Poster Session B
Myopathic rheumatic diseases (polymyositis, dermatomyositis, inclusion body myositis)
Session: (1155–1182) Muscle Biology, Myositis & Myopathies – Basic & Clinical Science Poster II
1169: All-cause Mortality and Risk Factors for Death in a Large Multi-center Prospective Registry Cohort of Idiopathic Inflammatory Myositis in China
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- LP
Abstract Poster Presenter(s)
Liying Peng1, Peng Yin2, Mucong Li3, Qian Wang4, Yanhong wang1, Shuang Zhou4, chanyuan wu4, Jiuliang zhao1, Dong xu5, Mengtao Li3 and xiaofeng Zeng4, 1Peking Union Medical College, Beijing, China, 2Chinese Center for Disease Control and Prevention, Beijing, China, 3Peking Union Medical College Hospital, Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing, China, 4Department of Rheumatology, Peking Union Medical College Hospital, Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing, China, 5Peking Union Medical College Hospital, Beijing, China
Background/Purpose: Our study depicted the mortality and independent risk factors of IIM patients in a large multi-center prospective registry cohort in China.
Methods: Patients registered before 31st, December 2021 in the Chinese Rheumatism Data Center-Myositis Registry (CRDC-MYO) were included. Juvenile patients, patients with malignancy at baseline, or patients complicated with other CTD were excluded. Baseline and follow-up data were collected from CRDC-MYO registry database. Death information was obtained from the Chinese Center for Disease Control and Prevention's disease surveillance points system. Kaplan-Meier Curves and Log-rank test was used to compare the mortality. Univariable and multivariable Cox hazards regression analysis were used to identify potential risk factors for death.
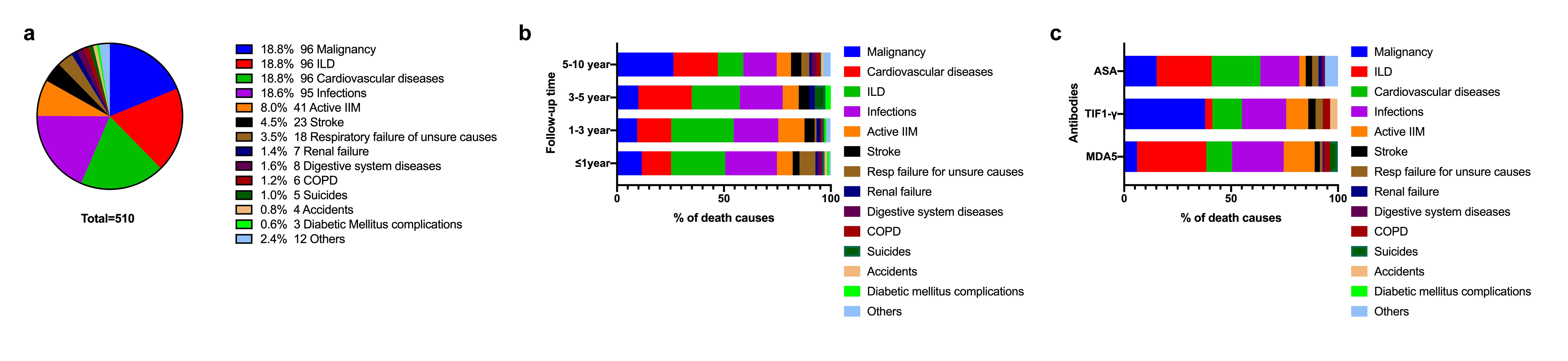
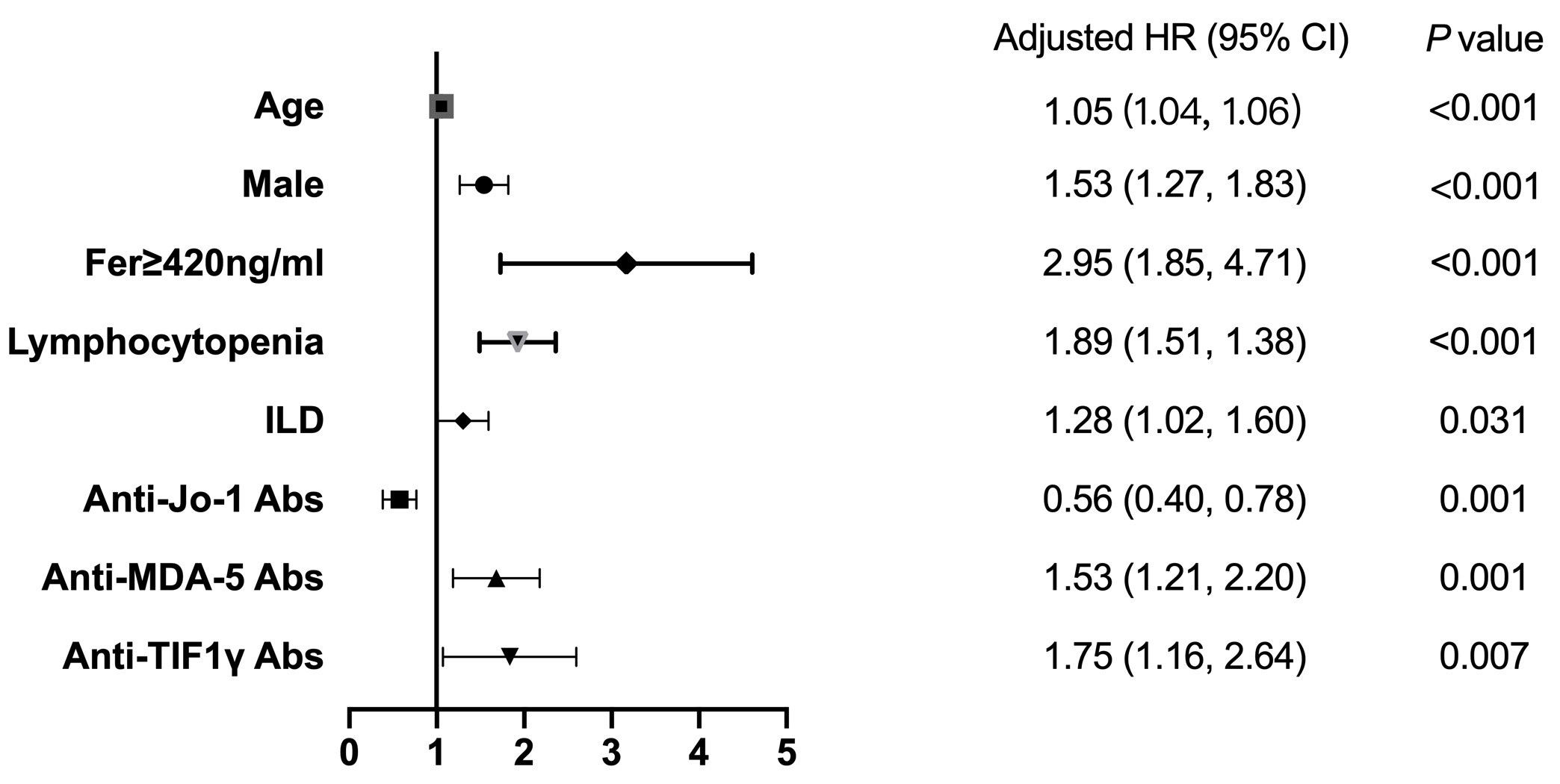
Results: 4534 IIM cases were finally enrolled, including 2902 dermatomyositis (64.0%), 592 polymyositis (13.1%), 927 antisynthetase syndrome (20.4%), and 113 immune-mediated necrotising myopathy (2.5%). 510 deaths in total were recorded. The cumulative survival at 1, 3, 5 and 10 years were 92.6%, 88.6%, 86.2%, and 80.5% (Figure 1a). Significant differences (P< 0.05) in survival between different subgroups (Figure 1b) as well as different myositis-specific antibodies were confirmed by log-rank test (Figure 1c). Malignancy (18.8%), interstitial lung disease (18.8%), cardiovascular diseases (18.8%), and infections (18.6%) were the most common causes of deaths (Figure 2a). We observed a shift in the predominant causes of death from pulmonary interstitial disease and infection within the initial three-year period to tumor and cardiovascular diseases in the subsequent years as the follow-up time extended (Figure 2b). There is significant variation in the composition of causes of death among myositis patients with different antibodies (Figure 2c). Patients with positive anti-TIF1γ antibody commonly succumb to malignancies, whereas patients with positive anti-MDA5 antibody and anti-Jo-1 antibody frequently experience mortality due to interstitial lung disease. Multivariable Cox regression analysis confirmed male (HR=1.53, 95%CI 1.27-1.83), ferritin≥420ng/ml (2.95 [1.85-4.71]), lymphocytopenia (1.89 [1.51-1.38]), ILD (1.28 [1.02-1.60]), anti-MDA-5 antibody (1.53 [1.21-2.20]), and anti-TIF1γ antibody (1.75 [1.16-2.64]) as independent risk factors, and anti-Jo-1 antibody (0.56 [0.40-0.78]) as protective factor for mortality after adjusting for age (Figure 3).
Conclusion: Patients with positive anti-MDA5 antibody exhibited the most rapid decline in survival rate during the first year, whereas patients with anti-TIF1γ antibody had a worse prognosis over a longer follow-up period. This might be attributed to the fact that causes of mortality among myositis patients vary over time, with anti-TIF1γ-positive patients being more susceptible to malignancies. In addition to interstitial lung disease, myositis-specific antibodies appeared to exert a more decisive influence on the prognosis of myositis patients compared to other clinical manifestations. This suggests that future classification of myositis patients based on myositis-specific antibodies might be more rational.
.jpg)
L. Peng: None; P. Yin: None; M. Li: None; Q. Wang: None; Y. wang: None; S. Zhou: None; c. wu: None; J. zhao: None; D. xu: None; M. Li: None; x. Zeng: None.
Background/Purpose: Our study depicted the mortality and independent risk factors of IIM patients in a large multi-center prospective registry cohort in China.
Methods: Patients registered before 31st, December 2021 in the Chinese Rheumatism Data Center-Myositis Registry (CRDC-MYO) were included. Juvenile patients, patients with malignancy at baseline, or patients complicated with other CTD were excluded. Baseline and follow-up data were collected from CRDC-MYO registry database. Death information was obtained from the Chinese Center for Disease Control and Prevention's disease surveillance points system. Kaplan-Meier Curves and Log-rank test was used to compare the mortality. Univariable and multivariable Cox hazards regression analysis were used to identify potential risk factors for death.
Results: 4534 IIM cases were finally enrolled, including 2902 dermatomyositis (64.0%), 592 polymyositis (13.1%), 927 antisynthetase syndrome (20.4%), and 113 immune-mediated necrotising myopathy (2.5%). 510 deaths in total were recorded. The cumulative survival at 1, 3, 5 and 10 years were 92.6%, 88.6%, 86.2%, and 80.5% (Figure 1a). Significant differences (P< 0.05) in survival between different subgroups (Figure 1b) as well as different myositis-specific antibodies were confirmed by log-rank test (Figure 1c). Malignancy (18.8%), interstitial lung disease (18.8%), cardiovascular diseases (18.8%), and infections (18.6%) were the most common causes of deaths (Figure 2a). We observed a shift in the predominant causes of death from pulmonary interstitial disease and infection within the initial three-year period to tumor and cardiovascular diseases in the subsequent years as the follow-up time extended (Figure 2b). There is significant variation in the composition of causes of death among myositis patients with different antibodies (Figure 2c). Patients with positive anti-TIF1γ antibody commonly succumb to malignancies, whereas patients with positive anti-MDA5 antibody and anti-Jo-1 antibody frequently experience mortality due to interstitial lung disease. Multivariable Cox regression analysis confirmed male (HR=1.53, 95%CI 1.27-1.83), ferritin≥420ng/ml (2.95 [1.85-4.71]), lymphocytopenia (1.89 [1.51-1.38]), ILD (1.28 [1.02-1.60]), anti-MDA-5 antibody (1.53 [1.21-2.20]), and anti-TIF1γ antibody (1.75 [1.16-2.64]) as independent risk factors, and anti-Jo-1 antibody (0.56 [0.40-0.78]) as protective factor for mortality after adjusting for age (Figure 3).
Conclusion: Patients with positive anti-MDA5 antibody exhibited the most rapid decline in survival rate during the first year, whereas patients with anti-TIF1γ antibody had a worse prognosis over a longer follow-up period. This might be attributed to the fact that causes of mortality among myositis patients vary over time, with anti-TIF1γ-positive patients being more susceptible to malignancies. In addition to interstitial lung disease, myositis-specific antibodies appeared to exert a more decisive influence on the prognosis of myositis patients compared to other clinical manifestations. This suggests that future classification of myositis patients based on myositis-specific antibodies might be more rational.
.jpg)
Figure 1 Kaplan-Meier curves for: a. the entire idiopathic inflammatory myositis patients in Chinese Rheumatism Data Center-Myositis Registry (CRDC-MYO); b. patients in different myositis subtypes; c. patients with different myositis-specific antibodies.

Figure 2 a. Death causes of IIM patients in CRDC-MYO registry. b. Death causes during various follow-up periods. c. Death causes among patients with varying myositis-specific antibody profiles.

Figure 3 Independent risk factors for death after adjusting for age using multivariable Cox regression analysis.
L. Peng: None; P. Yin: None; M. Li: None; Q. Wang: None; Y. wang: None; S. Zhou: None; c. wu: None; J. zhao: None; D. xu: None; M. Li: None; x. Zeng: None.



