Poster Session B
Periodic fever syndromes, autoinflammatory diseases, Still’s disease and MAS/HLH
Session: (1124–1154) Miscellaneous Rheumatic & Inflammatory Diseases Poster II
1131: Clinical Phenotypes of IgG4-related Disease in a Multi-ethnic Singapore Cohort
Monday, November 13, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- CC
Choon-Guan Chua, MRCP (he/him/his)
National Healthcare Group (NHG)
Singapore, SingaporeDisclosure information not submitted.
Abstract Poster Presenter(s)
Choon Guan Chua1, Weida Chew1, Jeggrey Kay Wee Kam1, Hwee-Pin Phua1, Chengzi Chow1, Carol Yee-Leng Ng1, Wei-Yen Lim1, Ru Sin Lim1, Jereme Yijin Gan1, Mung-Ee Loh1, Tianrong Yeo2, David Zhiwei Law1, Stephrene Seok Wei Chan3, Amanda Francesca Ya-Fang Cheang4, Yong-Howe Ho1 and Charles Kien-Fong Vu1, 1Tan Tock Seng Hospital, Singapore, Singapore, 2National Neurology Institute, Singapore, Singapore, 3National University Hospital, Singapore, Singapore, 4Woodlands Health Campus, Singapore, Singapore
Background/Purpose: IgG4-related disease (IgG4-RD) is an immune-mediated condition that is heterogenous and can result in organ failure. To understand the disease profile of our local population better, a multi-disciplinary team was formed to review the IgG4-RD patients seen in our hospital.
Methods: A chart review was undertaken for all IgG4-RD patients seen between 1 January 2015 and 30 September 2021 at a major tertiary hospital in Singapore. All patients included fulfilled the 2020 revised comprehensive diagnostic (RCD) criteria for IgG4-RD for at least possible IgG4-RD and then scored according to the 2019 ACR/EULAR classification.
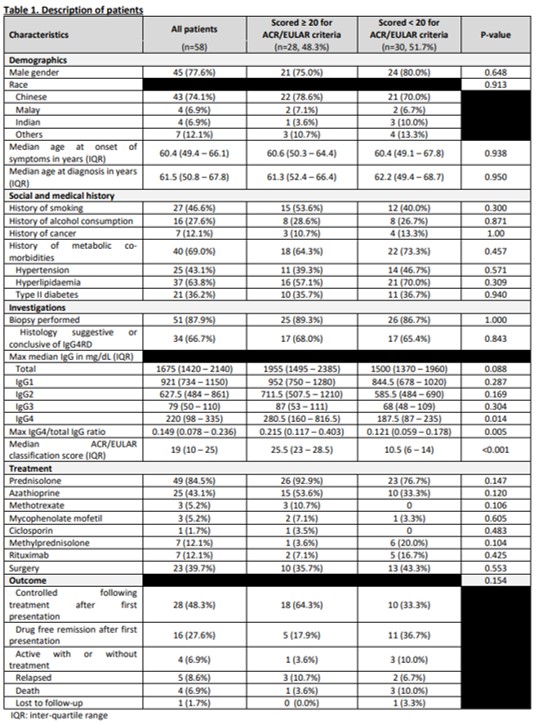
Results: Of the 58 patients included in this study, 28 scored at least 20 (i.e. completely fulfilled) for the 2019 ACR/EULAR classification criteria. 45/58 (77.6%) were male, 43/58 (74.1%) were Chinese, and median age at onset of symptoms and at diagnosis were 60.4 [inter-quartile range (IQR) 49.4-66.1] and 61.5 (IQR 50.8-67.8) years respectively. 27/58 (46.6%) were smokers, 7/58 (12.1%) had cancers, and 40/58 (69.0%) had underlying metabolic co-morbidities. Patients who completely fulfilled the ACR/EULAR classification criteria scored between 21 and 44 (median 25.5), and those who did not fulfil had a score of 4 to 19 (median 10.5). The distribution of clinical phenotypes were: 22/58 (37.9%) head and neck, 20/58 (34.5%) pancreato-biliary, 12/58 (20.7%) Mikulicz/systemic, and 4/58 (6.9%) retro-peritoneal fibrosis/aortitis. The three commonest sites of involvement were pancreato-hepato-biliary 26/58 (44.8%), ocular 17/58 (29.3%) and lymph nodes 14/58 (24.1%). The median maximum serum IgG4 level and median IgG4/total IgG ratio were 220mg/dL (IQR 98-335) and 0.149 (IQR 0.078-0.236) respectively. Patients with Mikulicz/systemic phenotype had significantly higher median total serum IgG, IgG1, IgG2 and IgG3 (p< 0.050). The median maximum serum IgG4 level for those who fulfilled the ACR/EULAR criteria was 280.5mg/dL (IQR 160-816.5) and those who did not fulfil was 187.5mg/dL (87-235) (p=0.014). Histological samples were suggestive/conclusive of IgG4-RD in 68% of patients who completely fulfilled the ACR/EULAR classification criteria and 65.4% of patients who did not (p=0.843). Prednisolone was the commonest treatment prescribed to patients (49/58, 84.5%). Steroid-sparing immunosuppressants were given to 32/58 (55.2%), for which azathioprine was the commonest (25/58, 43.1%) followed by rituximab (7/58, 12.1%). Surgical excision was done in 23/58 (39.7%). 44/58 (75.9%) patients achieved disease remission after first presentation and 16/58 (27.6%) were in drug-free remission. Mortality was 4/58 (6.9%) with one case attributable to complications of IgG4-RD.
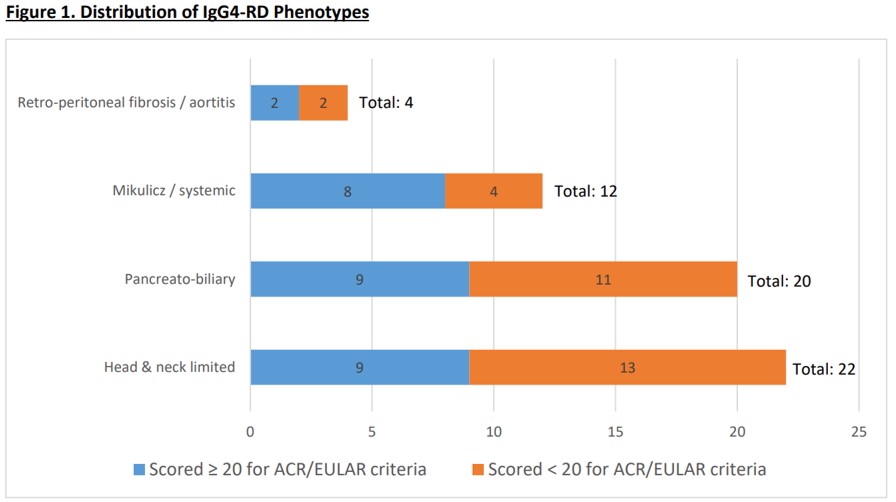
Conclusion: The head and neck IgG4-RD phenotype was the commonest one in our cohort, followed by pancreato-biliary. This condition occurred more commonly in males with no gender pre-dilection in any clinical phenotype. The ACR/EULAR classification criteria appeared too restrictive and the 2020 RCD was better able to capture the full spectral of IgG4-RD patients. The overall prognosis for IgG4-RD is good and histological investigation remains important for the diagnosis of this disease.

C. Chua: None; W. Chew: None; J. Kam: None; H. Phua: None; C. Chow: None; C. Ng: None; W. Lim: None; R. Lim: None; J. Gan: None; M. Loh: None; T. Yeo: None; D. Law: None; S. Chan: None; A. Cheang: None; Y. Ho: None; C. Vu: None.
Background/Purpose: IgG4-related disease (IgG4-RD) is an immune-mediated condition that is heterogenous and can result in organ failure. To understand the disease profile of our local population better, a multi-disciplinary team was formed to review the IgG4-RD patients seen in our hospital.
Methods: A chart review was undertaken for all IgG4-RD patients seen between 1 January 2015 and 30 September 2021 at a major tertiary hospital in Singapore. All patients included fulfilled the 2020 revised comprehensive diagnostic (RCD) criteria for IgG4-RD for at least possible IgG4-RD and then scored according to the 2019 ACR/EULAR classification.
Results: Of the 58 patients included in this study, 28 scored at least 20 (i.e. completely fulfilled) for the 2019 ACR/EULAR classification criteria. 45/58 (77.6%) were male, 43/58 (74.1%) were Chinese, and median age at onset of symptoms and at diagnosis were 60.4 [inter-quartile range (IQR) 49.4-66.1] and 61.5 (IQR 50.8-67.8) years respectively. 27/58 (46.6%) were smokers, 7/58 (12.1%) had cancers, and 40/58 (69.0%) had underlying metabolic co-morbidities. Patients who completely fulfilled the ACR/EULAR classification criteria scored between 21 and 44 (median 25.5), and those who did not fulfil had a score of 4 to 19 (median 10.5). The distribution of clinical phenotypes were: 22/58 (37.9%) head and neck, 20/58 (34.5%) pancreato-biliary, 12/58 (20.7%) Mikulicz/systemic, and 4/58 (6.9%) retro-peritoneal fibrosis/aortitis. The three commonest sites of involvement were pancreato-hepato-biliary 26/58 (44.8%), ocular 17/58 (29.3%) and lymph nodes 14/58 (24.1%). The median maximum serum IgG4 level and median IgG4/total IgG ratio were 220mg/dL (IQR 98-335) and 0.149 (IQR 0.078-0.236) respectively. Patients with Mikulicz/systemic phenotype had significantly higher median total serum IgG, IgG1, IgG2 and IgG3 (p< 0.050). The median maximum serum IgG4 level for those who fulfilled the ACR/EULAR criteria was 280.5mg/dL (IQR 160-816.5) and those who did not fulfil was 187.5mg/dL (87-235) (p=0.014). Histological samples were suggestive/conclusive of IgG4-RD in 68% of patients who completely fulfilled the ACR/EULAR classification criteria and 65.4% of patients who did not (p=0.843). Prednisolone was the commonest treatment prescribed to patients (49/58, 84.5%). Steroid-sparing immunosuppressants were given to 32/58 (55.2%), for which azathioprine was the commonest (25/58, 43.1%) followed by rituximab (7/58, 12.1%). Surgical excision was done in 23/58 (39.7%). 44/58 (75.9%) patients achieved disease remission after first presentation and 16/58 (27.6%) were in drug-free remission. Mortality was 4/58 (6.9%) with one case attributable to complications of IgG4-RD.
Conclusion: The head and neck IgG4-RD phenotype was the commonest one in our cohort, followed by pancreato-biliary. This condition occurred more commonly in males with no gender pre-dilection in any clinical phenotype. The ACR/EULAR classification criteria appeared too restrictive and the 2020 RCD was better able to capture the full spectral of IgG4-RD patients. The overall prognosis for IgG4-RD is good and histological investigation remains important for the diagnosis of this disease.

Description of patients

Distribution of IgG4-related disease phenotypes

Sites of IgG4-related disease manifestations
C. Chua: None; W. Chew: None; J. Kam: None; H. Phua: None; C. Chow: None; C. Ng: None; W. Lim: None; R. Lim: None; J. Gan: None; M. Loh: None; T. Yeo: None; D. Law: None; S. Chan: None; A. Cheang: None; Y. Ho: None; C. Vu: None.



