Poster Session A
Immunobiology
Session: (0066–0095) T Cell Biology & Targets in Autoimmune & Inflammatory Disease Poster
0073: PD-1hi Cells Are Highly Present in the Rheumatoid Joint, and Express Regulatory Capacities
Sunday, November 12, 2023
9:00 AM - 11:00 AM PT
Location: Poster Hall
- SG
Stinne Greisen, PhD
Aarhus University/Aarhus University Hospital
Aarhus, DenmarkDisclosure information not submitted.
Abstract Poster Presenter(s)
Sofie Rask1, Christian Andersen2, Malene Hvid1, Kim Ravnskjær2, Bent Deleuran1 and Stinne Greisen3, 1Aarhus University, Aarhus, Denmark, 2University of Southern Denmark, Odense, Denmark, 3Aarhus University/Aarhus University Hospital, Aarhus, Denmark
Background/Purpose: Programmed death 1 (PD-1) is an immune checkpoint receptor expressed by activated T cells, and of major importance in maintaining peripheral tolerance. Expression of PD-1 has been associated with T cells exhaustion, plasma cell differentiation and bone homeostasis. With emerging treatments engaging the PD-1 pathway in Rheumatoid Arthritis (RA) this pathway is of continued interest.
We aimed to investigate PD-1hi T cells from RA synovial fluid (SF).
Methods: SF was collected from RA patients with disease flare (n=7). Cells were stained for flow and sorted in CD3+ PD-1hi/PD-1lo populations. Post sorting, bulk RNA seq was performed, and cells were stimulated with antiCD3/CD28. Cytokines in the supernatants were investigated using V-plex multipanel assay. Supernatants were added to fibroblast cultures and the osteoblast cell line SaOs-2.
Results: Evaluated by flow cytometry, PD-1+ cells represented 42% of CD4+ T cells and 34% of CD8+ T cells in the SF. When comparing co-expression of checkpoint receptors and transcription factors between PD-1hi and PD-1lo CD4+ T cell; Tigit, Tim3 and NFAT were all increased in PD-1hi (all p < 0.05), Lag-3 was slightly elevated (p=0.07), whereas TCF1 and TOX expression did not differ. These differences were not observed between PD-1hi and PD-1lo CD8+ T cells.
Post sorting, RNAseq revealed PD-1hi and PD-1lo cells to cluster separately. In PD-1hi cells, gene expression corresponded to structural signatures, including tubulin binding and cytoskeletal motor activity (p < 0.01). Genes related to peripheral T helper cells, including IL21 and CXCL13 were highly upregulated (all p< 0.05) The gene PHEX was highly expressed (log2 fold change=5.2), suggesting an association with bone mineralization. The signature in PD-1lo cells was associated with immune activation genes (p < 0.005). Stimulating cells with CD3/CD28 post sorting resulted in lower production of IL-2, IFNg, TNFa, IL-8, IL-10, IL-13, IL-12, and IL-1b from PD-1hi cells compared to PD-1lo. The supernatant from PD-1hi cells only slightly activated fibroblasts, whereas the PD-1lo supernatant significantly activated fibroblasts, as measured by by MCP-1 production and surface ICAM expression (fig 1). When adding the PD-1hi and PD-1lo supernatant to osteoblast cultures, bone mineralization was significantly increased by the PD-1hi supernatant (fig 2).
Conclusion: PD-1hi cells are present in the synovial joint. They are not exhausted but express multiple checkpoint receptors, suggesting regulatory capacities. They could play a central role in structural maintenance through effects on fibroblasts and osteoblasts.
.gif)
S. Rask: None; C. Andersen: None; M. Hvid: None; K. Ravnskjær: Thermo Fisher, 3; B. Deleuran: None; S. Greisen: None.
Background/Purpose: Programmed death 1 (PD-1) is an immune checkpoint receptor expressed by activated T cells, and of major importance in maintaining peripheral tolerance. Expression of PD-1 has been associated with T cells exhaustion, plasma cell differentiation and bone homeostasis. With emerging treatments engaging the PD-1 pathway in Rheumatoid Arthritis (RA) this pathway is of continued interest.
We aimed to investigate PD-1hi T cells from RA synovial fluid (SF).
Methods: SF was collected from RA patients with disease flare (n=7). Cells were stained for flow and sorted in CD3+ PD-1hi/PD-1lo populations. Post sorting, bulk RNA seq was performed, and cells were stimulated with antiCD3/CD28. Cytokines in the supernatants were investigated using V-plex multipanel assay. Supernatants were added to fibroblast cultures and the osteoblast cell line SaOs-2.
Results: Evaluated by flow cytometry, PD-1+ cells represented 42% of CD4+ T cells and 34% of CD8+ T cells in the SF. When comparing co-expression of checkpoint receptors and transcription factors between PD-1hi and PD-1lo CD4+ T cell; Tigit, Tim3 and NFAT were all increased in PD-1hi (all p < 0.05), Lag-3 was slightly elevated (p=0.07), whereas TCF1 and TOX expression did not differ. These differences were not observed between PD-1hi and PD-1lo CD8+ T cells.
Post sorting, RNAseq revealed PD-1hi and PD-1lo cells to cluster separately. In PD-1hi cells, gene expression corresponded to structural signatures, including tubulin binding and cytoskeletal motor activity (p < 0.01). Genes related to peripheral T helper cells, including IL21 and CXCL13 were highly upregulated (all p< 0.05) The gene PHEX was highly expressed (log2 fold change=5.2), suggesting an association with bone mineralization. The signature in PD-1lo cells was associated with immune activation genes (p < 0.005). Stimulating cells with CD3/CD28 post sorting resulted in lower production of IL-2, IFNg, TNFa, IL-8, IL-10, IL-13, IL-12, and IL-1b from PD-1hi cells compared to PD-1lo. The supernatant from PD-1hi cells only slightly activated fibroblasts, whereas the PD-1lo supernatant significantly activated fibroblasts, as measured by by MCP-1 production and surface ICAM expression (fig 1). When adding the PD-1hi and PD-1lo supernatant to osteoblast cultures, bone mineralization was significantly increased by the PD-1hi supernatant (fig 2).
Conclusion: PD-1hi cells are present in the synovial joint. They are not exhausted but express multiple checkpoint receptors, suggesting regulatory capacities. They could play a central role in structural maintenance through effects on fibroblasts and osteoblasts.
.gif)
Fig 1: Left: Expression of ICAM on fibroblasts after culturing with PD-1 hi/PD-1lo supernatant. IFNg used as a positive control. Right: MCP-1 production measured in the supernatant from fibroblasts after culturing with PD-1 hi/PD-1lo supernatant. IFNg used as a positive control.

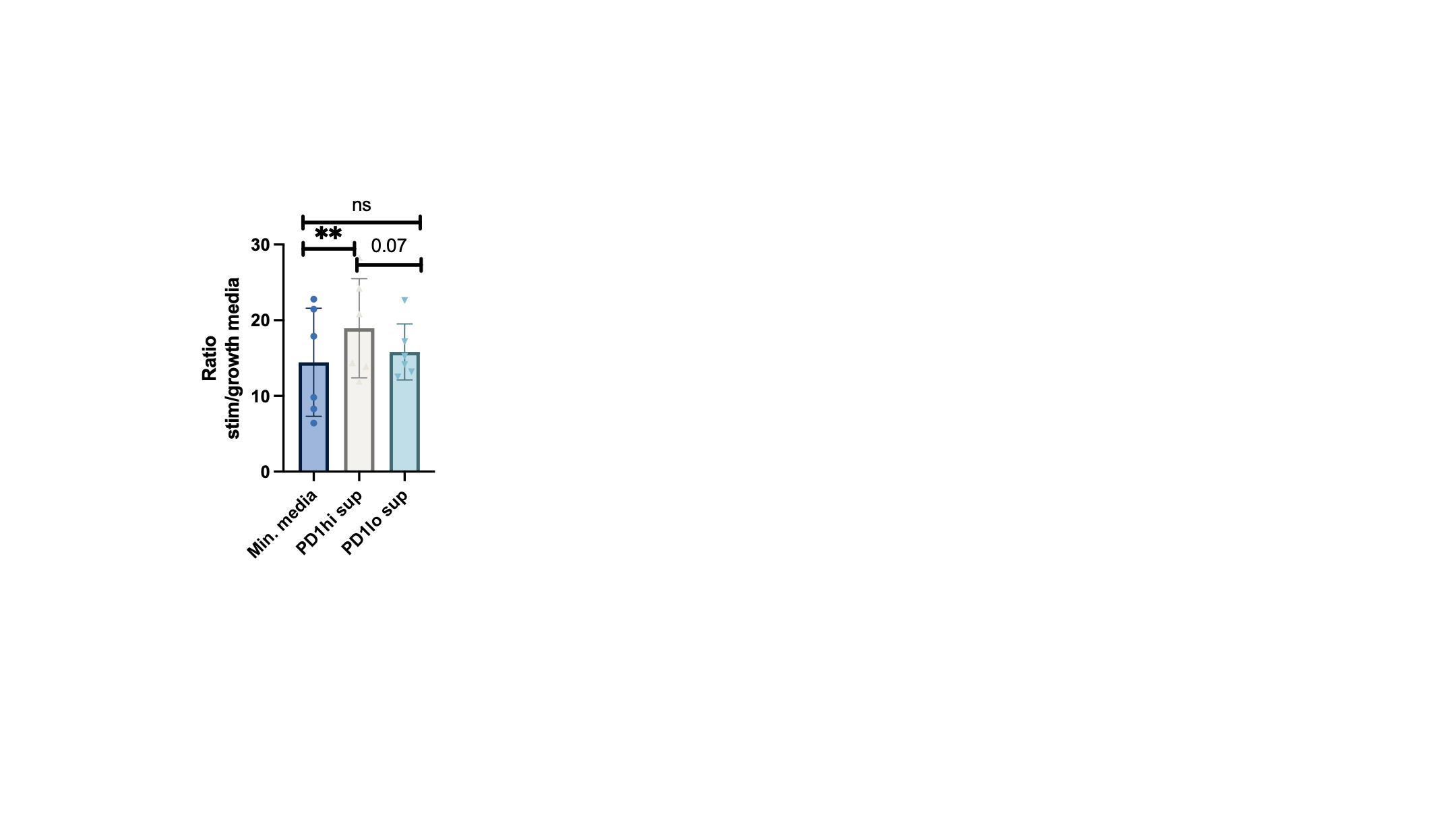
Mineralization measured in the SaOs-2 osteoblast cell line after culturing with PD-1hi and PD-1lo supernatant. Data are normalized to the cell line in growth media.
S. Rask: None; C. Andersen: None; M. Hvid: None; K. Ravnskjær: Thermo Fisher, 3; B. Deleuran: None; S. Greisen: None.



