Poster Session A
Fibrosing rheumatic diseases (scleroderma, MCTD, IgG4-related disease, scleroderma mimics)
Session: (0609–0672) Systemic Sclerosis & Related Disorders – Clinical Poster I: Research
0641: The Evaluation of Lower Extremities Arterial Disease in Systemic Sclerosis Patients Through Rheumatologist-Vascular Surgeon Multidisciplinary Management: Preliminary Data from an Italian Single Center Study
Sunday, November 12, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- ML
Maria Grazia Lazzaroni, MD, PhD (she/her/hers)
ASST Spedali Civili di Brescia
Brescia, Brescia, ItalyDisclosure information not submitted.
Abstract Poster Presenter(s)
Maria Grazia Lazzaroni1, Liala Moschetti1, Eleonora Pedretti1, Paolo Baggi2, Franco Franceschini3, Stefano Bonardelli2 and Paolo Airò1, 1Rheumatology and Clinical Immunology, ASST Spedali Civili of Brescia, University of Brescia, Brescia, Italy, 2Vascular Surgery, ASST Spedali Civili di Brescia, University of Brescia, Brescia, Italy, 3Rheumatology and Clinical Immunology, ASST Spedali Civili of Brescia, Department of Clinical and Experimental Sciences, University of Brescia, Brescia, Italy
Background/Purpose: The occurrence of lower limbs macrovascular complications configuring lower extremities arterial disease (LEAD) has been reported in Systemic Sclerosis (SSc) patients. Recently, digital ulcers (DUs), pulmonary arterial hypertension (PAH), steroid use and active smoking/having stopped ≤3 years were identified as factors associated with lower limbs amputation in a single-centre SSc cohort1. Our aim was the estimation of LEAD prevalence in: (i) the overall SSc cohort and (ii) at-risk patients according to the above-mentioned features.
Methods: Consecutive SSc patients attending our centre for scheduled visits between October 2022 and April 2023 were included. Patients without known LEAD with ≥1 feature associated to lower limb amputation, as described above1 were referred for lower extremities arterial Doppler ultrasonography (DUS) performed by a single expert vascular surgeon.
Results: Among 192 SSc patients evaluated (93% females, 81% limited cutaneous involvement, 45% anti-centromere), 18 (9%) were previously diagnosed with LEAD, requiring revascularization interventions in 8 (44%) and amputations in 5 (28%). As compared to the remaining 174, they were older (median[1st-3rd quartile]: 75[69-79] vs 62[51-70] years; p< 0.001), had a longer disease duration (20[15-27] vs 12[6-19] years; p:0.004), higher frequency of DUs (90% vs 54%; p:0.001), especially at lower limbs (67% vs 12%; p< 0.001), more comorbidities (Charlson Comorbidity Index: 6[5-7] vs 3[2-5]; p< 0.001), and were more frequently treated with prostanoids (67% vs 31%; p:0.002) and steroids (61% vs 31%; p:0.010).
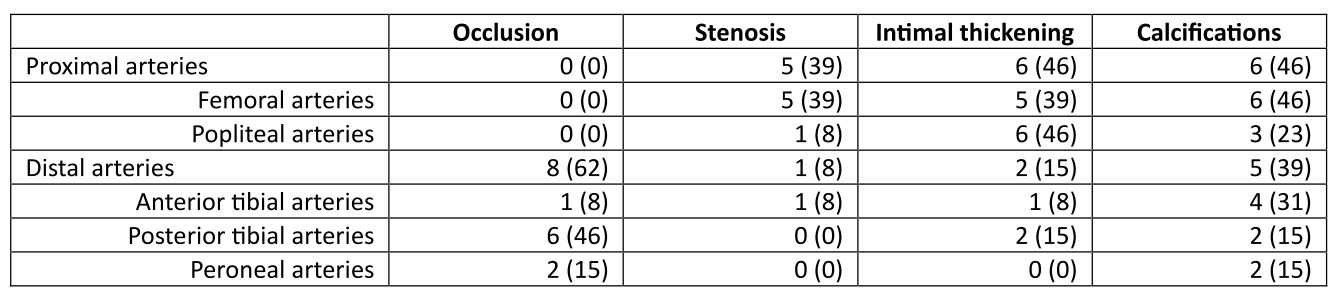
At least 1 LEAD risk factor was identified in 124/174 patients (71%) (DUs (77%); steroid use (40%); smoking (26%); PAH (5%)). Among 41 patients so far evaluated by DUS, LEAD was detected in 13 (32%) (Table 1): 10 were asymptomatic (stage I), 2 reported mild claudication (stage IIa), 1 reported pain also at rest (stage III). 10/13 were already on treatment with anti-platelets/anti-coagulants, in the remaining 3 patients low dose aspirin was added; the patient with LEAD stage III was referred to angiographic study. As compared to 28 patients with a normal DUS, no differences were observed in clinical-demographic features (Table 2).
Conclusion: Based on these preliminary data, in our SSc cohort the prevalence of diagnosed LEAD stands at 9%. However, by selecting at-risk SSc patients (DUs, PAH, steroid use and smoking), LEAD signs on DUS were detected in 32% of them, mostly free from lower limb symptoms and traditional CV risk-factors. This underlines the need to implement the diagnostic/therapeutic work-up of SSc patients by performing lower extremities arterial DUS and including vascular surgeons in the multidisciplinary team dedicated to SSc patients.
References. 1Bertolino et al. JSRD. 2020
The Authors would like to thank GILS Patient Association for kindly supporting this project.
M. Lazzaroni: None; L. Moschetti: None; E. Pedretti: None; P. Baggi: None; F. Franceschini: None; S. Bonardelli: None; P. Airò: None.
Background/Purpose: The occurrence of lower limbs macrovascular complications configuring lower extremities arterial disease (LEAD) has been reported in Systemic Sclerosis (SSc) patients. Recently, digital ulcers (DUs), pulmonary arterial hypertension (PAH), steroid use and active smoking/having stopped ≤3 years were identified as factors associated with lower limbs amputation in a single-centre SSc cohort1. Our aim was the estimation of LEAD prevalence in: (i) the overall SSc cohort and (ii) at-risk patients according to the above-mentioned features.
Methods: Consecutive SSc patients attending our centre for scheduled visits between October 2022 and April 2023 were included. Patients without known LEAD with ≥1 feature associated to lower limb amputation, as described above1 were referred for lower extremities arterial Doppler ultrasonography (DUS) performed by a single expert vascular surgeon.
Results: Among 192 SSc patients evaluated (93% females, 81% limited cutaneous involvement, 45% anti-centromere), 18 (9%) were previously diagnosed with LEAD, requiring revascularization interventions in 8 (44%) and amputations in 5 (28%). As compared to the remaining 174, they were older (median[1st-3rd quartile]: 75[69-79] vs 62[51-70] years; p< 0.001), had a longer disease duration (20[15-27] vs 12[6-19] years; p:0.004), higher frequency of DUs (90% vs 54%; p:0.001), especially at lower limbs (67% vs 12%; p< 0.001), more comorbidities (Charlson Comorbidity Index: 6[5-7] vs 3[2-5]; p< 0.001), and were more frequently treated with prostanoids (67% vs 31%; p:0.002) and steroids (61% vs 31%; p:0.010).
At least 1 LEAD risk factor was identified in 124/174 patients (71%) (DUs (77%); steroid use (40%); smoking (26%); PAH (5%)). Among 41 patients so far evaluated by DUS, LEAD was detected in 13 (32%) (Table 1): 10 were asymptomatic (stage I), 2 reported mild claudication (stage IIa), 1 reported pain also at rest (stage III). 10/13 were already on treatment with anti-platelets/anti-coagulants, in the remaining 3 patients low dose aspirin was added; the patient with LEAD stage III was referred to angiographic study. As compared to 28 patients with a normal DUS, no differences were observed in clinical-demographic features (Table 2).
Conclusion: Based on these preliminary data, in our SSc cohort the prevalence of diagnosed LEAD stands at 9%. However, by selecting at-risk SSc patients (DUs, PAH, steroid use and smoking), LEAD signs on DUS were detected in 32% of them, mostly free from lower limb symptoms and traditional CV risk-factors. This underlines the need to implement the diagnostic/therapeutic work-up of SSc patients by performing lower extremities arterial DUS and including vascular surgeons in the multidisciplinary team dedicated to SSc patients.
References. 1Bertolino et al. JSRD. 2020
The Authors would like to thank GILS Patient Association for kindly supporting this project.

Table 1. Characterization of LEAD findings on DUS in 13 patients. Variables are expressed as n (%).

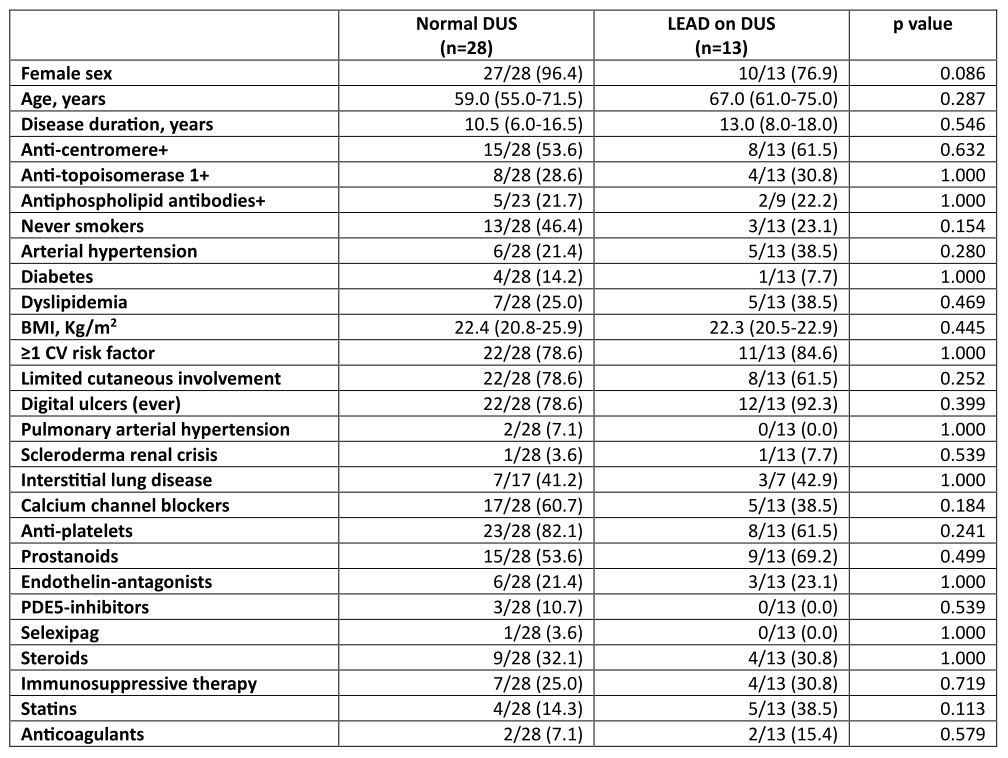
Table 2. Comparison of demographic, clinical-therapeutic features and CV risk factors in patients with LEAD on DUS vs patients with normal DUS. Categorical variables are expressed as n (%) and compared with Chi Squared/Fisher exact test; continuous variables are expressed as median (1st-3rd quartile) and compared with Mann Whitney test.
Abbreviations: BMI= Body Mass Index, CV= cardiovascular, PDE5= phosphodiesterase 5.
Abbreviations: BMI= Body Mass Index, CV= cardiovascular, PDE5= phosphodiesterase 5.
M. Lazzaroni: None; L. Moschetti: None; E. Pedretti: None; P. Baggi: None; F. Franceschini: None; S. Bonardelli: None; P. Airò: None.



