status, distance to care, pollution burden, food accessibility, and social work consultation. Statistical analyses performed in Stata v15.1 and ArcGIS Pro2.2.
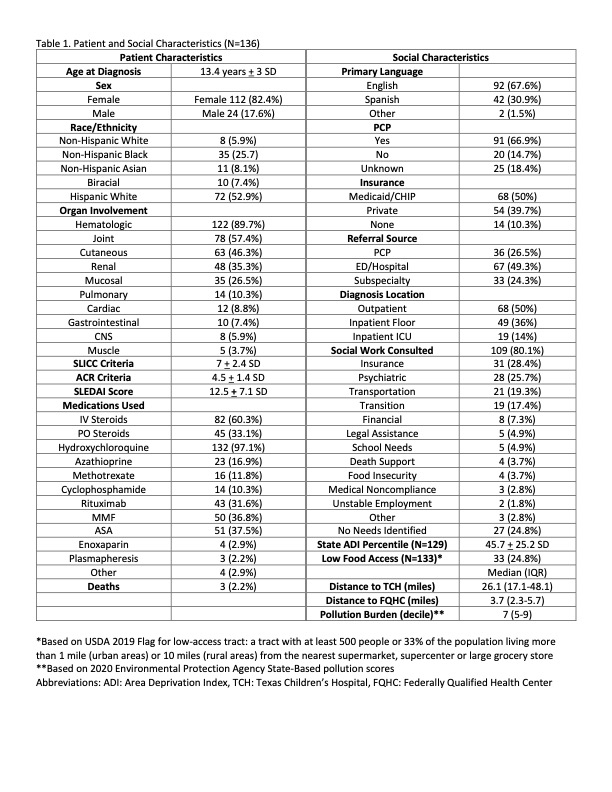
Results: Mean age at diagnosis was 13.4 years + 3 SD, with 82.4% female, 52.9% Hispanic White (HW) and 25.7% non-Hispanic Black (NHB). Fourteen patients (10.3%) were uninsured (UI) and 50% had Medicaid (M) or Children’s Health Insurance Program (CHIP). Half were diagnosed during inpatient admission (14% in the ICU). Average SLEDAI at diagnosis was 12.5 + 7.1 SD; 48.5% had SLEDAI >12 (severe disease). Average ADI (%) was 45.7 + 25.2 SD. Twenty-five percent lived in a census tract with low-access to supermarkets. The median pollution burden score decile was 7 (IQR 5-9). Social work was consulted in 80.1% (Table 1).
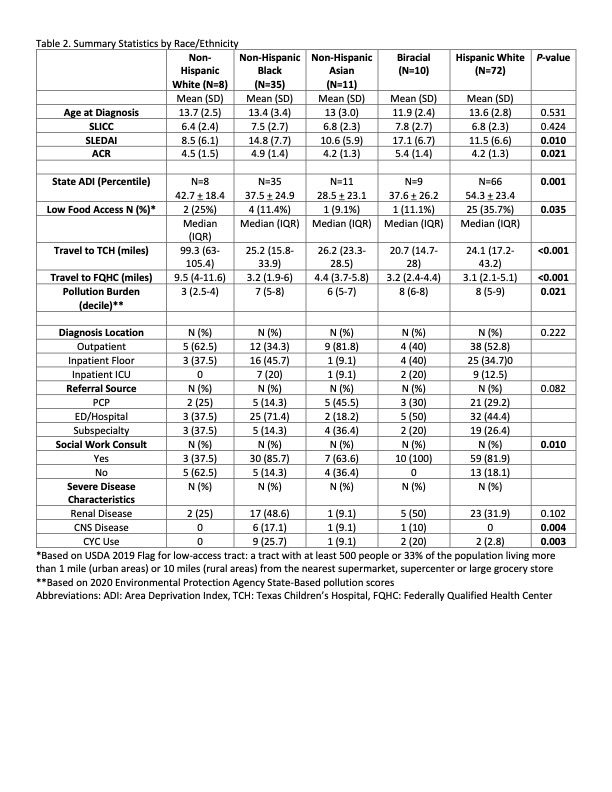
SLEDAI scores were higher in NHB and Biracial (BR) patients at presentation (BR 17.1, NHB 14.8, HW 11.5, Asian (A) 10.6, Non-Hispanic White (NHW) 8.5; P=0.01), Table 2. CNS involvement was highest among NHB children (NHB 17.1%, BR 10%, A 9.1%, HW 0%, NHW 0%; P=0.004). CYC was most often used in NHB and BR patients (NHB 25.7%, BR 20%, A 9.1%, HW 2.8%, NHW 0%; P=0.003). HW patients had the highest ADI (HW 54.3, NHW 42.7, BR 37.6, NHB 37.5, A 28.5; P=0.001) and live in lower food accessible neighborhoods (HW 35.7%, NHW 25%, NHB 11.4%, BR 11.1%, A 9.1%; P=0.035). NHWs travel further to TCH (NHW 99.3 miles, A 26.2, NHB 25.2, HW 24.1, BR 20.7; P< 0.001), live in less polluted neighborhoods (burden score BR 8, HW 8, NHB 7, A 6, NHW 3; P=0.021), and were less likely to have a social work consult (BR 100%, NHB 85.7%, HW 81.9%, A 63.6%, NHW 37.5%; P=0.01).
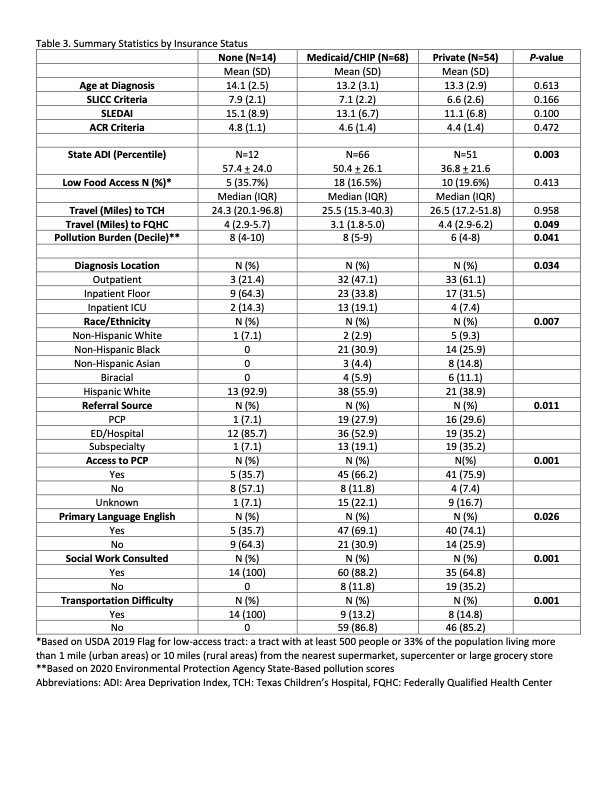
UI patients were most likely to be diagnosed on an inpatient floor and those with M had the highest proportion of ICU admissions (Floor: UI 64.3%, M 33.8%, Private (P) 31.5%; ICU: M 19.1%, UI 14.3%, P 7.4%; P=0.034), Table 3. UI and M patients had higher ADI (UI 57.4%, M 50.4%, P 36.8%; P=0.003), more social work consults (UI 100%, M 88.2%, P 64.8%; P=0.001) and live in more polluted neighborhoods (burden score UI 8, M 8, P 6; P=0.041).
Conclusion: In children with cSLE drawn from a large urban catchment area, we observed an impact of non-modifiable (e.g., race/ethnicity) and modifiable (e.g, insurance status, access to care, food accessibility) factors on disease severity at presentation. Next steps include geospatial mapping to identify high-risk neighborhoods with a discordant number of cSLE patients, and targeting modifiable risk factors in these communities to improve patient experiences and outcomes.
E. Beil: None; E. Muscal: Sobi, 1, 11; A. Oluyomi: None; O. Rosales: None; D. Guffey: None; M. DeGuzman: None; C. Yildirim-Toruner: None; A. Ramirez: None; E. Peckham-Gregory: None.
Background/Purpose: The prevalence of childhood-onset SLE (cSLE) differs by racial/ethnic group. Yet, the role of social determinants of health (SDoH) in disease severity is not understood. We hypothesized that in an urban center with a large, diverse catchment area, SDoH influence the severity of cSLE at diagnosis.
Methods: We completed an IRB-approved retrospective review of 136 children newly diagnosed with cSLE between 1/1/18-5/31/22 at Texas Children’s Hospital (TCH). We abstracted demographic, clinical severity characteristics (SLEDAI at diagnosis, inpatient or ICU admission, CNS, CYC therapy) and SDoH variables such as State Area Deprivation Index (ADI; higher quartiles indicate greater deprivation), insurance status, distance to care, pollution burden, food accessibility, and social work consultation. Statistical analyses performed in Stata v15.1 and ArcGIS Pro2.2.
Results: Mean age at diagnosis was 13.4 years + 3 SD, with 82.4% female, 52.9% Hispanic White (HW) and 25.7% non-Hispanic Black (NHB). Fourteen patients (10.3%) were uninsured (UI) and 50% had Medicaid (M) or Children’s Health Insurance Program (CHIP). Half were diagnosed during inpatient admission (14% in the ICU). Average SLEDAI at diagnosis was 12.5 + 7.1 SD; 48.5% had SLEDAI >12 (severe disease). Average ADI (%) was 45.7 + 25.2 SD. Twenty-five percent lived in a census tract with low-access to supermarkets. The median pollution burden score decile was 7 (IQR 5-9). Social work was consulted in 80.1% (Table 1).
SLEDAI scores were higher in NHB and Biracial (BR) patients at presentation (BR 17.1, NHB 14.8, HW 11.5, Asian (A) 10.6, Non-Hispanic White (NHW) 8.5; P=0.01), Table 2. CNS involvement was highest among NHB children (NHB 17.1%, BR 10%, A 9.1%, HW 0%, NHW 0%; P=0.004). CYC was most often used in NHB and BR patients (NHB 25.7%, BR 20%, A 9.1%, HW 2.8%, NHW 0%; P=0.003). HW patients had the highest ADI (HW 54.3, NHW 42.7, BR 37.6, NHB 37.5, A 28.5; P=0.001) and live in lower food accessible neighborhoods (HW 35.7%, NHW 25%, NHB 11.4%, BR 11.1%, A 9.1%; P=0.035). NHWs travel further to TCH (NHW 99.3 miles, A 26.2, NHB 25.2, HW 24.1, BR 20.7; P< 0.001), live in less polluted neighborhoods (burden score BR 8, HW 8, NHB 7, A 6, NHW 3; P=0.021), and were less likely to have a social work consult (BR 100%, NHB 85.7%, HW 81.9%, A 63.6%, NHW 37.5%; P=0.01).
UI patients were most likely to be diagnosed on an inpatient floor and those with M had the highest proportion of ICU admissions (Floor: UI 64.3%, M 33.8%, Private (P) 31.5%; ICU: M 19.1%, UI 14.3%, P 7.4%; P=0.034), Table 3. UI and M patients had higher ADI (UI 57.4%, M 50.4%, P 36.8%; P=0.003), more social work consults (UI 100%, M 88.2%, P 64.8%; P=0.001) and live in more polluted neighborhoods (burden score UI 8, M 8, P 6; P=0.041).
Conclusion: In children with cSLE drawn from a large urban catchment area, we observed an impact of non-modifiable (e.g., race/ethnicity) and modifiable (e.g, insurance status, access to care, food accessibility) factors on disease severity at presentation. Next steps include geospatial mapping to identify high-risk neighborhoods with a discordant number of cSLE patients, and targeting modifiable risk factors in these communities to improve patient experiences and outcomes.

Table 1. Patient and Social Characteristics (N=136)

Table 2. Summary Statistics by Race/Ethnicity

Table 3. Summary Statistics by Insurance Status
E. Beil: None; E. Muscal: Sobi, 1, 11; A. Oluyomi: None; O. Rosales: None; D. Guffey: None; M. DeGuzman: None; C. Yildirim-Toruner: None; A. Ramirez: None; E. Peckham-Gregory: None.



