Poster Session B
Myopathic rheumatic diseases (polymyositis, dermatomyositis, inclusion body myositis)
Session: (1155–1182) Muscle Biology, Myositis & Myopathies – Basic & Clinical Science Poster II
1175: Inclusion of All Myositis Specific Autoantibodies or Other Rashes Leads to Better Sensitivity but Lower Specificity of 2017 EULAR/ACR Myositis Classification Criteria for Dermatomyositis
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- YH
Yusra Hasan, MD
CHI Health Creighton university medical center
Omaha, NE, United StatesDisclosure information not submitted.
Abstract Poster Presenter(s)
Yusra Hasan1, Katharine Ching Chung2, Dana Ascherman3, Siamak Moghadam-Kia4, Chester V. Oddis3 and Rohit Aggarwal3, 1CHI Health Creighton University Medical Center, Omaha, NE, 2University of Pittsburgh Medical Center, Mckeesport, PA, 3University of Pittsburgh, Pittsburgh, PA, 4University of Pittsburgh Medical Center, Pittsburgh, PA
Background/Purpose: Idiopathic Inflammatory Myopathies (IIM), collectively known as myositis, are heterogeneous disorders characterized by muscle weakness and muscle inflammation. ACR/EULAR classification criterion for IIM was published in 2016 that showed the sensitivity and specificity for probable diagnosis 87%/82% without biopsies, and 93%/88% with biopsies. The criteria is currently being used in most clinical trials and research studies. However, it has been criticized for its lack of a full panel of autoantibodies as well as the non-inclusion of other Dermatomyositis-specific rashes. The aim of our study was to evaluate if the addition of other myositis-specific antibodies (MSAs) and/or DM rashes other than Gottron papules/sign or heliotrope rash would improve the accuracy of the criteria.
Methods: Data were obtained from a prospectively collected myositis registry at a single tertiary care center but retrospectively extracted in subjects with an initial visit between 1995 to 2020. The classification criteria dataset included all variables of 2017 EULAR/ACR as well as Bohan and Peter myositis classification criteria.Additional variables were verified by chart review if/when required and all variables and scores were cross-checked by 2 physicians. Classification scores were re-calculated by adding:
Results: 798 patients with IIM including 268 with dermatomyositis, 41 with clinically amyopathic dermatomyositis (CADM). In our analysis, 2017 EULAR/ACR showed 91% accuracy, with high sensitivity (87% and 73%) and specificity (94%, and 93%), with and without muscle biopsy, respectively. Bohan and Peter showed lower sensitivity and specificity of 57% and 74% respectively.
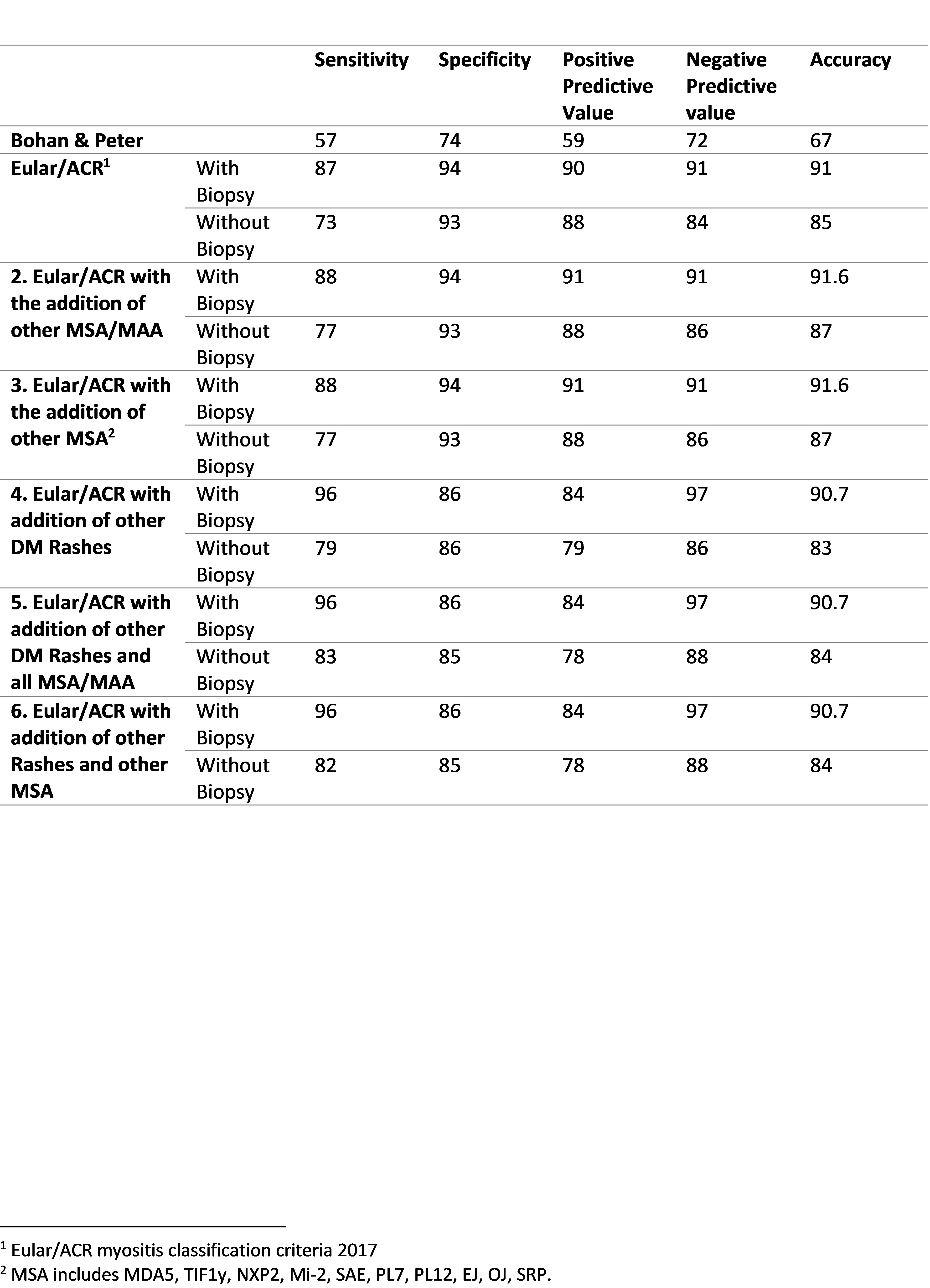
The modification of adding other MSA/MAA along with Anti Jo1 leads to a minor improvement in sensitivity (88% and 77% with and without biopsy respectively) without loss of specificity. Adding other DM rashes with Gottron papules increases sensitivity significantly (96% and 79% with and without biopsy, respectively) but with a decrease in specificity (86%). (Table 1)
The modification of adding other MSA/MAA as well as other DM rashes together improves sensitivity the best but at the cost of specificity.
Conclusion: The addition of other skin rashes and/or MSA to the 2016 EULAR/ACR criteria improves sensitivity but at a cost of specificity. Modification of the EULAR/ACR classification criteria is required to overcome some of the shortcomings of the current criteria.
Y. Hasan: None; K. Chung: None; D. Ascherman: None; S. Moghadam-Kia: None; C. V. Oddis: Boehringer-Ingelheim, 5, Cabaletta, 5, EMD Serono, 5, Novartis, 5, Pfizer, 1; R. Aggarwal: Actigraph, 2, Alexion, 2, ANI Pharmaceuticals, 2, Argenx, 2, AstraZeneca, 2, Boehringer-Ingelheim, 2, 5, Bristol-Myers Squibb(BMS), 2, 5, CabalettaBio, 2, Capella Bioscience, 2, Corbus, 2, CSL Behring, 2, EMD Serono, 2, 5, Galapagos, 2, Horizon Therapeutics, 2, I-Cell, 2, Janssen, 2, 5, Kezar, 2, Kyverna, 2, Mallinckrodt, 5, Merck, 2, Octapharma, 2, Pfizer, 2, 5, Q32, 5, Roivant, 2, Sanofi, 2, Teva, 2.
Background/Purpose: Idiopathic Inflammatory Myopathies (IIM), collectively known as myositis, are heterogeneous disorders characterized by muscle weakness and muscle inflammation. ACR/EULAR classification criterion for IIM was published in 2016 that showed the sensitivity and specificity for probable diagnosis 87%/82% without biopsies, and 93%/88% with biopsies. The criteria is currently being used in most clinical trials and research studies. However, it has been criticized for its lack of a full panel of autoantibodies as well as the non-inclusion of other Dermatomyositis-specific rashes. The aim of our study was to evaluate if the addition of other myositis-specific antibodies (MSAs) and/or DM rashes other than Gottron papules/sign or heliotrope rash would improve the accuracy of the criteria.
Methods: Data were obtained from a prospectively collected myositis registry at a single tertiary care center but retrospectively extracted in subjects with an initial visit between 1995 to 2020. The classification criteria dataset included all variables of 2017 EULAR/ACR as well as Bohan and Peter myositis classification criteria.Additional variables were verified by chart review if/when required and all variables and scores were cross-checked by 2 physicians. Classification scores were re-calculated by adding:
- all non-Jo1 MSA/MAA receiving the same score as Jo-1,
- all other DM rashes except Gottron papule/sign, and heliotrope (i.e., shawl sign, V-neck, holster sign, malar rash not sparing nasolabial fold, mechanics hands, periorbital edema) receiving the same score as Gottron papules.
- both a & b.
Results: 798 patients with IIM including 268 with dermatomyositis, 41 with clinically amyopathic dermatomyositis (CADM). In our analysis, 2017 EULAR/ACR showed 91% accuracy, with high sensitivity (87% and 73%) and specificity (94%, and 93%), with and without muscle biopsy, respectively. Bohan and Peter showed lower sensitivity and specificity of 57% and 74% respectively.
The modification of adding other MSA/MAA along with Anti Jo1 leads to a minor improvement in sensitivity (88% and 77% with and without biopsy respectively) without loss of specificity. Adding other DM rashes with Gottron papules increases sensitivity significantly (96% and 79% with and without biopsy, respectively) but with a decrease in specificity (86%). (Table 1)
The modification of adding other MSA/MAA as well as other DM rashes together improves sensitivity the best but at the cost of specificity.
Conclusion: The addition of other skin rashes and/or MSA to the 2016 EULAR/ACR criteria improves sensitivity but at a cost of specificity. Modification of the EULAR/ACR classification criteria is required to overcome some of the shortcomings of the current criteria.

Psychometric properties of IIM classification criteria and proposed modifications.
Y. Hasan: None; K. Chung: None; D. Ascherman: None; S. Moghadam-Kia: None; C. V. Oddis: Boehringer-Ingelheim, 5, Cabaletta, 5, EMD Serono, 5, Novartis, 5, Pfizer, 1; R. Aggarwal: Actigraph, 2, Alexion, 2, ANI Pharmaceuticals, 2, Argenx, 2, AstraZeneca, 2, Boehringer-Ingelheim, 2, 5, Bristol-Myers Squibb(BMS), 2, 5, CabalettaBio, 2, Capella Bioscience, 2, Corbus, 2, CSL Behring, 2, EMD Serono, 2, 5, Galapagos, 2, Horizon Therapeutics, 2, I-Cell, 2, Janssen, 2, 5, Kezar, 2, Kyverna, 2, Mallinckrodt, 5, Merck, 2, Octapharma, 2, Pfizer, 2, 5, Q32, 5, Roivant, 2, Sanofi, 2, Teva, 2.



