Poster Session A
Spondyloarthritis (SpA) including psoriatic arthritis (PsA)
Session: (0510–0542) Spondyloarthritis Including Psoriatic Arthritis – Treatment Poster I: AxSpA
0512: Factors Associated with Treatment Pathways in Early Axial Spondyloarthritis: A Multistate Analysis of the 10-year Follow-up of the DESIR Cohort
Sunday, November 12, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- EP
Abstract Poster Presenter(s)
Elodie Portier1, Sylvie chevret2, Adeline Ruyssen-Witrand3, Anouk Walter-Petrich2, Maxime Dougados4 and Anna Molto5, 1Hôpital Cochin, Paris, France, 2Saint Louis Hospital, Paris, France, 3Toulouse University Hospital, Toulouse, France, 4Rheumatology Department, Cochin Hospital; INSERM (U1153): Clinical Epidemiology and Biostatistics, University of Paris, Paris, France, 5HOPITAL COCHIN AP-HP, Service de Rhumatologie, Paris, France
Background/Purpose: Current recommendations for the management of patients with axial spondyloarthritis (axSpA) emphasize the need of individualized strategy in the therapeutic decision. Thus, many factors seem to impact this strategy.
The objectives of the study were to describe the therapeutic strategies observed in axSpA, and to assess the factors associated with treatment changes over time.
Methods: This study included patients with axSpA from the French prospective cohort DESIR, with a scheduled 10-year follow-up. A multi-state model with 4 ordered treatment states ("none", "non-steroidal anti-inflammatory drugs (NSAID)", "conventional synthetic DMARD (csDMARD)", "TNF inhibitors (TNFi)") was defined, with 6 possible transitions. Estimation of the restricted mean sojourn times spent in each state from the state occupation probabilities was performed. Then, predictors of those transitions were assessed by multivariable Cox models.
Results: 686 (96.9%) of the 708 patients who had more than one visit were analyzed. At cohort entry, 199 (29.0%) were untreated, 427 (62.2%) received NSAID, and 60 (8.7%) received csDMARD and none TNFi.
Over the 10 years of follow-up, patients mostly received NSAID (46.4% of the time) followed by TNFi (24.4% of the time). In multivariable analysis (figure), presence of sacroiliitis on radiography, internal bowel disease and articular index were associated with transition to NSAID. Duration in the previous state was often a significant protective factor associated with transition to csDMARD or TNFi. Finally, the several disease activity outcomes were associated with most transitions.
Conclusion: This was the first study using a multistate model to easily represent the different states, detailing the transitions across them, and their associated factors. Different time profiles of axSpA patient management were identified, including abstention up to a significant proportion of patients treated with csDMARD.
E. Portier: None; S. chevret: None; A. Ruyssen-Witrand: None; A. Walter-Petrich: None; M. Dougados: AbbVie, 2, 5, Bristol Myers Squibb, 2, 5, Eli Lilly, 2, 5, MSD, 2, 5, Novartis, 2, 5, Pfizer Inc, 2, 5, Roche, 2, 5, UCB, 2, 5; A. Molto: None.
Background/Purpose: Current recommendations for the management of patients with axial spondyloarthritis (axSpA) emphasize the need of individualized strategy in the therapeutic decision. Thus, many factors seem to impact this strategy.
The objectives of the study were to describe the therapeutic strategies observed in axSpA, and to assess the factors associated with treatment changes over time.
Methods: This study included patients with axSpA from the French prospective cohort DESIR, with a scheduled 10-year follow-up. A multi-state model with 4 ordered treatment states ("none", "non-steroidal anti-inflammatory drugs (NSAID)", "conventional synthetic DMARD (csDMARD)", "TNF inhibitors (TNFi)") was defined, with 6 possible transitions. Estimation of the restricted mean sojourn times spent in each state from the state occupation probabilities was performed. Then, predictors of those transitions were assessed by multivariable Cox models.
Results: 686 (96.9%) of the 708 patients who had more than one visit were analyzed. At cohort entry, 199 (29.0%) were untreated, 427 (62.2%) received NSAID, and 60 (8.7%) received csDMARD and none TNFi.
Over the 10 years of follow-up, patients mostly received NSAID (46.4% of the time) followed by TNFi (24.4% of the time). In multivariable analysis (figure), presence of sacroiliitis on radiography, internal bowel disease and articular index were associated with transition to NSAID. Duration in the previous state was often a significant protective factor associated with transition to csDMARD or TNFi. Finally, the several disease activity outcomes were associated with most transitions.
Conclusion: This was the first study using a multistate model to easily represent the different states, detailing the transitions across them, and their associated factors. Different time profiles of axSpA patient management were identified, including abstention up to a significant proportion of patients treated with csDMARD.

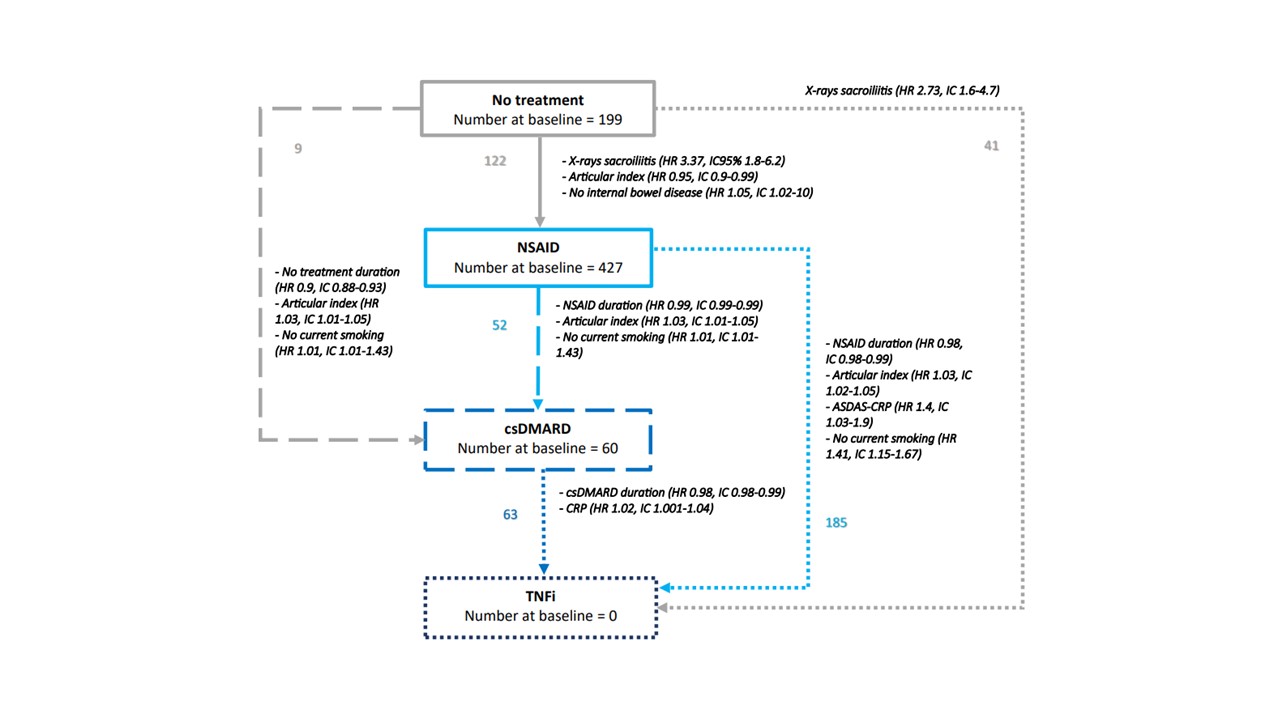
Figure: Multistate model representation. Each arrow corresponds to a possible transition (n=6). Number at baseline denotes the number of patients who started from the state at baseline. The number of events and factors significantly associated with each transition in the multivariable analysis are written near to the corresponding arrow.
NSAID refers to non-steroids anti-inflammatory drugs, csDMARD stands for conventional synthetic Disease Modifying Anti-Rheumatic Drug, and TNFi for tumor necrosis factor inhibitors.
NSAID refers to non-steroids anti-inflammatory drugs, csDMARD stands for conventional synthetic Disease Modifying Anti-Rheumatic Drug, and TNFi for tumor necrosis factor inhibitors.
E. Portier: None; S. chevret: None; A. Ruyssen-Witrand: None; A. Walter-Petrich: None; M. Dougados: AbbVie, 2, 5, Bristol Myers Squibb, 2, 5, Eli Lilly, 2, 5, MSD, 2, 5, Novartis, 2, 5, Pfizer Inc, 2, 5, Roche, 2, 5, UCB, 2, 5; A. Molto: None.



