Poster Session A
Fibrosing rheumatic diseases (scleroderma, MCTD, IgG4-related disease, scleroderma mimics)
Session: (0609–0672) Systemic Sclerosis & Related Disorders – Clinical Poster I: Research
0669: Optical Coherence Tomography Angiography in Systemic Sclerosis: Correlations with Morphological and Functional Peripheral Microvascular Status
Sunday, November 12, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
.png)
Maurizio Cutolo, MD
University of Genova
Genova, Genoa, ItalyDisclosure(s): BI: Grant/Research Support (Ongoing)
Abstract Poster Presenter(s)
Carlo Alberto Cutolo1, Elvis Hysa2, Andrea Cere3, Paola Toma1, Tommaso Cannavacciuolo1, Chiara Toma1, Serena Balito4, Veronica Gerli4, Alberto Sulli3, Vanessa Smith5, Carlo Enrico Traverso1, Massimo Nicolò1 and Maurizio Cutolo6, 1Ophthalmology Clinic DiNOGMI, IRCCS Ophthalmology Unit San Martino Polyclinic, University of Genoa, Genoa, Italy, 2Laboratory of Experimental Rheumatology and Academic Division of Clinical Rheumatology, Department of Internal Medicine, University of Genova, IRCCS San Martino Polyclinic Hospital, Genova, Italy, 3Laboratory of Experimental Rheumatology and Academic Division of Rheumatology, Department of Internal Medicine, University of Genoa, IRCCS San Martino Polyclinic Hospital, Genoa, Italy, 4Laboratory of Experimental Rheumatology and Academic Division of Clinical Rheumatology, Department of Internal Medicine, University of Genoa, Italy - IRCCS San Martino Polyclinic, Genoa, Italy, 5Ghent University Hospital, Gent, Belgium, 6Laboratory of Experimental Rheumatology, Division of Clinical Rheumatology, Department of Internal Medicine, University of Genova, IRCCS San Martino Polyclinic, Genova, Italy
Background/Purpose: Systemic sclerosis (SSc) is a rare and complex autoimmune disease featured by a progressive microvascular damage. The involvement of the ocular microvasculature has been reported in SSc but correlations with nailfold capillaroscopy (NVC) and laser speckle contrast analysis (LASCA) have been scarcely investigated [1].
We aimed to compare Optical Coherence Tomography Angiography (OCTA) variables in SSc patients vs age- and sex- matched healthy controls (HCs). The morphological peripheral microvascular status, assessed by NVC, and the functional perfusion, analysed by LASCA, were correlated with the OCTA data among the SSc cohort.
Methods: The enrolment included 35 SSc patients (mean age 61.1 ± 13.4 years, mean disease duration 9.5 ± 6 years) and 28 HCs in a single centre from March to October 2022.
The patients were classified according to the ACR/EULAR 2013 criteria, and multiple assessments were performed, at the same day, including ophthalmological examinations, OCTA, NVC and LASCA.
The clinical, laboratory and instrumental data of SSc patients were analysed and correlated with the OCTA data.
Patients were under standard treatment for SSc and those requiring endovenous prostanoids were evaluated for the study assessment at least one month after the last infusion.
Results: Among the ocular features, the intraocular pressure (IOP) was significantly higher in SSc than in HCs (p=0.006).
Despite the structural features in OCTA being similar, a significant difference was detected in all the perfusion variables, including the superficial vascular plexus (SVP), deep vascular plexus (DVP), and choriocapillaris (CC) (Table 1).
When patients were stratified according to the clinical extension of skin involvement, diffuse cutaneous SSc (dcSSc) patients showed a significantly reduced CC perfusion compared to limited cutaneous SSc (lcSSc) patients. Interestingly, the choroidal thickness (CT) in dcSSc was nearly twice that of lcSSc (p < 0.0001). The age and disease duration did not significantly differ among the two subgroups (respectively, p = 0.18 and p = 0.37).
In addition, the mean number of capillaries per linear mm at NVC and the mean peripheral perfusion assessed by LASCA at the level of 2nd to 5th fingertip were negatively correlated with the IOP (r = -0.30 and r = -0.36, both p < 0.01).
Finally, the mean capillary number at NVC was also positively correlated with the perfusion values of the SVP and DVP at OCTA (r = 0.3, p = 0.01 and r = 0.28, p = 0.01) and the mean peripheral perfusion detected by LASCA positively correlated with the DVP and CC perfusion (r = 0.29 and r = 0.28, both p = 0.01).
Conclusion: The higher IOP in all SSc patients might be in line with reported vascular abnormalities occurring in the optic nerve head [2].
The reduced capillary density and perfusion of the retina and choriocapillaris suggest an ocular microvascular impairment similarly to what is observed at the nailfold and fingertips in SSc patients.
The increased CT limited to dcSSc might be related to attempts of ocular microvascular reactivity and deposition of sub-endothelial extracellular matrix in agreement with the fibrotic process observed in other tissues in such patients.
References: [1] Kreps et al. Semin Arthr Rheum 2019. [2] Hysa et al. Aut Rev 2021
C. Cutolo: None; E. Hysa: None; A. Cere: None; P. Toma: None; T. Cannavacciuolo: None; C. Toma: None; S. Balito: None; V. Gerli: None; A. Sulli: None; V. Smith: Boehringer Ingelheim, 2, 5, 6, 12, Support for travel, Galapagos, 6, Janssen-Cilag, 1, 2, 5, 6; C. Traverso: None; M. Nicolò: None; M. Cutolo: Amgen, 5, Boehringer Ingelheim, 5, Bristol-Myers Squibb, 5, Lab.Baldacci, 5.
Background/Purpose: Systemic sclerosis (SSc) is a rare and complex autoimmune disease featured by a progressive microvascular damage. The involvement of the ocular microvasculature has been reported in SSc but correlations with nailfold capillaroscopy (NVC) and laser speckle contrast analysis (LASCA) have been scarcely investigated [1].
We aimed to compare Optical Coherence Tomography Angiography (OCTA) variables in SSc patients vs age- and sex- matched healthy controls (HCs). The morphological peripheral microvascular status, assessed by NVC, and the functional perfusion, analysed by LASCA, were correlated with the OCTA data among the SSc cohort.
Methods: The enrolment included 35 SSc patients (mean age 61.1 ± 13.4 years, mean disease duration 9.5 ± 6 years) and 28 HCs in a single centre from March to October 2022.
The patients were classified according to the ACR/EULAR 2013 criteria, and multiple assessments were performed, at the same day, including ophthalmological examinations, OCTA, NVC and LASCA.
The clinical, laboratory and instrumental data of SSc patients were analysed and correlated with the OCTA data.
Patients were under standard treatment for SSc and those requiring endovenous prostanoids were evaluated for the study assessment at least one month after the last infusion.
Results: Among the ocular features, the intraocular pressure (IOP) was significantly higher in SSc than in HCs (p=0.006).
Despite the structural features in OCTA being similar, a significant difference was detected in all the perfusion variables, including the superficial vascular plexus (SVP), deep vascular plexus (DVP), and choriocapillaris (CC) (Table 1).
When patients were stratified according to the clinical extension of skin involvement, diffuse cutaneous SSc (dcSSc) patients showed a significantly reduced CC perfusion compared to limited cutaneous SSc (lcSSc) patients. Interestingly, the choroidal thickness (CT) in dcSSc was nearly twice that of lcSSc (p < 0.0001). The age and disease duration did not significantly differ among the two subgroups (respectively, p = 0.18 and p = 0.37).
In addition, the mean number of capillaries per linear mm at NVC and the mean peripheral perfusion assessed by LASCA at the level of 2nd to 5th fingertip were negatively correlated with the IOP (r = -0.30 and r = -0.36, both p < 0.01).
Finally, the mean capillary number at NVC was also positively correlated with the perfusion values of the SVP and DVP at OCTA (r = 0.3, p = 0.01 and r = 0.28, p = 0.01) and the mean peripheral perfusion detected by LASCA positively correlated with the DVP and CC perfusion (r = 0.29 and r = 0.28, both p = 0.01).
Conclusion: The higher IOP in all SSc patients might be in line with reported vascular abnormalities occurring in the optic nerve head [2].
The reduced capillary density and perfusion of the retina and choriocapillaris suggest an ocular microvascular impairment similarly to what is observed at the nailfold and fingertips in SSc patients.
The increased CT limited to dcSSc might be related to attempts of ocular microvascular reactivity and deposition of sub-endothelial extracellular matrix in agreement with the fibrotic process observed in other tissues in such patients.
References: [1] Kreps et al. Semin Arthr Rheum 2019. [2] Hysa et al. Aut Rev 2021

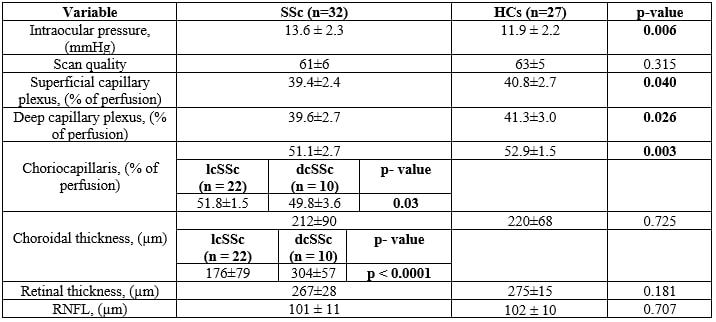
Table 1. Comparisons of ocular features and OCTA data between SSc and HCs.
Abbreviations. SSc: systemic sclerosis; HCs: healthy controls; lcSSc: localized cutaneous systemic sclerosis; dcSSc: diffuse cutaneous systemic sclerosis; RNFL= retinal nerve fiber layer.
Abbreviations. SSc: systemic sclerosis; HCs: healthy controls; lcSSc: localized cutaneous systemic sclerosis; dcSSc: diffuse cutaneous systemic sclerosis; RNFL= retinal nerve fiber layer.
C. Cutolo: None; E. Hysa: None; A. Cere: None; P. Toma: None; T. Cannavacciuolo: None; C. Toma: None; S. Balito: None; V. Gerli: None; A. Sulli: None; V. Smith: Boehringer Ingelheim, 2, 5, 6, 12, Support for travel, Galapagos, 6, Janssen-Cilag, 1, 2, 5, 6; C. Traverso: None; M. Nicolò: None; M. Cutolo: Amgen, 5, Boehringer Ingelheim, 5, Bristol-Myers Squibb, 5, Lab.Baldacci, 5.



