Poster Session B
Crystal arthropathies
Session: (1100–1123) Metabolic & Crystal Arthropathies – Basic & Clinical Science Poster II
1120: Target Serum Urate Levels, Recurrent Gout Flare Rates, and Gout-Primary Hospitalizations: Nationwide Prospective Cohort Study of 3,613 Gout Patients
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall

Natalie McCormick, PhD, MSc (she/her/hers)
Massachusetts General Hospital
Boston, MA, United StatesDisclosure(s): No financial relationships with ineligible companies to disclose
Abstract Poster Presenter(s)
Natalie McCormick1, Chio Yokose2, Gregory Challener1, Amit Joshi3, Sruthi Tanikella1 and Hyon K. Choi4, 1Massachusetts General Hospital, Boston, MA, 2Massachusetts General Hospital, Waltham, MA, 3Channing Division of Network Medicine, Boston, MA, 4Massachusetts General Hospital and Harvard Medical School, Lexington, MA
Background/Purpose: Despite rheumatology guidelines' emphasis on treat-to-target-serum-urate (SU) levels (<6 or <5 mg/dL, urate crystal sub-saturation points), this pathophysiology-based recommendation is not accepted in primary care practice (where >90% of gout care occurs) or endorsed by the American College of Physicians.To that end, proportions of gout flares associated with these target levels, including those requiring hospitalization, are unknown. We quantified associations of target SU with recurrent flares, including gout-primary hospitalizations, among gout patients nested in a prospective nationwide cohort.
Methods: This was a prospective cohort study of UK adults recruited over 2006-2010 and followed-up through primary care medical record linkage. As done previously [Cipolletta et al. JAMA 2022], flares among prevalent gout patients were ascertained by (1) hospitalization with gout (ICD-10 M10) as primary discharge diagnosis; (2) diagnosis of gout flare in primary care records; or (3) diagnosis of gout in primary care records and prescription issued on the same day for corticosteroids, colchicine, or non-steroidal anti-inflammatory drugs (NSAIDs).We also investigated flares requiring hospitalisation. Poisson regression was used to assess the relation between baseline SU levels and rates of recurrent gout flares over 1, 2, 5, and 10 years of follow-up.
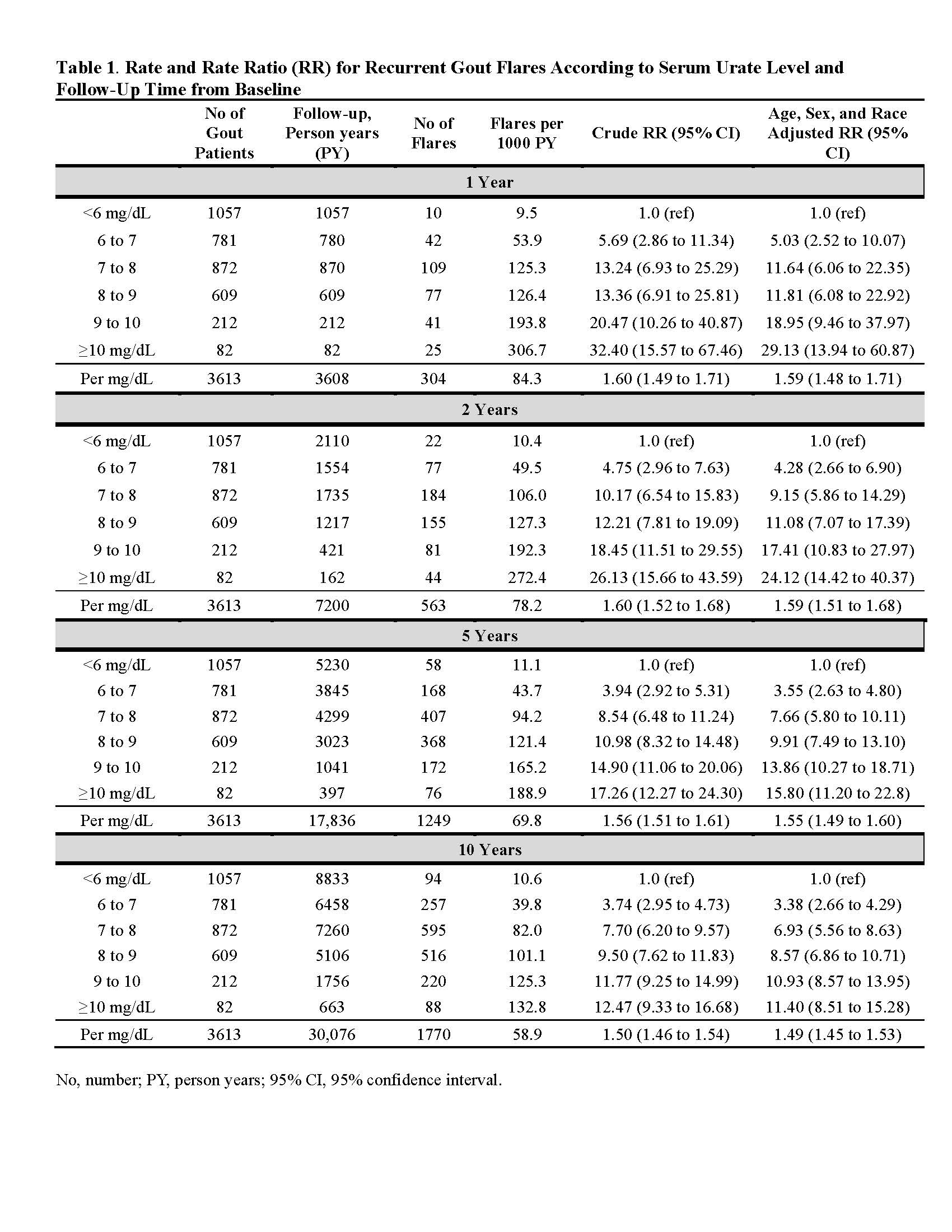
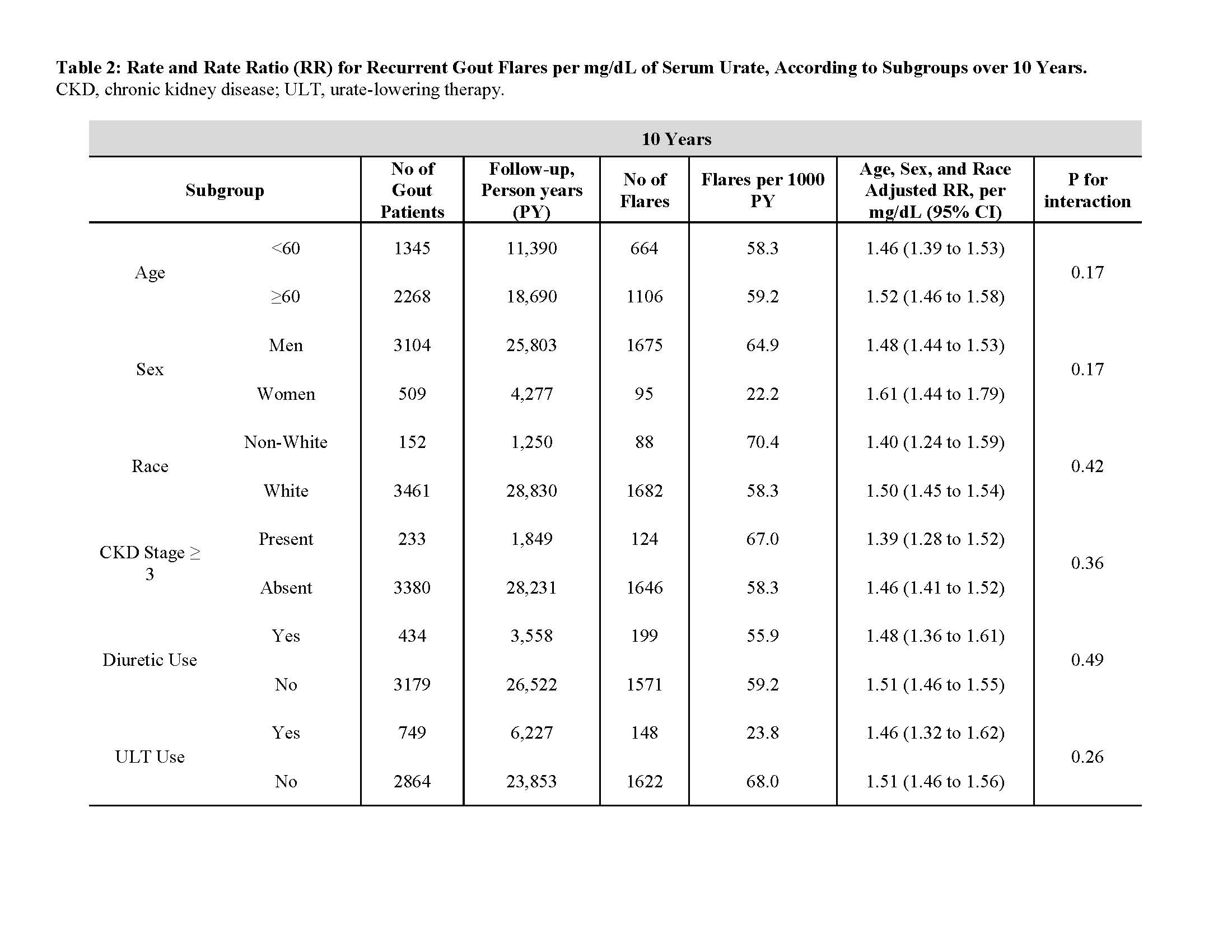
Results: We followed 3,613 prevalent gout patients (86% male, mean age 60 years), among whom we documented 1,770 gout flare events over 10 years.95% (1,676/1,770) and 98% (1,728/1,770) of flares occurred in baseline SU ≥6 and ≥5 mg/dL, respectively. Rate ratio (RR) for flares with SU levels of < 6.0, 6.0-6.9, 7.0-7.9, 8.0-8.9, 9.0-9.9, and ≥10 mg/dL were 1.0, 5.03, 11.64, 11.81, 18.95, and 29.13, respectively during first year of follow-up (1.59 [1.48-1.71] per mg/dL), and 1.0, 3.38, 6.93, 8.57, 10.93, and 11.40, respectively, over whole 10-year follow-up (1.49 [1.45-1.53] per mg/dL) (Table 1).Associations persisted irrespective of sex, race, age group, chronic kidney disease status, and diuretic and urate-lowering therapy use (all P for interaction >0.17) (Table 2). 97% (62/64) and 100% (64/64) of flares requiring hospitalization occurred in baseline SU ≥6 and ≥5 mg/dL, respectively (Table 3); corresponding RR were 1.0, 4.77, 9.02, 10.58, 34.36, and 46.43, respectively (1.77 [1.53-2.05] per mg/dL).
Conclusion: In this prospective cohort of gout patients treated in primary care, 95% and 98% of flares occurred in baseline SU ≥6 and ≥5 mg/dL, respectively. Associations were more prominent for hospitalized flares, with no cases among those with SU < 5mg/dL; higher serum urate levels are strongly associated with frequency of recurrent flares in a graded manner. These findings support the utility of these target urate levels for gout patient care, consistent with a treat-to-target approach recommended by rheumatology societies in the US and Europe, but not the American College of Physicians.
.jpg)
N. McCormick: None; C. Yokose: None; G. Challener: None; A. Joshi: Regeneron, 3; S. Tanikella: None; H. Choi: Ani, 2, Horizon, 2, 5, LG, 2, Protalix, 2, Shanton, 2.
Background/Purpose: Despite rheumatology guidelines' emphasis on treat-to-target-serum-urate (SU) levels (<6 or <5 mg/dL, urate crystal sub-saturation points), this pathophysiology-based recommendation is not accepted in primary care practice (where >90% of gout care occurs) or endorsed by the American College of Physicians.To that end, proportions of gout flares associated with these target levels, including those requiring hospitalization, are unknown. We quantified associations of target SU with recurrent flares, including gout-primary hospitalizations, among gout patients nested in a prospective nationwide cohort.
Methods: This was a prospective cohort study of UK adults recruited over 2006-2010 and followed-up through primary care medical record linkage. As done previously [Cipolletta et al. JAMA 2022], flares among prevalent gout patients were ascertained by (1) hospitalization with gout (ICD-10 M10) as primary discharge diagnosis; (2) diagnosis of gout flare in primary care records; or (3) diagnosis of gout in primary care records and prescription issued on the same day for corticosteroids, colchicine, or non-steroidal anti-inflammatory drugs (NSAIDs).We also investigated flares requiring hospitalisation. Poisson regression was used to assess the relation between baseline SU levels and rates of recurrent gout flares over 1, 2, 5, and 10 years of follow-up.
Results: We followed 3,613 prevalent gout patients (86% male, mean age 60 years), among whom we documented 1,770 gout flare events over 10 years.95% (1,676/1,770) and 98% (1,728/1,770) of flares occurred in baseline SU ≥6 and ≥5 mg/dL, respectively. Rate ratio (RR) for flares with SU levels of < 6.0, 6.0-6.9, 7.0-7.9, 8.0-8.9, 9.0-9.9, and ≥10 mg/dL were 1.0, 5.03, 11.64, 11.81, 18.95, and 29.13, respectively during first year of follow-up (1.59 [1.48-1.71] per mg/dL), and 1.0, 3.38, 6.93, 8.57, 10.93, and 11.40, respectively, over whole 10-year follow-up (1.49 [1.45-1.53] per mg/dL) (Table 1).Associations persisted irrespective of sex, race, age group, chronic kidney disease status, and diuretic and urate-lowering therapy use (all P for interaction >0.17) (Table 2). 97% (62/64) and 100% (64/64) of flares requiring hospitalization occurred in baseline SU ≥6 and ≥5 mg/dL, respectively (Table 3); corresponding RR were 1.0, 4.77, 9.02, 10.58, 34.36, and 46.43, respectively (1.77 [1.53-2.05] per mg/dL).
Conclusion: In this prospective cohort of gout patients treated in primary care, 95% and 98% of flares occurred in baseline SU ≥6 and ≥5 mg/dL, respectively. Associations were more prominent for hospitalized flares, with no cases among those with SU < 5mg/dL; higher serum urate levels are strongly associated with frequency of recurrent flares in a graded manner. These findings support the utility of these target urate levels for gout patient care, consistent with a treat-to-target approach recommended by rheumatology societies in the US and Europe, but not the American College of Physicians.

Table 1. Rate and Rate Ratio (RR) for Recurrent Gout Flares According to Serum Urate Level and Follow-Up Time from Baseline.
No, number; PY, person years; 95% CI, 95% confidence interval.
No, number; PY, person years; 95% CI, 95% confidence interval.

Table 2: Rate and Rate Ratio (RR) for Recurrent Gout Flares per mg/dL of Serum Urate, According to Subgroups over 10 Years.
CKD, chronic kidney disease; ULT, urate-lowering therapy; SD, standard deviation.
CKD, chronic kidney disease; ULT, urate-lowering therapy; SD, standard deviation.
.jpg)
Table 3: Rate and Rate Ratios (RR) for Recurrent Gout Flares Requiring Hospitalization
No, number; PY, person years; SD, standard deviation; 95% CI, 95% confidence interval. Hospitalizations were ascertained through March 5, 2020 (max 12.8 years follow-up)
No, number; PY, person years; SD, standard deviation; 95% CI, 95% confidence interval. Hospitalizations were ascertained through March 5, 2020 (max 12.8 years follow-up)
N. McCormick: None; C. Yokose: None; G. Challener: None; A. Joshi: Regeneron, 3; S. Tanikella: None; H. Choi: Ani, 2, Horizon, 2, 5, LG, 2, Protalix, 2, Shanton, 2.



