Poster Session B
Vasculitis
Session: (1534–1553) Vasculitis – ANCA-Associated Poster II: Epidemiology, Outcomes, & Classification
1546: Eosinophilic Granulomatosis with Polyangiitis: Clinical Suspicion Red Flags Identification by a Systematic Literature Review and Multidisciplinary Expert Consensus
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- RB
Ricardo Blanco, PhD
Hospital Universitario Marqués de Valdecilla, IDIVAL
Santander, SpainDisclosure information not submitted.
Abstract Poster Presenter(s)
Ricardo Blanco1, Iñigo Rúa-Figueroa2, Roser Solans3, Maria C Cid4, Marina Blanco5, Ismael Garcia Moguel6, Francisco Perez Grimaldi7, Ana Noblejas8, Moises Labrador3, Cristian Domingo9, Georgina espigol10, Fernando Sanchez Toril11, Francisco Ortiz-Sanjuán12, Ebymar Arismendi13 and Jose María Alvaro-Gracias14, 1Hospital Universitario Marqués de Valdecilla, IDIVAL, Santander, Spain, 2Rheumatology, Hospital de Gran Canaria Doctor Negrin, Las Palmas de Gran Canaria, Spain, 3Internal Medicine Department, H. Universitari Vall d’Hebron, Universitat Autònoma de Barcelona, Barcelona, Spain, 4Hospital Clinic Barcelona, Barcelona, Spain, 5Pneumology Department, Hospital Universitario de A Coruña, Madrid, Spain, 6Allergy Department, Hospital Universitario 12 de Octubre, Madrid, Spain; Instituto de Investigación Sanitaria Hospital 12 de Octubre (imas12), Madrid, Spain, 7Pneumology Department, H. University of Jerez, Cádiz, Spain, 8Internal Medicine Department, Hospital Universitario La Paz, Madrid, Spain, 9Pneumology Department, Corporació Sanitaria Parc Taulí, Universitat Autònoma de Barcelona, Barcelona, Spain, 10Autoimmune Diseases Department, Hospital Clínic, FCRB-IDIBAPS, Universitat de Barcelona, Barcelona, Spain, 11Pneumology Department, Hospital Arnau Vilanova, Valencia, Spain;, Valencia, Spain, 12Hospital Universitario y Politécnico La Fe, Valencia, Spain, 13Pneumology Department, Hospital Clínic de Barcelona, Barcelona, Spain, Universitat de Barcelona, Spain and CIBERES, Barcelona, Spain, 14Hospital General Universitario Gregorio Marañon, Madrid, Spain
Background/Purpose: Eosinophilic Granulomatosis with Polyangiitis (EGPA) is a rare ANCA-associated vasculitis, characterized histologically by eosinophilic tissue infiltration, necrotizing vasculitis, and eosinophil-rich granulomatous inflammation.
The diagnosis of EGPA is often challenging due to its rarity, heterogeneous and multiorgan clinical presentation, and the overlapping with other vasculitis or eosinophilic disorders. The identification of suspicion signals of EGPA addresses a fundamental practical barrier in achieving timely diagnosis for patients with this rare but potentially devastating disease.
Our purpose was to identify a comprehensive and evidence-based checklist of signs, symptoms and laboratory parameters reported to precede the diagnosis of EGPA that can be used as red flags, raising the suspicion and prompt the performance of appropriate confirmatory tests.
Methods: A systematic literature search strategy was developed to identify signs, symptoms and laboratory abnormalities that should raise the suspicion of a possible EGPA patient. GRADE (Grading of Recommendations, Assessment, Development and Evaluations) methodology was used to assess the quality of the scientific evidence supporting each criterion.
A multidisciplinary nominal group consensus approach (including rheumatologists, internal medicine specialists, pulmonologists, and allergists) was established for the development of the expert consensus.
Red flags identified as suspicion signals for EGPA were categorized by organ system, manifestation, and laboratory test to facilitate rational, evidence-based clinical review of patients presenting with eosinophilia.
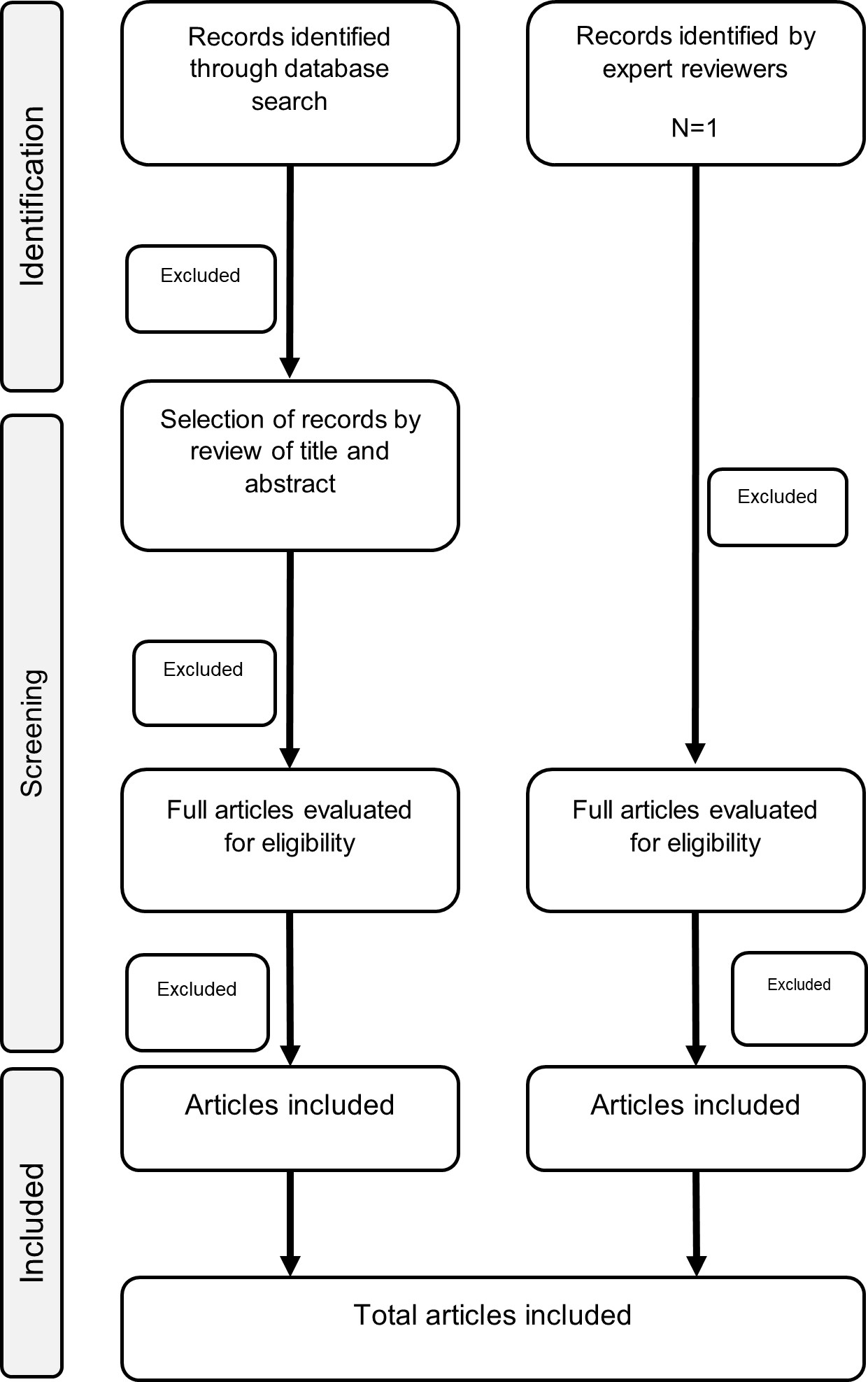
Results: A total of 382 records were identified and reviewed, and 85 studies were included in the literature review (Figure 1). From these 85 publications a total of 214 items were assessed and 40 red flags were identified as relevant to raise a suspicion of EGPA. As the publications were derived from observational studies the GRADE level of evidence was low.
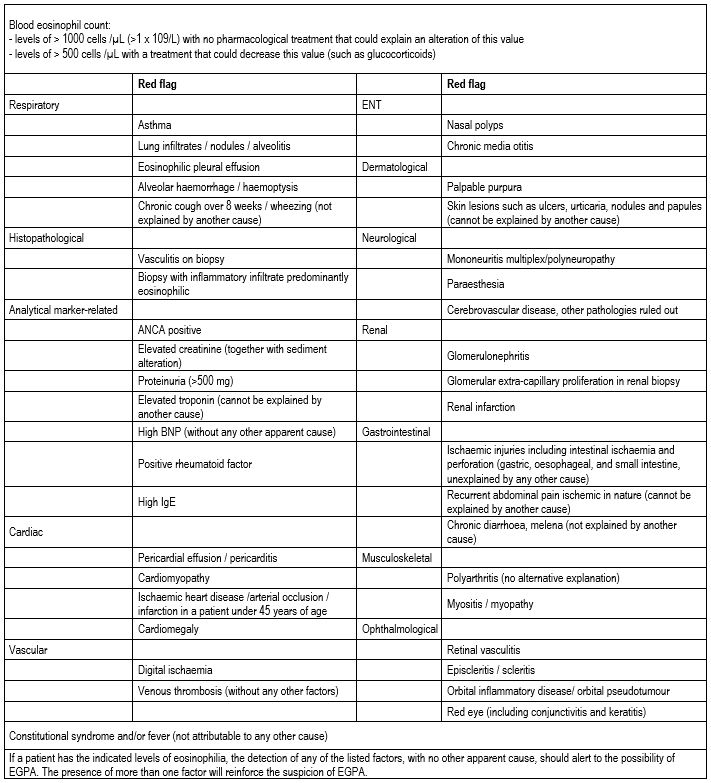
Using these 40 red flags, an evidence-based clinical checklist tool was developed for use in routine practice to raise EGPA suspicion in patients with eosinophilia (peripheral blood eosinophil count >1 x 109/L, with no treatment that could explain an alteration of this value) (Table 1).
Conclusion: Systematic literature review, multidisciplinary expert consensus rating and GRADE methodology has enabled, for the first time, the identification of a comprehensive set of red flags that could be used to raise a suspicion for EGPA, providing clinicians with an evidence-based checklist tool that can be integrated into their routine practice.
R. Blanco: AbbVie, 5, 6, Amgen, 6, AstraZeneca, 2, BMS, 6, Eli Lilly, 6, Galapagos, 2, 6, Janssen, 2, 6, MSD, 6, Novartis, 2, 6, Pfizer, 2, 6, Roche, 5, 6, Sanofi, 6; I. Rúa-Figueroa: AstraZeneca, 5, GSK, 1, 6; R. Solans: CSL-Vifor, 6, GSK, 1, 6; M. Cid: AbbVie/Abbott, 1, 2, 6, AstraZeneca, 1, GSK, 1, 2, 6, Kininksa Pharmaceutical, 5, SCL-Vifor, 2, 6; M. Blanco: None; I. Garcia Moguel: AstraZeneca, 1, 2, 5, 6, GSK, 1, 2, 5, 6, Sanofi, 1, 2, 5, 6, Teva Therapeutics, 1, 2, 5, 6; F. Perez Grimaldi: AstraZeneca, 6, Chiesi, 6, GSK, 6, Novartis, 6, Sanofi, 6, Teva Therapeutics, 6; A. Noblejas: CSL-Vifor, 6, GSK, 1, 6; M. Labrador: AstraZeneca, 6, GSK, 1, 6, Novartis, 6, Sanofi, 6; C. Domingo: ALK, 1, 2, 5, 6, AstraZeneca, 1, 2, 5, 6, Chiesi, 1, 2, 5, 6, GSK, 1, 2, 6, Menarini, 12, Travel fees, Novartis, 1, 2, 5, 6, Sanofi, 1, 2, 5, 6, Teva Therapeutics, 1, 2, 5, 6; G. espigol: CSl-Vifor, 1, GSK, 1; F. Sanchez Toril: None; F. Ortiz-Sanjuán: Eli Lilly, 6, Grunenthal, 2, GSK, 2; E. Arismendi: AstraZeneca, 6, GebroPharna, 6, GSK, 6, Merck/MSD, 6, Sanofi, 1; J. Alvaro-Gracias: Abbvie, 2, 6, AstraZeneca, 2, 6, Eli Lilly, 2, 6, Galapagos, 2, 6, Gilead, 2, 6, GSK, 2, 6, Merck/MSD, 2, 6, Novartis, 2, 6, Pfizer, 2, 6, UCB, 2, 6.
Background/Purpose: Eosinophilic Granulomatosis with Polyangiitis (EGPA) is a rare ANCA-associated vasculitis, characterized histologically by eosinophilic tissue infiltration, necrotizing vasculitis, and eosinophil-rich granulomatous inflammation.
The diagnosis of EGPA is often challenging due to its rarity, heterogeneous and multiorgan clinical presentation, and the overlapping with other vasculitis or eosinophilic disorders. The identification of suspicion signals of EGPA addresses a fundamental practical barrier in achieving timely diagnosis for patients with this rare but potentially devastating disease.
Our purpose was to identify a comprehensive and evidence-based checklist of signs, symptoms and laboratory parameters reported to precede the diagnosis of EGPA that can be used as red flags, raising the suspicion and prompt the performance of appropriate confirmatory tests.
Methods: A systematic literature search strategy was developed to identify signs, symptoms and laboratory abnormalities that should raise the suspicion of a possible EGPA patient. GRADE (Grading of Recommendations, Assessment, Development and Evaluations) methodology was used to assess the quality of the scientific evidence supporting each criterion.
A multidisciplinary nominal group consensus approach (including rheumatologists, internal medicine specialists, pulmonologists, and allergists) was established for the development of the expert consensus.
Red flags identified as suspicion signals for EGPA were categorized by organ system, manifestation, and laboratory test to facilitate rational, evidence-based clinical review of patients presenting with eosinophilia.
Results: A total of 382 records were identified and reviewed, and 85 studies were included in the literature review (Figure 1). From these 85 publications a total of 214 items were assessed and 40 red flags were identified as relevant to raise a suspicion of EGPA. As the publications were derived from observational studies the GRADE level of evidence was low.
Using these 40 red flags, an evidence-based clinical checklist tool was developed for use in routine practice to raise EGPA suspicion in patients with eosinophilia (peripheral blood eosinophil count >1 x 109/L, with no treatment that could explain an alteration of this value) (Table 1).
Conclusion: Systematic literature review, multidisciplinary expert consensus rating and GRADE methodology has enabled, for the first time, the identification of a comprehensive set of red flags that could be used to raise a suspicion for EGPA, providing clinicians with an evidence-based checklist tool that can be integrated into their routine practice.

Figure 1. PRISMA flowchart for the systematic literature review.

TABLE 1. EGPA suspicion red flags
R. Blanco: AbbVie, 5, 6, Amgen, 6, AstraZeneca, 2, BMS, 6, Eli Lilly, 6, Galapagos, 2, 6, Janssen, 2, 6, MSD, 6, Novartis, 2, 6, Pfizer, 2, 6, Roche, 5, 6, Sanofi, 6; I. Rúa-Figueroa: AstraZeneca, 5, GSK, 1, 6; R. Solans: CSL-Vifor, 6, GSK, 1, 6; M. Cid: AbbVie/Abbott, 1, 2, 6, AstraZeneca, 1, GSK, 1, 2, 6, Kininksa Pharmaceutical, 5, SCL-Vifor, 2, 6; M. Blanco: None; I. Garcia Moguel: AstraZeneca, 1, 2, 5, 6, GSK, 1, 2, 5, 6, Sanofi, 1, 2, 5, 6, Teva Therapeutics, 1, 2, 5, 6; F. Perez Grimaldi: AstraZeneca, 6, Chiesi, 6, GSK, 6, Novartis, 6, Sanofi, 6, Teva Therapeutics, 6; A. Noblejas: CSL-Vifor, 6, GSK, 1, 6; M. Labrador: AstraZeneca, 6, GSK, 1, 6, Novartis, 6, Sanofi, 6; C. Domingo: ALK, 1, 2, 5, 6, AstraZeneca, 1, 2, 5, 6, Chiesi, 1, 2, 5, 6, GSK, 1, 2, 6, Menarini, 12, Travel fees, Novartis, 1, 2, 5, 6, Sanofi, 1, 2, 5, 6, Teva Therapeutics, 1, 2, 5, 6; G. espigol: CSl-Vifor, 1, GSK, 1; F. Sanchez Toril: None; F. Ortiz-Sanjuán: Eli Lilly, 6, Grunenthal, 2, GSK, 2; E. Arismendi: AstraZeneca, 6, GebroPharna, 6, GSK, 6, Merck/MSD, 6, Sanofi, 1; J. Alvaro-Gracias: Abbvie, 2, 6, AstraZeneca, 2, 6, Eli Lilly, 2, 6, Galapagos, 2, 6, Gilead, 2, 6, GSK, 2, 6, Merck/MSD, 2, 6, Novartis, 2, 6, Pfizer, 2, 6, UCB, 2, 6.



