Abstract Session
Imaging
Session: Abstracts: Imaging of Rheumatic Diseases (0745–0750)
0750: Multispectral Optoacoustic Tomography of the Entheses Reveals Common Metabolic and Architectural Tissue Patterns in Psoriasis and Psoriatic Arthritis Independent of Inflammation
Sunday, November 12, 2023
3:15 PM - 3:25 PM PT
Location: Room 24A-C
- FF
Filippo Fagni, MD (he/him/his)
University clinic of Erlangen and Friedrich Alexander Universität Erlangen-Nürnberg
Erlangen, GermanyDisclosure information not submitted.
Presenting Author(s)
Filippo Fagni1, Koray Tascilar1, Rita Noversa de Sousa2, Sara Bayat1, Lukas Sollfrank3, Arnd Kleyer4, Michael Sticherling5, Adrian Regensburger6, Ferdinand Knieling6, Georg Schett7, Maximilian Waldner8 and David Simon1, 1Friedrich-Alexander-Universität (FAU) Erlangen-Nürnberg & Universitätsklinikum Erlangen, Department of Internal Medicine 3 - Rheumatology and Immunology / Deutsches Zentrum Immuntherapie, Erlangen, Germany, 2Department of Internal Medicine 3, Friedrich-Alexander University (FAU) Erlangen-Nuremberg and Universitätsklinikum Erlangen, Erlangen, Germany, 3Department Dermatology, Friedrich-Alexander University (FAU) Erlangen-Nuremberg and Universitätsklinikum Erlangen, Erlangen, Germany, 4University Hospital Erlangen, Erlangen, Germany, 5Friedrich-Alexander-Universität (FAU) Erlangen-Nürnberg & Universitätsklinikum Erlangen, Department of Dermatology, Erlangen, Germany, 6Department of Pediatrics and Adolescent Medicine, Friedrich-Alexander University (FAU) Erlangen-Nuremberg and Universitätsklinikum Erlangen, Erlangen, Germany, 7Friedrich-Alexander-Universität Erlangen-Nürnberg, Erlangen, Germany, 8Department of Internal Medicine 1, Friedrich-Alexander University (FAU) Erlangen-Nuremberg and Universitätsklinikum Erlangen, Erlangen, Germany
Background/Purpose: Multispectral optoacoustic tomography (MSOT) is a novel imaging platform that combines ultrasound (US) with optoacoustic imaging to allow non-invasive in vivo quantification of key metabolites of inflammation such as hemoglobin (Hb), oxygen saturation (SO2), and collagen and lipid levels by analyzing the wavelength spectra of the target tissues when exposed to near-infrared laser light (Regensburger AP, Biomedicines (2021)). MSOT has already proven capable of identifying arthritis and enthesitis in patients with PsA and RA (Tascilar K, Rheumatology (2023)). In our study, we aimed to assess metabolic and inflammatory changes at the entheses in patients with psoriasis (PsO), PsA, and healthy controls (HC) using MSOT in order to identify new potential imaging biomarkers for enthesitis.
Methods: A cross-sectional study in bDMARD-naïve PsA and PsO patients and HC was performed. Participants underwent sequential clinical, US and MSOT examination of six entheses (lateral humeral epicondyle, distal patellar tendon attachment, Achilles). MSOT wavelength spectra were determined and the corresponding values of Hb, SO2, collagen, and lipid were quantified. Mean differences between groups were calculated using linear mixed effects models. MSOT-measured analytes were compared between tender and non-tender entheses and between entheses with and without OMERACT-defined US anomalies. The study was approved by the Ethics Committee of the University of Erlangen-Nuremberg (464_18 B; 7) and was registered as a clinical trial (DRKS00024360).
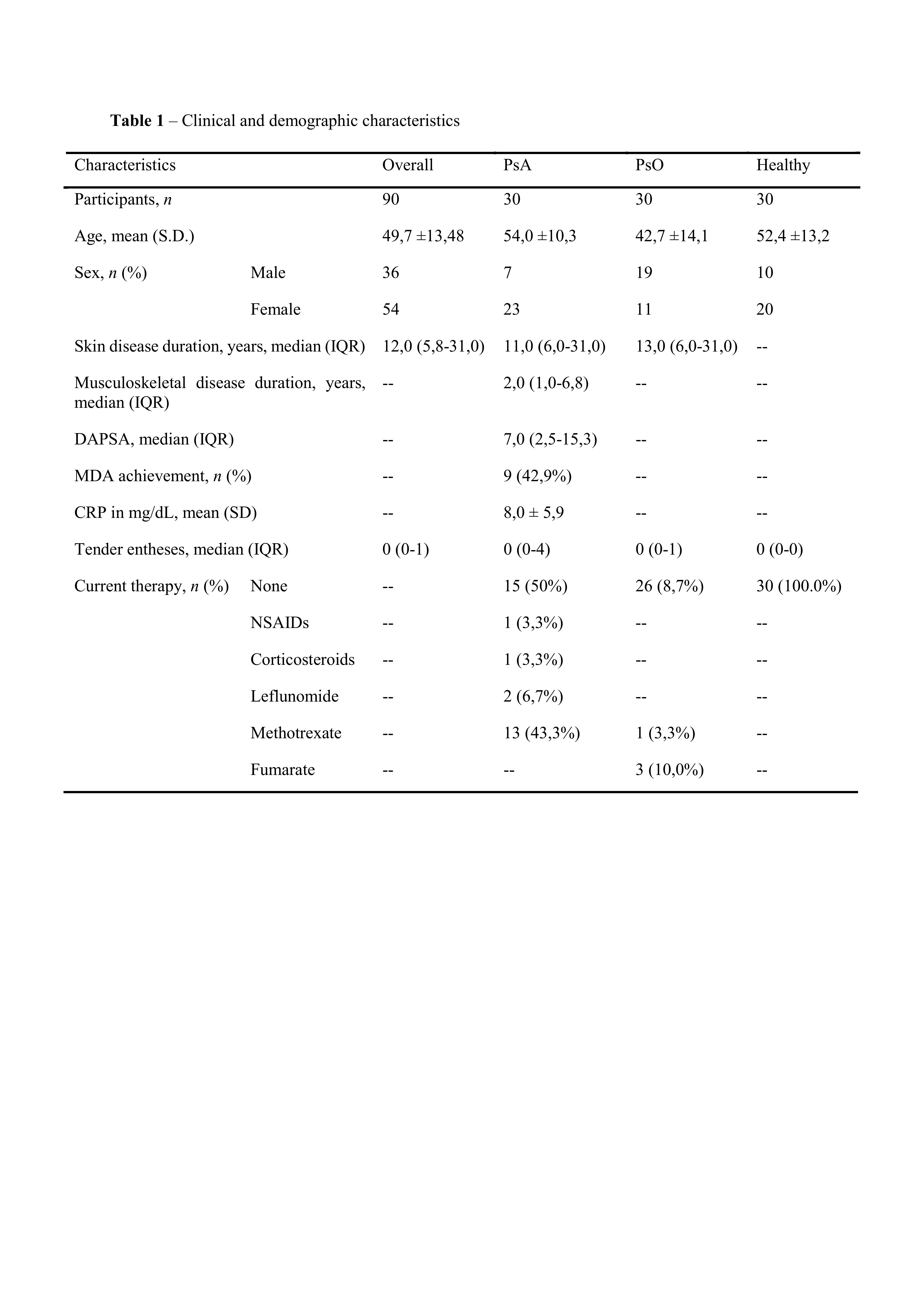
Results: Ninety participants were included (30 PsO, 30 PsA, 30 HC). Clinical and demographic characteristics are shown in table 1.540 entheses were clinically assessed, 540 US and 830 MSOT scans were obtained. Comparing MSOT wavelength spectra, significant differences from HC emerged for PsA between 800 nm and 1064 nm, and for PsO between 930 nm and 1100 nm (Figure 1). The corresponding metabolites distribution was obtained. Both PsA and PsO patients showed significantly increased oxygenated Hb (PsA: p=0.005; PsO: p=0.001) and SO2 (PsA: p< 0.001; PsO, p=0.001) levels and decreased collagen signals (PsA: p< 0.001; PsO: < 0.001) compared to HC, with more pronounced changes in the PsA group (Table 2). Significantly lower collagen levels (p=0.01) and increased signal for lipids (p=0.02) were recorded in tender entheses compared with non-tender ones. The presence of at least one US anomaly was associated with a significant positive difference in SO2 (p=0.003).
Conclusion: PsO and PsA patients show a distinct entheseal metabolic profile that is common to all psoriatic patients independently from clinical and US-detected signs of inflammation, thereby supporting the notion of a psoriatic disease spectrum characterized by varying degrees of musculoskeletal inflammation. Furthermore, MSOT can detect differences between inflamed and uninflamed entheses that are more pronounced in PsA than in those with skin psoriasis alone. Research efforts should now focus on defining MSOT cutoff values for enthesitis and longitudinal analyses should be conducted to assess the utility of MSOT as a risk stratification tool for the risk of progression to PsA in at-risk patients.
F. Fagni: Eli Lilly, 6, Galapagos, 6, Novartis, 6; K. Tascilar: None; R. Noversa de Sousa: None; S. Bayat: EI Lilly, 5; L. Sollfrank: None; A. Kleyer: None; M. Sticherling: EI Lilly, 5, El Lilly, 6, Janssen, 5, 6, Novartis, 5, 6; A. Regensburger: None; F. Knieling: None; G. Schett: None; M. Waldner: None; D. Simon: Janssen, 5.
Background/Purpose: Multispectral optoacoustic tomography (MSOT) is a novel imaging platform that combines ultrasound (US) with optoacoustic imaging to allow non-invasive in vivo quantification of key metabolites of inflammation such as hemoglobin (Hb), oxygen saturation (SO2), and collagen and lipid levels by analyzing the wavelength spectra of the target tissues when exposed to near-infrared laser light (Regensburger AP, Biomedicines (2021)). MSOT has already proven capable of identifying arthritis and enthesitis in patients with PsA and RA (Tascilar K, Rheumatology (2023)). In our study, we aimed to assess metabolic and inflammatory changes at the entheses in patients with psoriasis (PsO), PsA, and healthy controls (HC) using MSOT in order to identify new potential imaging biomarkers for enthesitis.
Methods: A cross-sectional study in bDMARD-naïve PsA and PsO patients and HC was performed. Participants underwent sequential clinical, US and MSOT examination of six entheses (lateral humeral epicondyle, distal patellar tendon attachment, Achilles). MSOT wavelength spectra were determined and the corresponding values of Hb, SO2, collagen, and lipid were quantified. Mean differences between groups were calculated using linear mixed effects models. MSOT-measured analytes were compared between tender and non-tender entheses and between entheses with and without OMERACT-defined US anomalies. The study was approved by the Ethics Committee of the University of Erlangen-Nuremberg (464_18 B; 7) and was registered as a clinical trial (DRKS00024360).
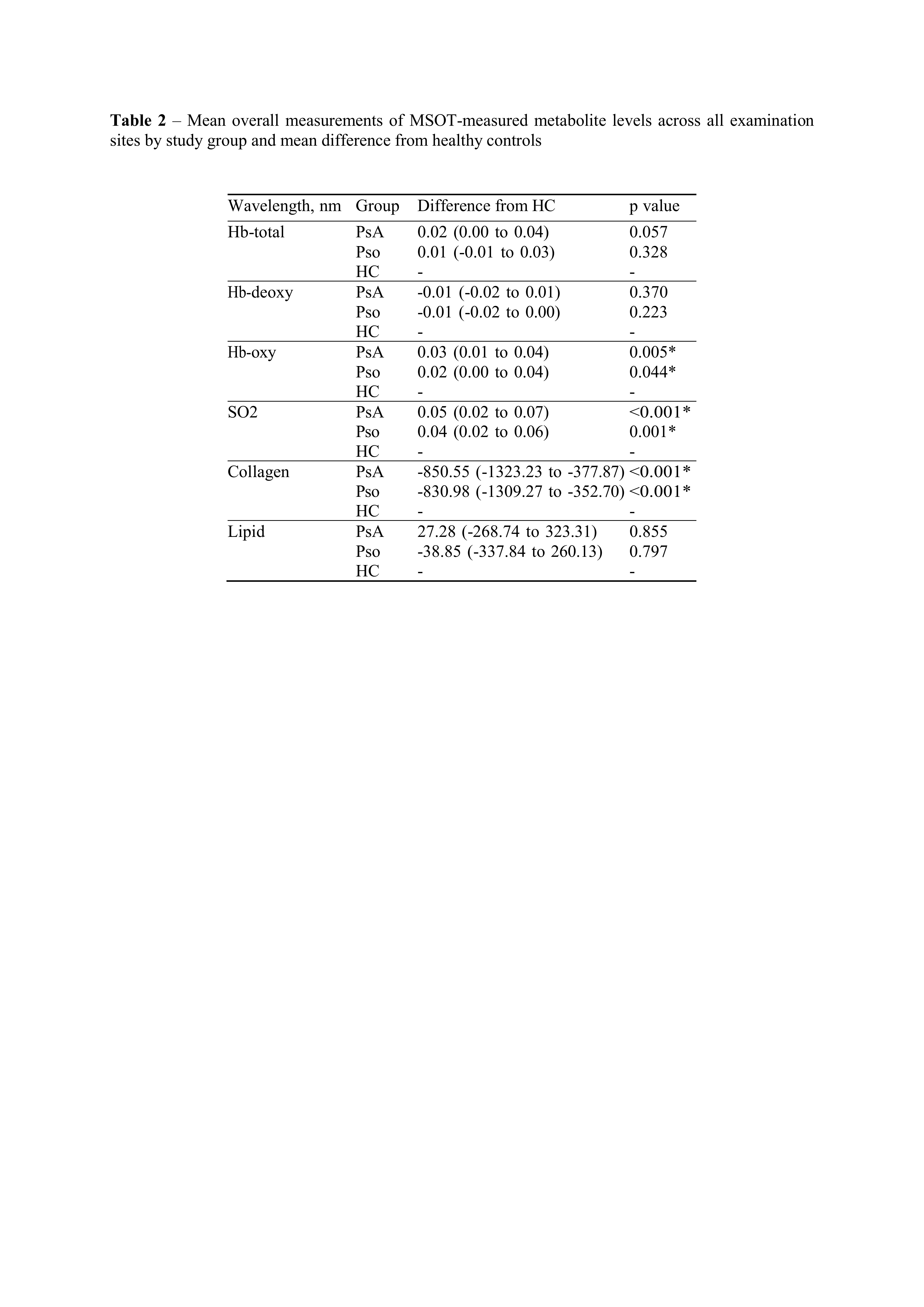
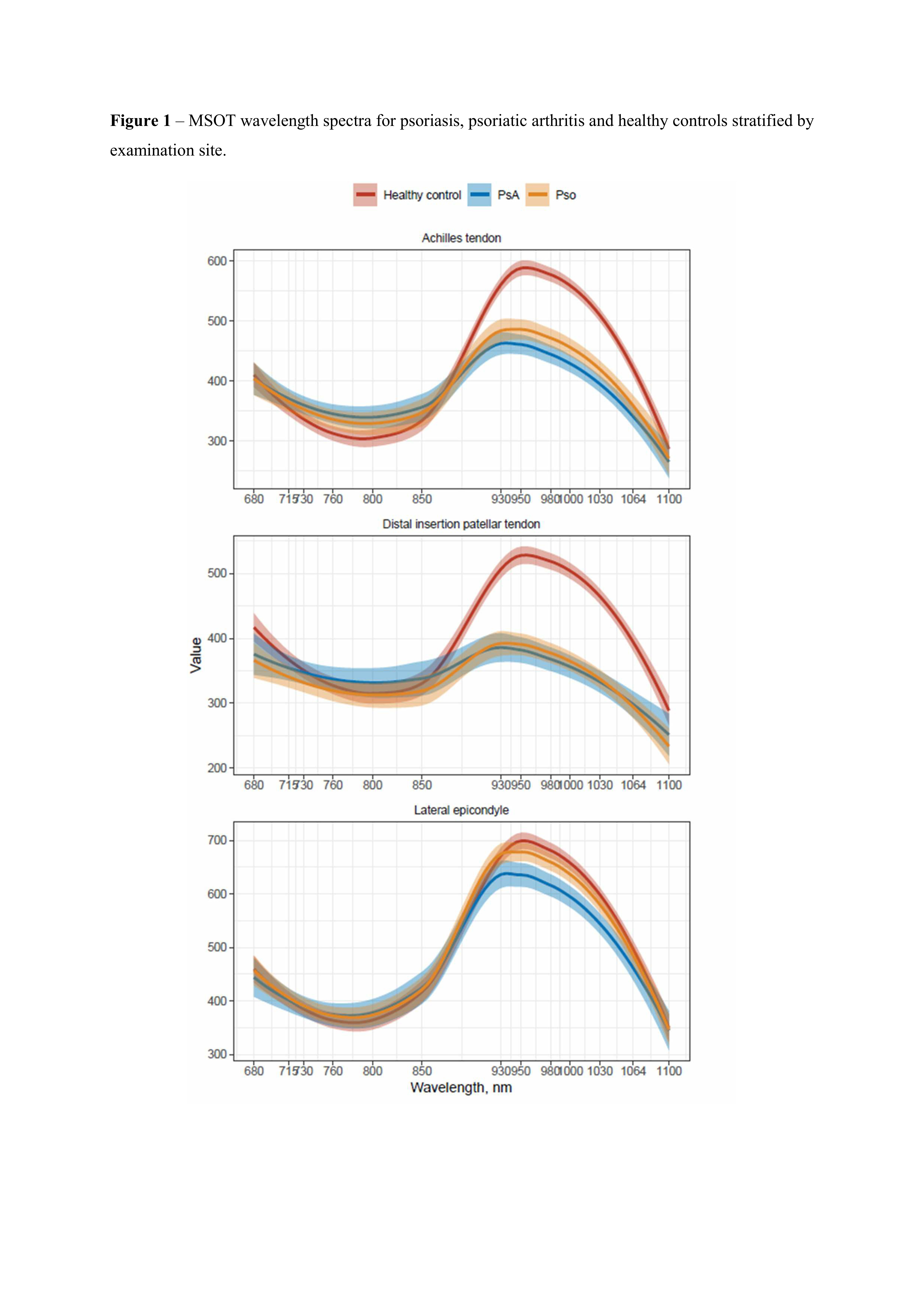
Results: Ninety participants were included (30 PsO, 30 PsA, 30 HC). Clinical and demographic characteristics are shown in table 1.540 entheses were clinically assessed, 540 US and 830 MSOT scans were obtained. Comparing MSOT wavelength spectra, significant differences from HC emerged for PsA between 800 nm and 1064 nm, and for PsO between 930 nm and 1100 nm (Figure 1). The corresponding metabolites distribution was obtained. Both PsA and PsO patients showed significantly increased oxygenated Hb (PsA: p=0.005; PsO: p=0.001) and SO2 (PsA: p< 0.001; PsO, p=0.001) levels and decreased collagen signals (PsA: p< 0.001; PsO: < 0.001) compared to HC, with more pronounced changes in the PsA group (Table 2). Significantly lower collagen levels (p=0.01) and increased signal for lipids (p=0.02) were recorded in tender entheses compared with non-tender ones. The presence of at least one US anomaly was associated with a significant positive difference in SO2 (p=0.003).
Conclusion: PsO and PsA patients show a distinct entheseal metabolic profile that is common to all psoriatic patients independently from clinical and US-detected signs of inflammation, thereby supporting the notion of a psoriatic disease spectrum characterized by varying degrees of musculoskeletal inflammation. Furthermore, MSOT can detect differences between inflamed and uninflamed entheses that are more pronounced in PsA than in those with skin psoriasis alone. Research efforts should now focus on defining MSOT cutoff values for enthesitis and longitudinal analyses should be conducted to assess the utility of MSOT as a risk stratification tool for the risk of progression to PsA in at-risk patients.

Table 1 – Clinical and demographic characteristics

Table 2 – Mean overall measurements of MSOT-measured metabolite levels across all examination sites by study group and mean difference from healthy controls

Figure 1 – MSOT wavelength spectra for psoriasis, psoriatic arthritis and healthy controls stratified by examination site.
F. Fagni: Eli Lilly, 6, Galapagos, 6, Novartis, 6; K. Tascilar: None; R. Noversa de Sousa: None; S. Bayat: EI Lilly, 5; L. Sollfrank: None; A. Kleyer: None; M. Sticherling: EI Lilly, 5, El Lilly, 6, Janssen, 5, 6, Novartis, 5, 6; A. Regensburger: None; F. Knieling: None; G. Schett: None; M. Waldner: None; D. Simon: Janssen, 5.



