Abstract Session
Epidemiology, health policy and outcomes
Session: Abstracts: Epidemiology & Public Health II (2449–2454)
2449: Cognitive Functioning Among Individuals with Systemic Lupus Erythematosus: A Population-Based Study
Tuesday, November 14, 2023
2:00 PM - 2:10 PM PT
Location: Room 6E/6D
- LP
Laura Plantinga, PhD, MSc (she/her/hers)
University of California, San Francisco
San Francisco, CA, United StatesDisclosure information not submitted.
Presenting Author(s)
Laura Plantinga1, C. Barrett Bowling2, Charmayne Dunlop-Thomas1, Courtney Hoge1, Bradley Pearce1, Cristina Drenkard1 and S. Sam Lim1, 1Emory University, Atlanta, GA, 2Duke University, Durham, NC
Background/Purpose: Studies of objectively measured cognitive dysfunction in SLE are often limited by small sample size, limited generalizability, and lack of diversity. We sought to comprehensively describe cognitive functioning and its correlates among participants recruited from a population-based, primarily Black U.S. cohort.
Methods: Participants (n=200; mean age, 42.6; 87.5% female, 86.5% Black, 5.0% Hispanic) completed in-person study visits (10/2019-5/2022), which included: (1) the NIH Toolbox Fluid Cognition Battery (episodic memory, working memory, attention and inhibitory control, cognitive flexibility, processing speed, overall composite measure; expressed as T-scores, adjusted for age, gender, race/ethnicity, and education); and (2) two brief screening tests, (a) a clock-drawing task (score range, 0-15; higher score=better performance) and (b) the Trail Making Test (TMT) B task (time in seconds, faster time=better performance). An additional 236 participants completed virtual study visits (10/2020-11/2021), which included NIH Toolbox episodic and working memory modules only. Descriptive statistics were calculated for all measures and the adjusted associations of various participant characteristics with the overall fluid cognition score were assessed with multivariable linear regression. Scatterplots and pairwise correlations were used to estimate relationships between cognitive functioning measures.
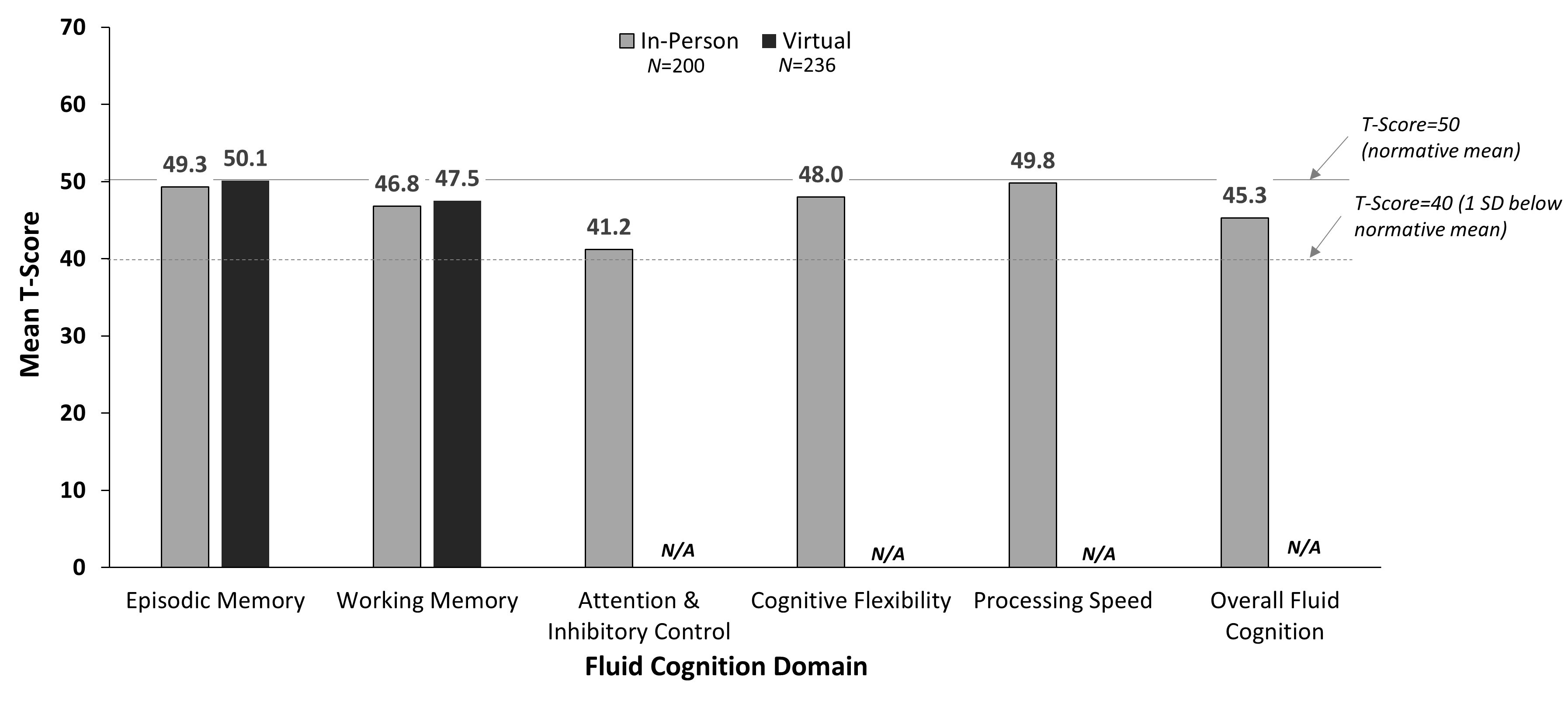
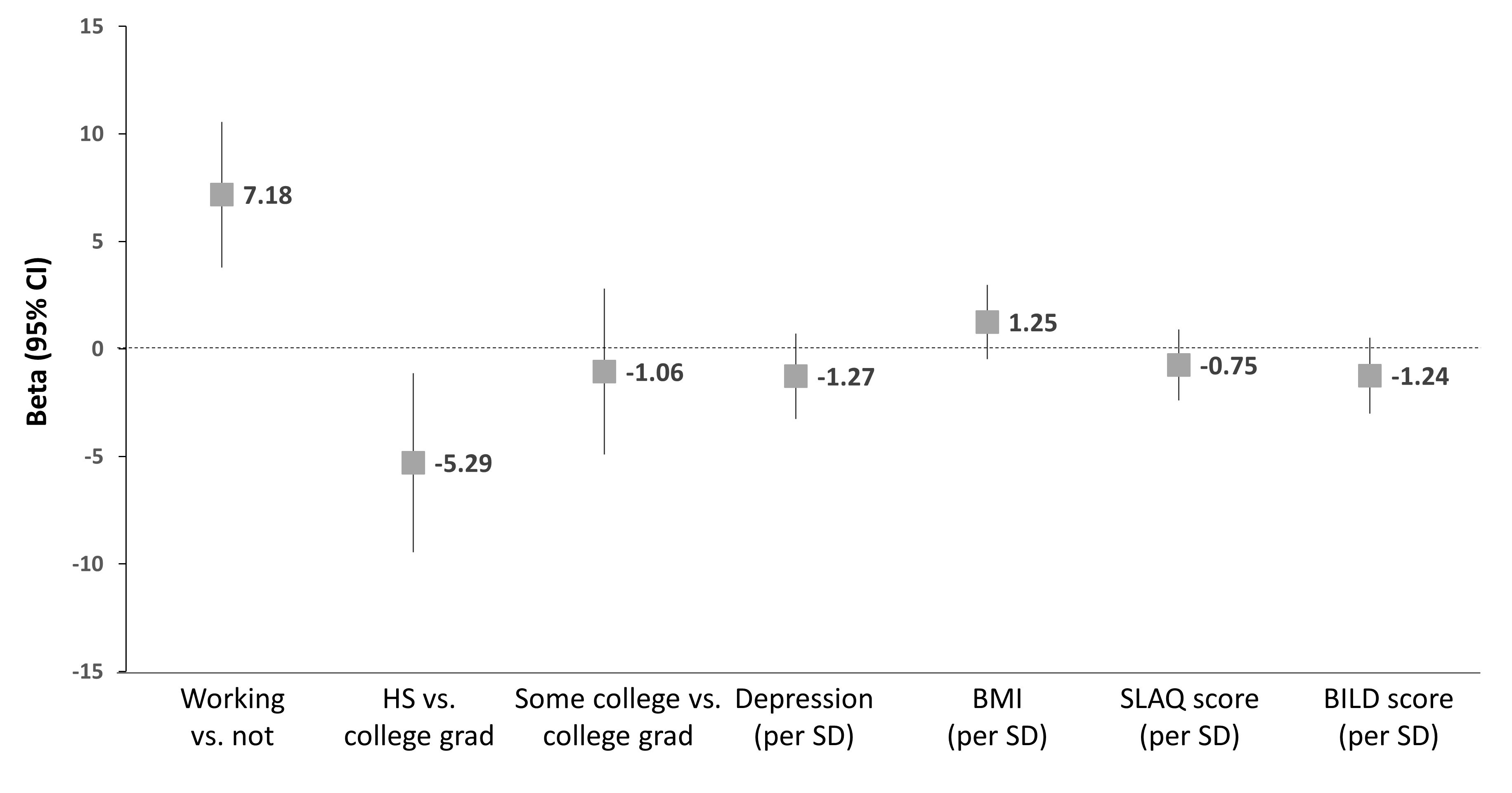
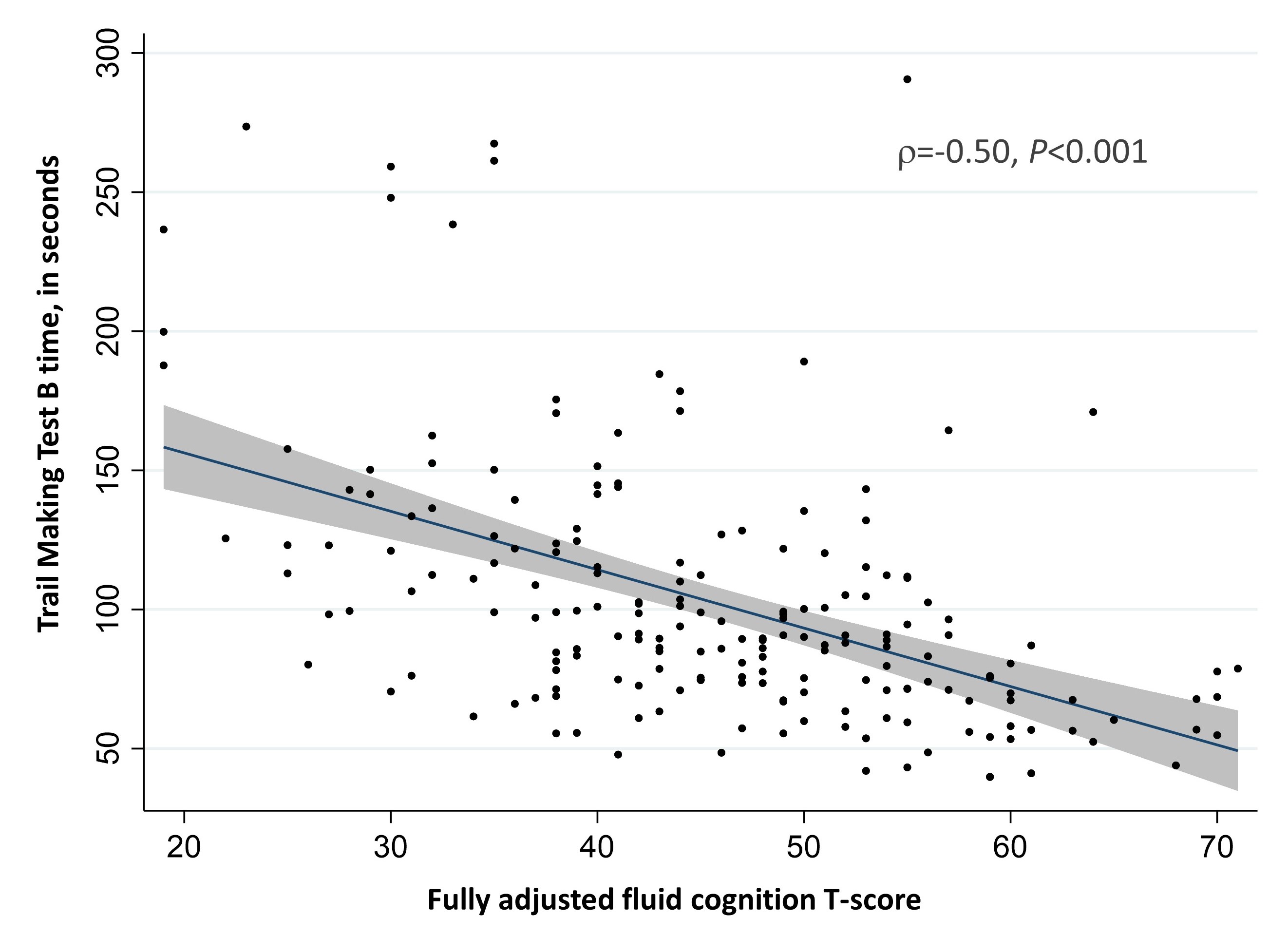
Results: The mean adjusted overall fluid cognition T-score was 45.3, ~0.5 SD below the general population mean; 31% participants scored < 40 ( >1 SD below the mean), suggesting impairment. The mean score for attention and inhibitory control was nearly 1 SD below average (Figure 1). Adjusted fluid cognition T-scores were not associated with age, race, ethnicity, or gender, but those who had a high school education or less vs. having a college degree or higher had 5.3 points ( >0.5 SD) lower score. Current working status was associated with a 7.2-point higher adjusted T-score, while higher depression, SLE activity, and SLE damage scores were associated with slightly lower T-scores (not statistically significant; Figure 2). Clock score (median=14, interquartile range, 13-15) was weakly correlated with fluid cognition T-score (r=0.17, P=0.01), while TMT B time (median=90.3, interquartile range, 71.9-121.1 s) was moderately correlated with fluid cognition T-score (Figure 3). Moreover, 2.5% of individuals did not complete the TMT B within 300 s, suggesting impairment.
Conclusion: Our results suggest individuals with SLE commonly suffer from deficits in fluid cognition, particularly attention and inhibitory control. Higher educational attainment and working status may be protective against impairment, but reverse causality may contribute to this observed pattern. Additionally, we found that multi-domain measurement of global fluid cognition among these individuals may provide nuanced information beyond that available from screening tasks that are designed primarily to detect impairment among older adults. Together, these results inform potential interventions to support cognitive function among individuals with SLE.
L. Plantinga: None; C. Bowling: None; C. Dunlop-Thomas: None; C. Hoge: None; B. Pearce: None; C. Drenkard: None; S. Lim: None.
Background/Purpose: Studies of objectively measured cognitive dysfunction in SLE are often limited by small sample size, limited generalizability, and lack of diversity. We sought to comprehensively describe cognitive functioning and its correlates among participants recruited from a population-based, primarily Black U.S. cohort.
Methods: Participants (n=200; mean age, 42.6; 87.5% female, 86.5% Black, 5.0% Hispanic) completed in-person study visits (10/2019-5/2022), which included: (1) the NIH Toolbox Fluid Cognition Battery (episodic memory, working memory, attention and inhibitory control, cognitive flexibility, processing speed, overall composite measure; expressed as T-scores, adjusted for age, gender, race/ethnicity, and education); and (2) two brief screening tests, (a) a clock-drawing task (score range, 0-15; higher score=better performance) and (b) the Trail Making Test (TMT) B task (time in seconds, faster time=better performance). An additional 236 participants completed virtual study visits (10/2020-11/2021), which included NIH Toolbox episodic and working memory modules only. Descriptive statistics were calculated for all measures and the adjusted associations of various participant characteristics with the overall fluid cognition score were assessed with multivariable linear regression. Scatterplots and pairwise correlations were used to estimate relationships between cognitive functioning measures.
Results: The mean adjusted overall fluid cognition T-score was 45.3, ~0.5 SD below the general population mean; 31% participants scored < 40 ( >1 SD below the mean), suggesting impairment. The mean score for attention and inhibitory control was nearly 1 SD below average (Figure 1). Adjusted fluid cognition T-scores were not associated with age, race, ethnicity, or gender, but those who had a high school education or less vs. having a college degree or higher had 5.3 points ( >0.5 SD) lower score. Current working status was associated with a 7.2-point higher adjusted T-score, while higher depression, SLE activity, and SLE damage scores were associated with slightly lower T-scores (not statistically significant; Figure 2). Clock score (median=14, interquartile range, 13-15) was weakly correlated with fluid cognition T-score (r=0.17, P=0.01), while TMT B time (median=90.3, interquartile range, 71.9-121.1 s) was moderately correlated with fluid cognition T-score (Figure 3). Moreover, 2.5% of individuals did not complete the TMT B within 300 s, suggesting impairment.
Conclusion: Our results suggest individuals with SLE commonly suffer from deficits in fluid cognition, particularly attention and inhibitory control. Higher educational attainment and working status may be protective against impairment, but reverse causality may contribute to this observed pattern. Additionally, we found that multi-domain measurement of global fluid cognition among these individuals may provide nuanced information beyond that available from screening tasks that are designed primarily to detect impairment among older adults. Together, these results inform potential interventions to support cognitive function among individuals with SLE.

Figure 1. Mean fully adjusted* NIH Toolbox Fluid Cognition Battery T-scores among individuals with SLE, by visit type.

Figure 2. Adjusted differences in fluid cognition T-score by individual characteristics. HS, high school; BMI, body mass index; SLAQ, SLE Activity Questionnaire; BILD, Brief Index of Lupus Damage.

Figure 3. Scatterplot of Trail Making Test B time vs. fully adjusted fluid cognition T-Score. Line, fitted values; shaded area, 95% CI.
L. Plantinga: None; C. Bowling: None; C. Dunlop-Thomas: None; C. Hoge: None; B. Pearce: None; C. Drenkard: None; S. Lim: None.



