Abstract Session
Crystal arthropathies
Session: Abstracts: Metabolic & Crystal Arthropathies – Basic & Clinical Science (0811–0816)
0816: Additive Association of ABCG2 rs4148155 and SLC22A12 rs75786299 Polymorphisms with Hyperuricemia, Gout and Nephrolithiasis, a Hospital-Based, Case-Control Study
Sunday, November 12, 2023
5:15 PM - 5:25 PM PT
Location: Room 25A-C
- CL
Ching-Tsai Lin, MD
Taichung Veterans General Hospital
Taichung, TaiwanDisclosure information not submitted.
Presenting Author(s)
Ching-Tsai Lin1, I-Chieh Chen2, Wen-Nan Huang1, Yi-Hsing Chen1, Ching-Heng Lin2 and Yi-Ming Chen1, 1Taichung Veterans General Hospital, Taichung, Taiwan, 2Department of Medical Research, Taichung Veterans General Hospital, Taichung, Taiwan
Background/Purpose: This study aimed to investigate the interaction between the ABCG2 rs4148155 and SLC22A12 rs75786299 variants and their association with incident gout and nephrolithiasis in the Taiwanese population to better understand the genetic loci regulating hyperuricemia and their contribution to nephrolithiasis development.
Methods: This retrospective case-control study involved 35,280 adults from the Taiwan Precise Medicine Initiative (TPMI) database. We examined the prevalence of gout and ultrasound confirmed nephrolithiasis as the primary and secondary outcome. Univariable and multivariable logistic regression models were used to explore the associations between genetic variants, serum uric acid levels, incident gout, and nephrolithiasis.
Results: The frequencies of the rs4148155 G allele and the rs75786299 A allele was 33% and 2.4%, respectively. Among participants, 7,056 were gout, and 4,110 had nephrolithiasis. Multivariable odds ratios (ORs) for gout were 1.65 (1.56-1.75) and 3.59 (2.92-4.41) among one and two carriers, respectively (p=0.01 and p< 0.001). For nephrolithiasis, the multivariable ORs were 1.09 (1.02-1.17) and 1.40 (1.09-1.81) for one and two carriers, respectively (p=0.01 and p=0.009). Sex-stratified analysis revealed an additive risk of gout and nephrolithiasis among carriers of these genetic variants, regardless of gender. Independent risk factors for nephrolithiasis included higher age, male gender, and the presence of gout, hypertension, and hyperlipidemia.
Conclusion: The study highlights a significant association between the rs4148155 (G) and rs75786299 (A) alleles and the development of gout and nephrolithiasis, indicating an additive risk among carriers. These findings support precision healthcare approaches for individuals with these genetic variants to target hyperuricemia, gout, and systemic comorbidities, ultimately preventing nephrolithiasis.
.jpg)
C. Lin: None; I. Chen: None; W. Huang: None; Y. Chen: None; C. Lin: None; Y. Chen: None.
Background/Purpose: This study aimed to investigate the interaction between the ABCG2 rs4148155 and SLC22A12 rs75786299 variants and their association with incident gout and nephrolithiasis in the Taiwanese population to better understand the genetic loci regulating hyperuricemia and their contribution to nephrolithiasis development.
Methods: This retrospective case-control study involved 35,280 adults from the Taiwan Precise Medicine Initiative (TPMI) database. We examined the prevalence of gout and ultrasound confirmed nephrolithiasis as the primary and secondary outcome. Univariable and multivariable logistic regression models were used to explore the associations between genetic variants, serum uric acid levels, incident gout, and nephrolithiasis.
Results: The frequencies of the rs4148155 G allele and the rs75786299 A allele was 33% and 2.4%, respectively. Among participants, 7,056 were gout, and 4,110 had nephrolithiasis. Multivariable odds ratios (ORs) for gout were 1.65 (1.56-1.75) and 3.59 (2.92-4.41) among one and two carriers, respectively (p=0.01 and p< 0.001). For nephrolithiasis, the multivariable ORs were 1.09 (1.02-1.17) and 1.40 (1.09-1.81) for one and two carriers, respectively (p=0.01 and p=0.009). Sex-stratified analysis revealed an additive risk of gout and nephrolithiasis among carriers of these genetic variants, regardless of gender. Independent risk factors for nephrolithiasis included higher age, male gender, and the presence of gout, hypertension, and hyperlipidemia.
Conclusion: The study highlights a significant association between the rs4148155 (G) and rs75786299 (A) alleles and the development of gout and nephrolithiasis, indicating an additive risk among carriers. These findings support precision healthcare approaches for individuals with these genetic variants to target hyperuricemia, gout, and systemic comorbidities, ultimately preventing nephrolithiasis.

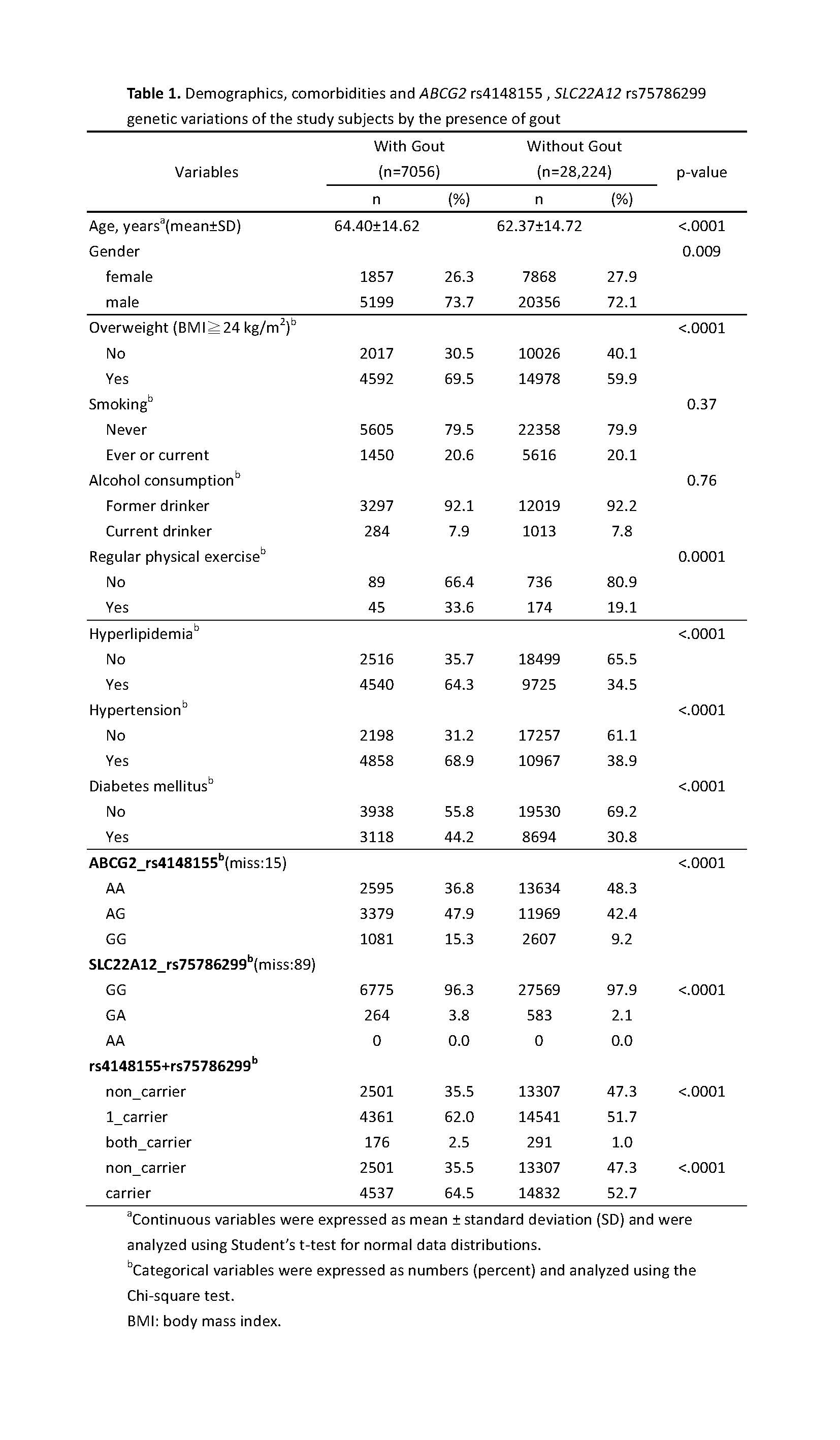
Table 1. Demographics, comorbidities and ABCG2 rs4148155 , SLC22A12 rs75786299 genetic variations of the study subjects by the presence of gout
.jpg)
Table 2. Association of ABCG2 rs4148155 , SLC22A12 rs75786299 alleles, hyperuricemia gout and nephrolithiasis with sex stratification

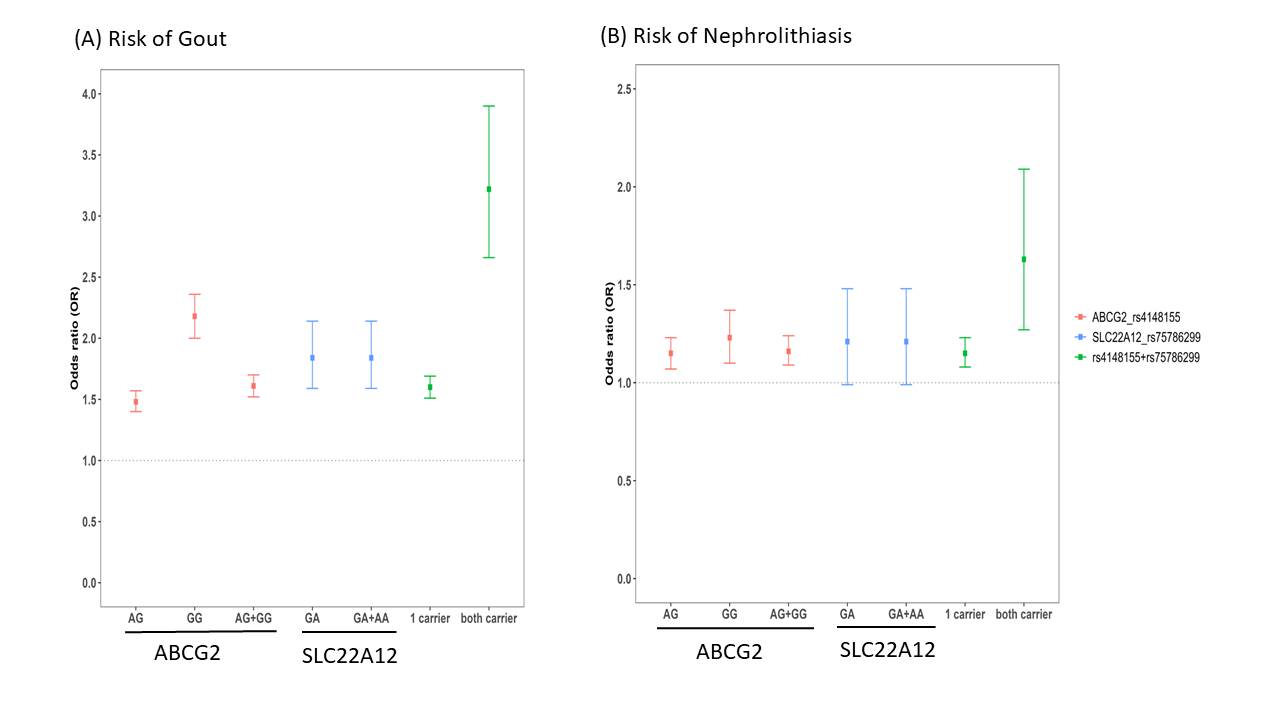
Figure 1 Risk of gout (A) and nephrolithiasis (B) among the carriers of ABCG2 rs4148155, SLC22A12 rs75786299 genotypic variants. Error bars represent the 95% confidence intervals (CI) of the odds ratios (ORs). (A) The univariable ORs (95% confidence intervals [CI] and p-values) for ABCG2 rs4148155 GG, AG, and AG+GG compared to the AA genotype were 2.18 (2.00-2.36, p<0.0001), 1.48, (1.4-1.57, p<0.0001), 1.61, (1.52-1.70, p<0.0001) and for SLC22A12 rs75786299 GA was 1.84 (1.59-2.14, p<0.0001) polymorphisms which were significantly associated with gout risk, respectively. Furthermore, under an additive model of inheritance, one and two carriers of ABCG2 rs4148155 (G) and SLC22A12 rs75786299 (A) remained independently associated with gout (OR = 1.60, 95% CI 1.51-1.69, p<0.0001; and OR = 3.22, 95% CI 2.66-3.90, p<0.0001, respectively). (B). The univariable ORs for the rs4148155 AG, GG, and AG+GG genotypes compared to the AA genotype were 1.15 (1.07–1.23, p=0.0001), 1.23 (1.10–1.37, p=0.0002), and 1.16 (1.06–1.24, p<0.0001), which were significantly associated with risk of nephrolithiasis respectively. In addition, the ORs for incident nephrolithiasis in individuals carrying one and two copies of the ABCG2 rs4148155(G) and SLC22A12 rs75786299(A) genotypic variants were 1.15 (1.08–1.23, p<0.0001) and 1.63 (1.27–2.09, p=0.0001).
C. Lin: None; I. Chen: None; W. Huang: None; Y. Chen: None; C. Lin: None; Y. Chen: None.



